Ultrasonography of the kidneys is one of the most common imaging modalities performed in children in the nephrology clinic. The routine use of prenatal ultrasound in pregnancy care has additionally provided nephrologists with a view into the kidneys and urinary tract as they develop in utero, allowing both families and care teams to prepare for complications related to the kidney that may arise after birth. Increased echogenicity of the kidneys, while non-specific, is one of the most common imaging findings on kidney ultrasound; it may be a transient finding, or a harbinger of serious kidney disease that warrants evaluation by a pediatric nephrologist.
The echogenicity of a kidney, or any organ for that matter, refers to how bright it appears on grayscale imaging by ultrasound. These images are produced when the ultrasound machine operates in two-dimensional brightness mode (B-mode), in which reflected echoes appear as bright dots. Tissue that most strongly reflects sound waves is hyperechoic and appears white (e.g. fibrous and adipose tissue), whereas fluid, such as from simple cysts or urine in the collecting system, reflects the weakest (anechoic) and appears black in color. Traditionally, the brightness of the kidneys on ultrasound has been described in relation to that of the liver, which has intermediate echogenicity, and is used as an internal comparison (so long as there isn’t liver pathology present, such as fatty liver disease).
Figure 1. Normal appearing kidney. On ultrasound, the kidney (white arrowhead) is hypoechoic in comparison to the liver (white arrow). Though slightly difficult to appreciate on this view, there is good corticomedullary differentiation with visualization of medullary pyramids (asterisks). The central hyperechoic area of the kidney is the renal sinus. Image source: Wikimedia.
Normal kidneys in children appear hypoechoic to the liver on ultrasound imaging, with the kidney cortex having a relative increase in brightness compared to the medullary pyramids. The kidneys of neonates commonly appear isoechoic, but typically by 6 months of age the appearance of the kidneys resembles that of older children and adults. Preterm neonates are an exception, as they may have kidneys that are hyperechoic on ultrasound and may be a normal variant. Neonatal kidneys may also have a transient increased echogenicity of the medullary pyramids in particular, that resolves by 2 weeks of life. The etiology remains unclear, but may be due to increased Tamm-Horsfall protein concentration in the renal tubules.
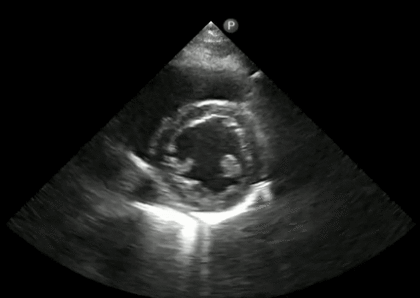
Figure 2. The neonatal kidney. On ultrasound, the kidney cortex (white arrowhead) is isoechoic in comparison to the liver (white arrow). There is increased corticomedullary differentiation with clear visualization of the medullary pyramids (asterisks), a common finding in normal neonatal kidneys. Image source: Anonymous.
Though there is some normal perinatal variation in the echotexture of the kidneys, prenatal and neonatal kidneys that have increased echogenicity should always be assessed for pathology that may suggest kidney disease, including congenital anomalies of the kidneys and urinary tract (CAKUT).
- Determine whether the echogenicity is patchy (e.g. dysplasia) or diffuse (e.g. ARPKD)
- Its location within the kidney
- Is it primarily cortical (e.g. acute tubular necrosis)
- medullary (e.g. nephrocalcinosis)?
- Normal medullary pyramids should always be hypoechoic in comparison to the cortex, regardless of how bright the cortex appears in imaging.
Next, pay particular attention to the size of the kidneys. Enlarged echogenic kidneys in utero are a common prenatal finding in polycystic kidney disease, even before macrocysts becomes visible on ultrasound. Making note of the amniotic fluid volume is important, as concomitant oligohydramnios or anhydramnios portends poor long-term kidney function, increased risk for pulmonary hypoplasia, and decreased postnatal survival. The degree of urinary tract dilatation should be assessed if present, as this may suggest obstructive uropathy with associated renal cystic dysplastic changes. The presence of other congenital abnormalities on fetal imaging may be strongly suggestive of an underlying genetic syndrome.Echogenic kidneys presenting during later in childhood or adolescence, particularly if the size of the kidneys is normal or enlarged for age, is more likely from acquired kidney disease, such as glomerular disorders (e.g. FSGS), AKI from multiple causes, pyelonephritis (current infection or old kidney scars), and infiltrative diseases. Small, echogenic kidneys will also commonly have poor corticomedullary differentiation and may be seen from long standing undiagnosed kidney disease of many causes that have led to advanced CKD. An incidental finding of echogenic kidneys in this setting should be followed up with appropriate assessment of kidney function, including blood pressure measurement, serum electrolytes, BUN, creatinine, calcium, phosphorus, urinalysis, and screening for other CKD sequelae such as anemia and secondary hyperparathyroidism.
Table 1. Examples of conditions associated with increased kidney echogenicity in children. Note that there may be variations in kidney size observed for certain conditions. Sources: Krensky et al 1983, Kraus et al 1990, Chaumoitre et al 2006, Bullo et al 2012, and Faubel et al 2014.
To complicate matters, increased echogenicity of the kidneys may also be a transient finding in the absence of other signs of kidney disease. Some studies have suggested that an increased state of hydration in adults as well as children, without underlying kidney disease, may influence kidney cortical echogenicity. In a study by Wiersma et al., 189 consecutive children who presented with acute abdominal pain were imaged with ultrasonography, and 10% had hyperechoic kidneys and 8% had isoechoic kidneys in comparison to the liver. Amongst the clinical diagnoses, acute appendicitis in particular was most closely associated with abnormal kidney ultrasonography, with 31% of patients with acute appendicitis having increased renal cortical echogenicity. Though only 50% of children with increased echogenicity reportedly had serum creatinine measurement and 67% had urinalysis performed (data not reported), the finding of increased kidney cortical echogenicity resolved in all re-examined children 2 weeks after initial ultrasonography. Incidentally found echogenic kidneys during an acute illness, when kidney function is normal, warrants repeat imaging to assess whether this abnormality has resolved.
Next time you read a kidney ultrasound report that states “increased echogenicity of the kidneys consistent with medical renal disease,” you’ll be able to interpret the images yourself and assess for possible causes of this non-specific finding. Describe the pattern of increased echogenicity (cortical, medullary, or both), size of the kidneys (small, normal, or enlarged when considering the patient’s age), and the clinical context to determine why the kidneys are echogenic in the first place.
Post by
Brian Stotter, MD


Fantastic Review Dr. Brian Stotter. I met you in Boston Children´s Last year. I´m Edgar Barajas from Mexico City.
Farewell and best regards. Thank´s for the post.