The publication of the National Cooperative Dialysis Study was a seminal moment in the history of Nephrology. It was on the basis of this RCT that dialysis time was deemed not to be an important predictor of outcomes (based on a p-value of 0.056), and the love affair with Kt/V(urea) effectively began. Nowadays, although Kt/V(urea) targets are slavishly met, hemodialysis patients continue to experience high rates of complications such as hypertension, LVH, CHF, hyperphosphatemia, malnutrition and death. Set this against the superior outcomes seen with longer treatments such as nocturnal HD, and you begin to wonder if they may be onto something in Tassin. There, longer dialysis times aren’t just instituted for their own sake; they permit the attainment of target dry weights that are almost impossible to reach in a shorter session i.e. it’s not the time that’s important, it’s what you do with it that matters. Here I’ll present some of their clinical pearls for achieving DW based on several review articles they have written on the subject:
First, a clinically meaningful definition of DW: “that body weight at the end of dialysis at which the patient can remain normotensive without antihypertensive medication, despite fluid accumulation, until the next dialysis.”
- At DW, a patient’s BP should remain in the normal range during the entire interdialytic period. If BP remains high after dialysis or is elevated before the next session, they are, by definition, above their DW.
- Dialysis session times of 5-6 hours are usually required, particularly when determining the DW for the first time. Trying to achieve the necessary ultrafiltration over a shorter time will cause hypotension and cramping, and lead to treatment failure.
- Go slowly! It takes 2-3 months to achieve DW in a new dialysis patient. During this time carefully controlled persistent UF and a strict low salt diet are used, while antihypertensive medications are weaned off entirely.
- It is essential that all BP medications be tapered down and stopped early in the process. Otherwise it will be impossible to achieve DW.
- Hypotension and cramping will often occur when nearing DW, and are a common cause of treatment failure. These symptoms do not indicate a patient has reached DW, rather the patient has hit their max refill capacity (Crit. lines predict hypotensive episodes, but do not assess dry weight for the same reasons). If a patient remains hypertensive while experiencing such symptoms, longer dialysis times are indicated to achieve UF goals.
- Be aware of the “lag phenomenon”. BP does not immediately change in response to changes in volume. Blood pressure may only normalize a few weeks after ECV has returned to normal.
- Do not wait for obvious signs of volume overload (oedema, hypertension, etc.). Pay attention to small signs such as headache or slight increase BP at the end of a session.
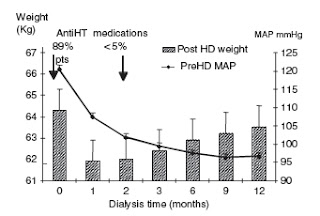
- Weight falls rapidly after initiating dialysis due to saline removal. However, as a rule of thumb, weight should return to pre-initiation levels after 1 year on dialysis due to muscle and fat build up, with BP now under control (see figure).
- In difficult cases, ambulatory blood pressure monitoring is an invaluable tool, as it gives the best estimate of the ‘true’ interdialytic BP (see point 1).



Most of the recent accounts of superior dialysis outcomes deal with frequency and duration.
It is a true anomaly in modern medicine to have an entire sub-specialty with actually worsening outcomes and such a vast gulf between "typical" vs. "achievable."
Kt/V has *failed* to improve outcomes. It has been given a LONG and fair chance to do so. It is time to accept this fact. Sometimes widely held prevailing wisdom can be wrong. Dialysis time does matter. Patients feeling better does matter, regardless whether their laboratory values are in "acceptable" ranges. "Washout" isn't just how a patient "feels"–it is a reflection of physiological shock they must endure. It is debilitating yet we routinely accept it because we "followed proper procedure."
What has happened to the clinician's common sense and compassion in this regard?
When such dramatically better outcomes such as Tassin are demonstrated to be possible the argument that "we don't know how" (to do better) rings false. Look at successful examples and use these as the starting point to begin creating better standards and raise the bar of what you are personally willing to accept.
Label it "resource issues" if you like, but
ultimately, nephrologists themselves must begin take personal responsibility to strive the best outcomes for their patients–even if it means hurting the bottom line. The potential for moral abuse of CMS bundled payment is great. Rise above it even if your colleagues will not.
Hopefully this truly outstanding RFN blog will help foster a new generation who will do better than the previous. At least emerging issues get discussed, but it is past time to take a hard, HONEST look at Kt/V's limitations in order to get out of this 30-year rut. Kt/V started out as a minimum acceptable standard which was subsequently forgotten. Tell your patients you are trying to give them "minimum acceptable" care and watch them head for the door.
Agreed, empirically-derived dialysis times in the late 1960's were 8 hours, 3 times a week. Although times were brought down elsewhere due to resource issues and in the light of Kt/V, they remained of this length in Tassin.
Nisha: Regarding diet / sodium intake, patients maintain a reasonably low salt diet. The effective average sodium chloride intake is 5 g per day and mean interdialytic weight gain is 1.8 kg (2.6% of
mean dry weight). The dialysate sodium is set at 138 mmol/l and patients are not requested to restrain from drinking.
Thanks for your feedback and support of the site.
Any mentions on differences in diet in this part of France as compared to the typical American diet? I often hear comparisons from international friends, about how, for example, in England they do not have as large of interdialytic weight gains, and I often wonder if it is due to a difference in sodium content in food and typical fluid intake in our dialysis patients compared to theirs.
Thanks, Nisha
The sad little secret about Tassin is that this group kept the original dialysis schedule developed during the 1960's all the way through till today. There was nothing secret about their work, they published several papers in the 80's and 90's that were over looked until recently.