Dear all,
It’s happening – Advances in Chronic Kidney Disease (ACKD) is taking a deep dive into the adult nephrology workforce in the United States. This issue (11 articles!) highlights the diverse aspects of and opportunities for a career in adult nephrology.
This series is a compilation of manuscripts from a group of diverse nephrologists and has been edited by RFN co-faculty leads Samira Farouk, MD, MS and Matthew Sparks, MD. Here’s their introductory editorial titled: “Reenvisioning the Adult Nephrology Workforce: The Future of Kidney Care in the United States.” In addition, ACKD Editor-in-Chief Charuhas Thakar, MD wrote an editorial here.
Below is a list of the articles in this issues as well as an accompanying brief summary and visual abstract. These visual abstracts are the work of: Sophia L Ambruso, DO, Michelle Lim, MBChC MRCP, Denisse Arellano, MD, Priti Meena, MD, Corina Teodosiu, MD, and Tiffany Truong, DO.
Several of the articles discuss opportunities for fellows to further sub-specialize. Natasha Dave, MD and Ankur Shah, MD have collated these in a searchable table here.
PDFs of all articles in this issue are available here.
Have any comments or suggestions? Let us know.
Enjoy and #NephForward!
The RFN Editorial Team
1. Redefining the Nephrology Workforce (Lederer ED & Lebowitz J)
2. Reinvigorating Nephrology Training (Shaikh A, et al.)
3. International Medical Graduates in Nephrology (Neyra J, et al.)
4. Research in Nephrology (Rangarajan S & Agarwal A)
5. Nephrology Clinician Educator (Roberts JK, et al.)
6. Sub-Specialization in Nephrology (Sachdeva M, et al.)
7. Critical Care Nephrology (Zeidman AD, et al.)
8. Transplant Nephrology Workforce (Concepcion BP, et al.)
9. Interventional Nephrology (Niyyar VD & Beathard G)
10. Palliative Care in Nephrology (Gelfand S, et al.)
11. Private Practice Nephrology (Agha I, et al.)
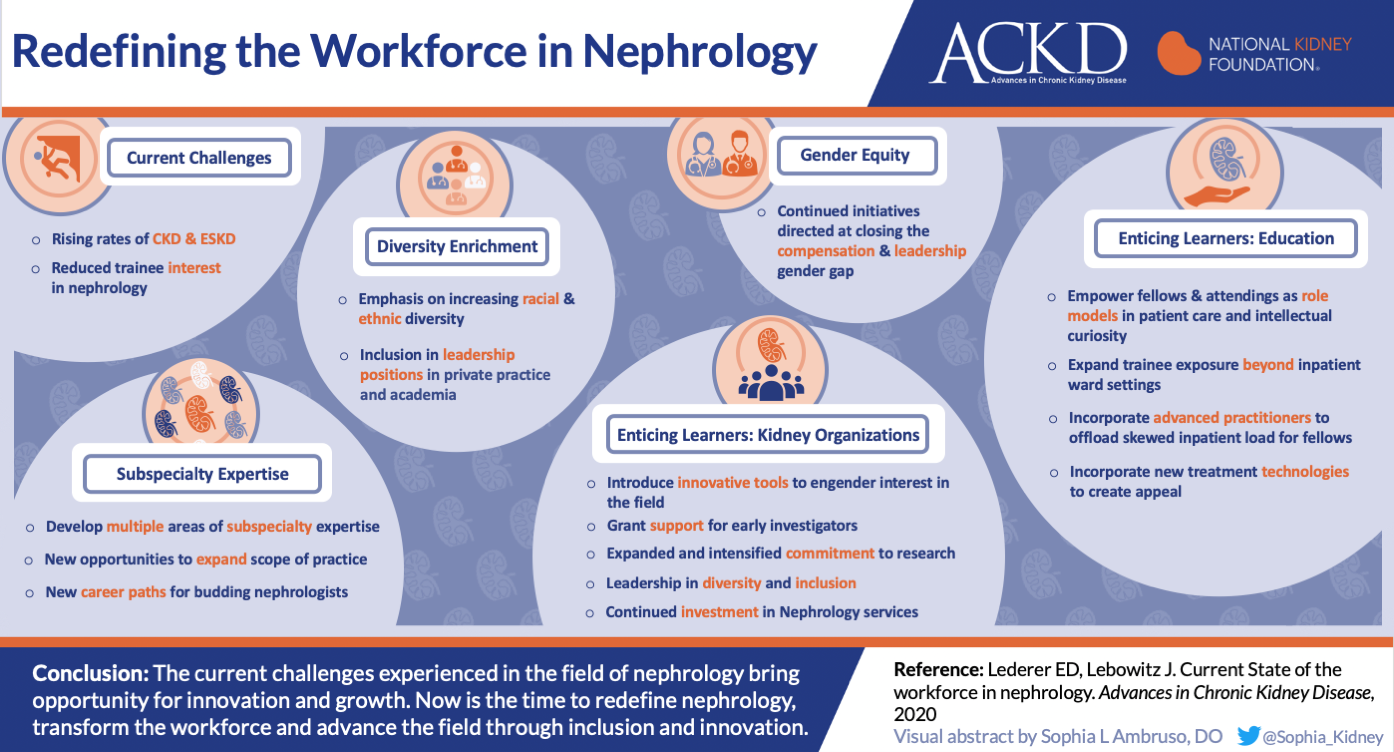
1. Redefining the Nephrology Workforce
The first article from Dr. Eleanor Lederer and Dr. Jonathan Lebowitz provides an overview of the workforce, discusses current challenges, and outlines strategies to increase diversity and ensure gender equity. The article also provides data from fellowship programs on how inpatient services are structured in regards to patient numbers, learner mix, and advanced practice provider usage. Finally, solutions are proposed to overcome the various challenges facing the nephrology community.
2. Reinvigorating Nephrology Training
Dr. Shaikh and colleagues review all aspects of nephrology education from medical school to fellowship to beyond. The authors first review the current landscape, discuss how exposures early in ones career can create both true and false perceptions of the field. Several innovations aimed to stimulate interest in nephrology are discussed. Novel paradigms in fellowship training are reviewed. Finally, the authors examine what steps are currently in place to reinvigorate the field of nephrology and enhance educational opportunities.
3. International Medical Graduates in Nephrology
International medical graduates (IMGs) make up a substantial proportion of trainees and attending nephrologists in the United States. Navigating the complex system of visas and immigration is daunting and filled with many challenges and roadblocks. Dr. Neyra et al provide a guide for both IMGs and programs to ensure success of each trainee. Listen to the National Kidney Foundation (NKF) Life as a Nephrologist podcast to hear directly from the authors here.
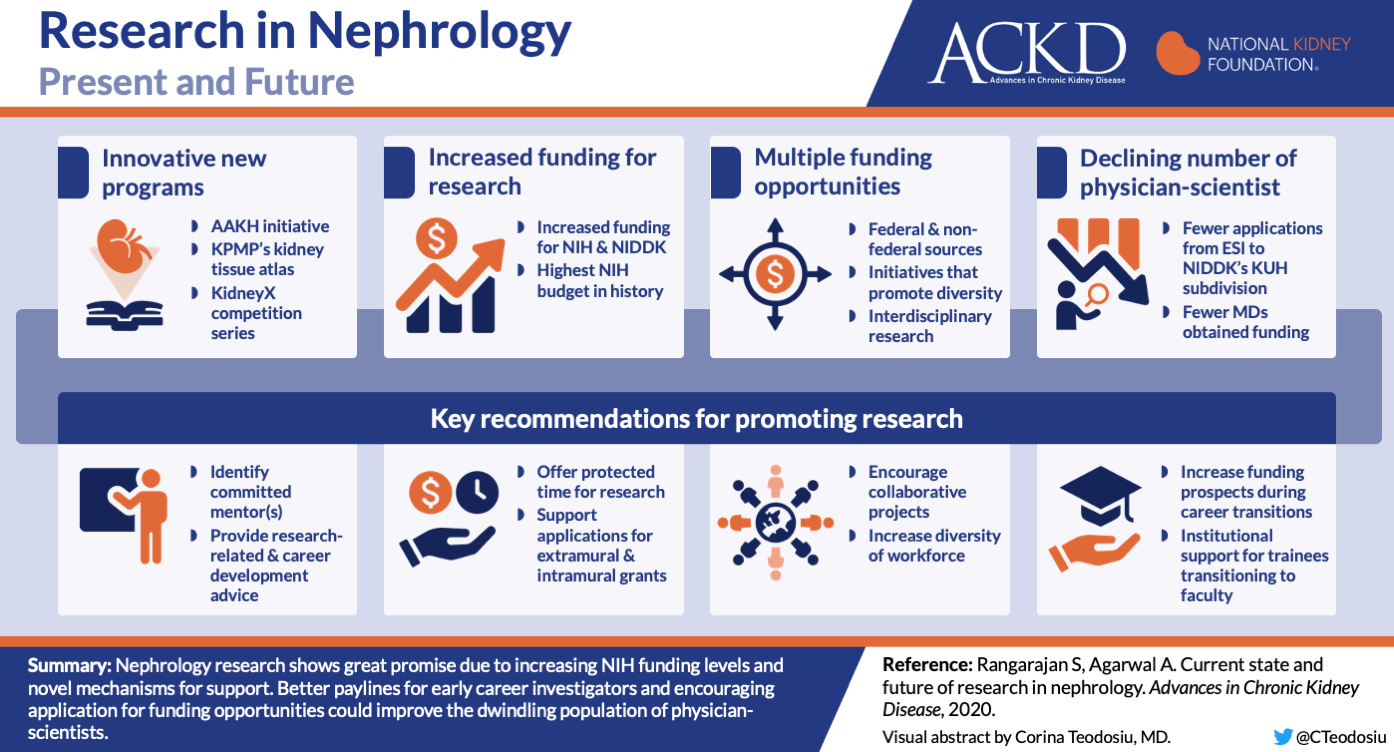
4. Research in Nephrology
In order to advance any field of medicine, it is imperative to have a strong and well-supported research component. The field of nephrology is currently witnessing several advances in kidney care. For example- SGLT2 inhibitors, GN management (anti-PLA2R), transplantation, tolvaptan for ADPKD and hyponatremia to name a few. Furthermore, initiatives like KidneyX and the NIH funded Kidney Precision Medicine Project have the potential to make even more important advances. Drs. Rangarajan and Agarwal discuss the current state of research funding in nephrology and importantly discuss several challenges to ensure a robust future of research in nephrology.
5. Nephrology Clinician Educator
The role of the clinician educator in nephrology is becoming further defined and developed. Dr. Roberts and colleagues review the skills needed for success and discuss various professional development opportunities including the attainment of advanced degrees. The authors describe how to become an effective educator, embrace technology/innovation, and describe how to ensure a sustained career as a successful clinician educator.
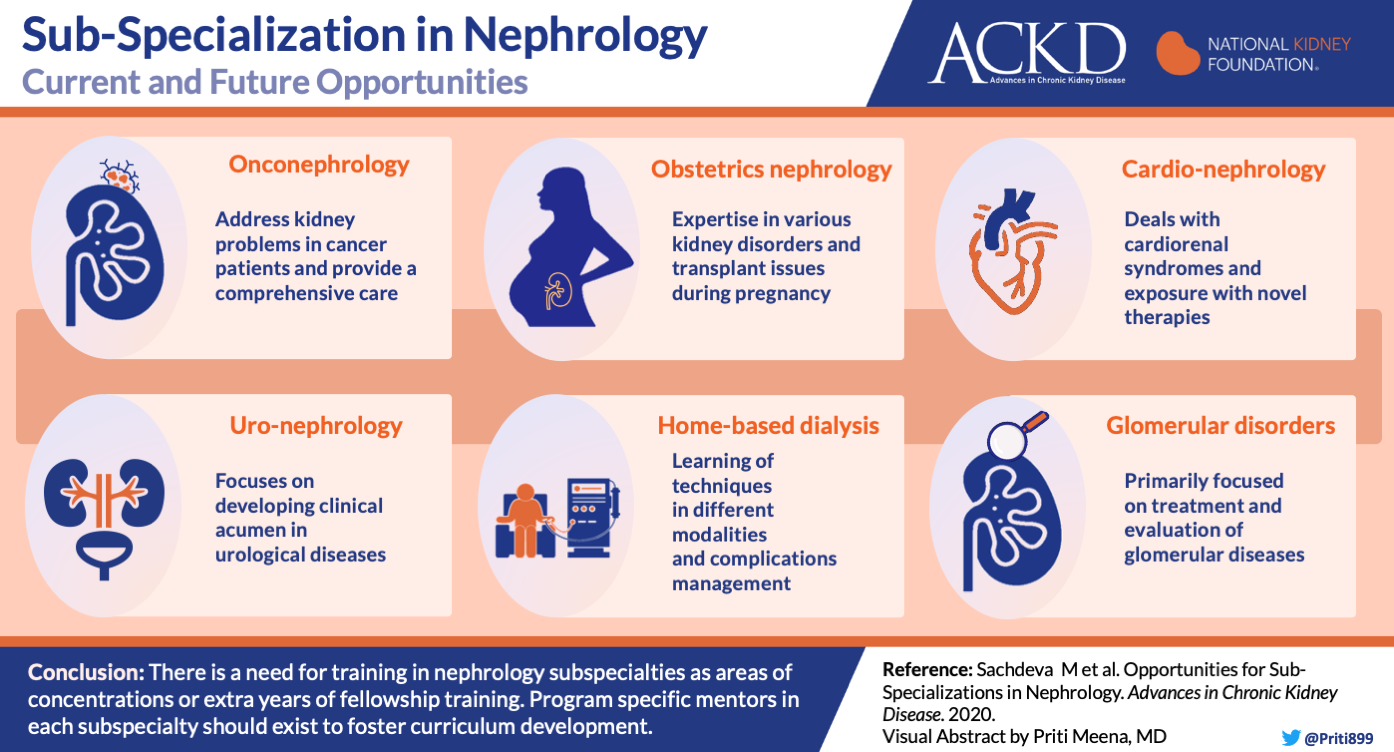
6. Sub-Specialization in Nephrology
Dr. Sachdeva and colleagues review several emerging areas of subspecialization in nephrology that aren’t as developed as the ones covered by stand alone articles in this issue. These includes onconephrology, obstetric nephrology, cardio-nephrology, uro-nephrology, home-based dialysis, and glomerular disorders. The authors review the current state and future of each areas.
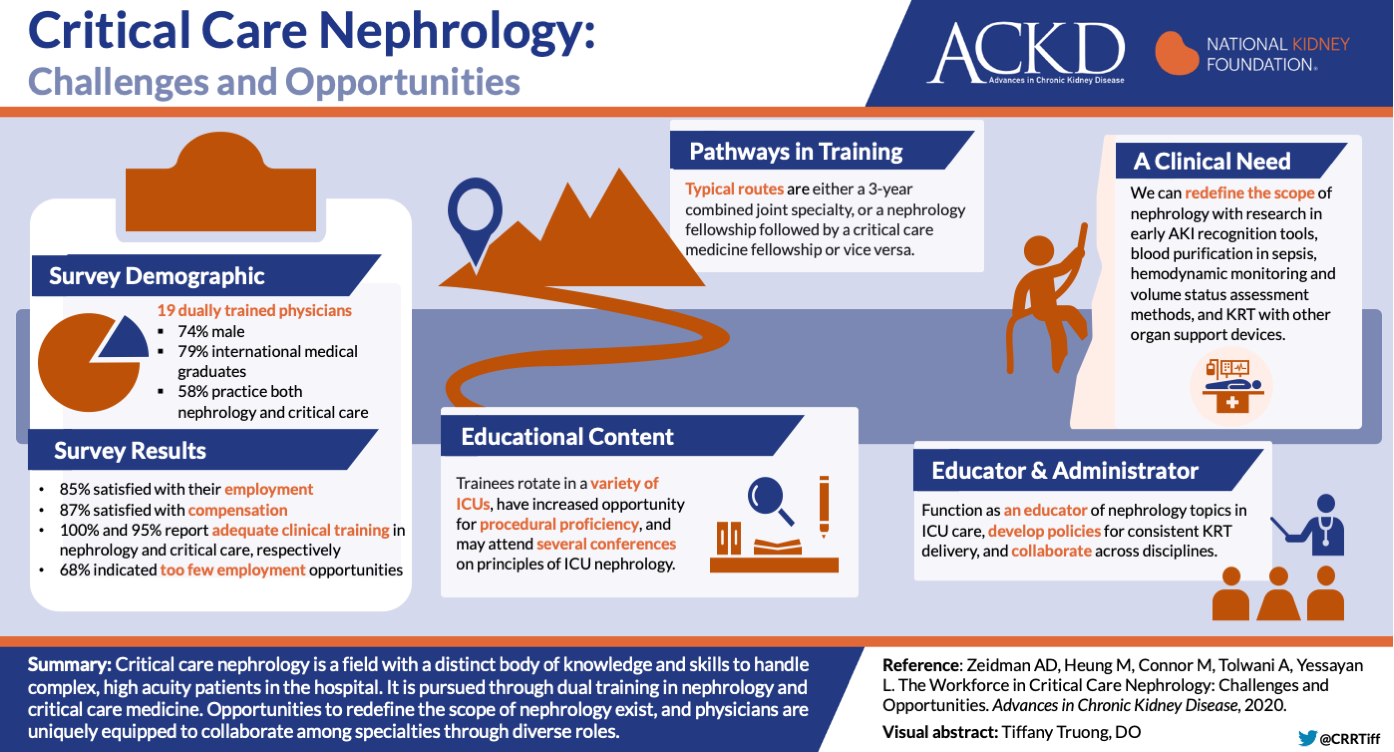
7. Critical Care Nephrology
The intersection between critical care and nephrology continues to grow. Dr. Zeidman and colleagues survey current individuals who are practicing both critical care and nephrology and ask about their satisfaction, compensation, and employment opportunities. The authors review the current training pathways available, educational curriculum, and current climate for employment. They also discuss the potential future of combined nephrology and critical care.
8. Transplant Nephrology Workforce
Dr. Concepcion and colleagues review the current state and future directions of the transplant nephrology workforce. Transplant nephrology is the most established subspecialty of nephrology with a well-developed training program and a defined clinical apparatus (medical directorship, independent service line). The authors review the current status of fellowship training, educational requirements, and the unique opportunities available in transplantation.

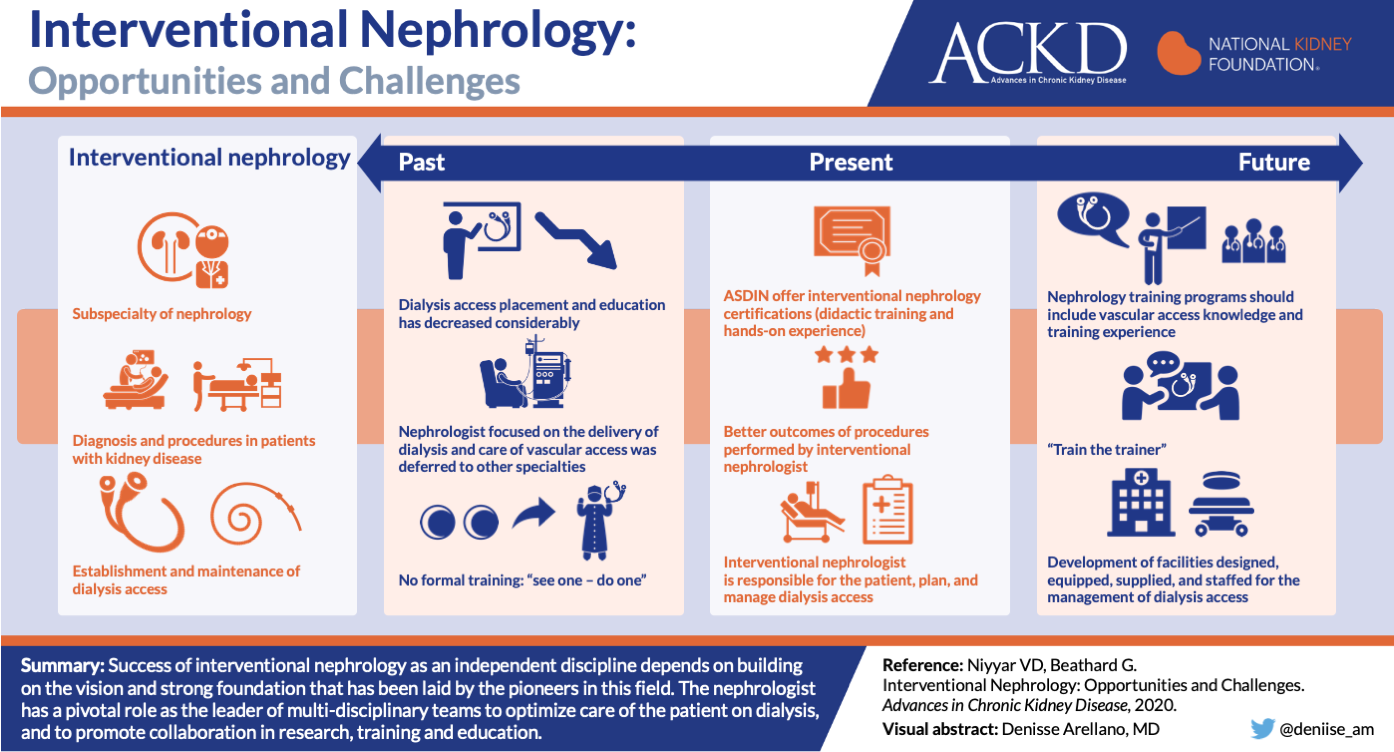
9. Interventional Nephrology
Dialysis access is a vital component to the patient undergoing dialysis. Interventional nephrology grew out the the need to provide close care and monitoring of dialysis access. Dr. Niyyar and Dr. Beathard discuss the past, present, and future of interventional nephrology. The discuss the evolution of the American Society of Interventional Nephrology (ASDIN), the growth of training programs offering certified training in Interventional Nephrology and a look at the future of the subspecialty.
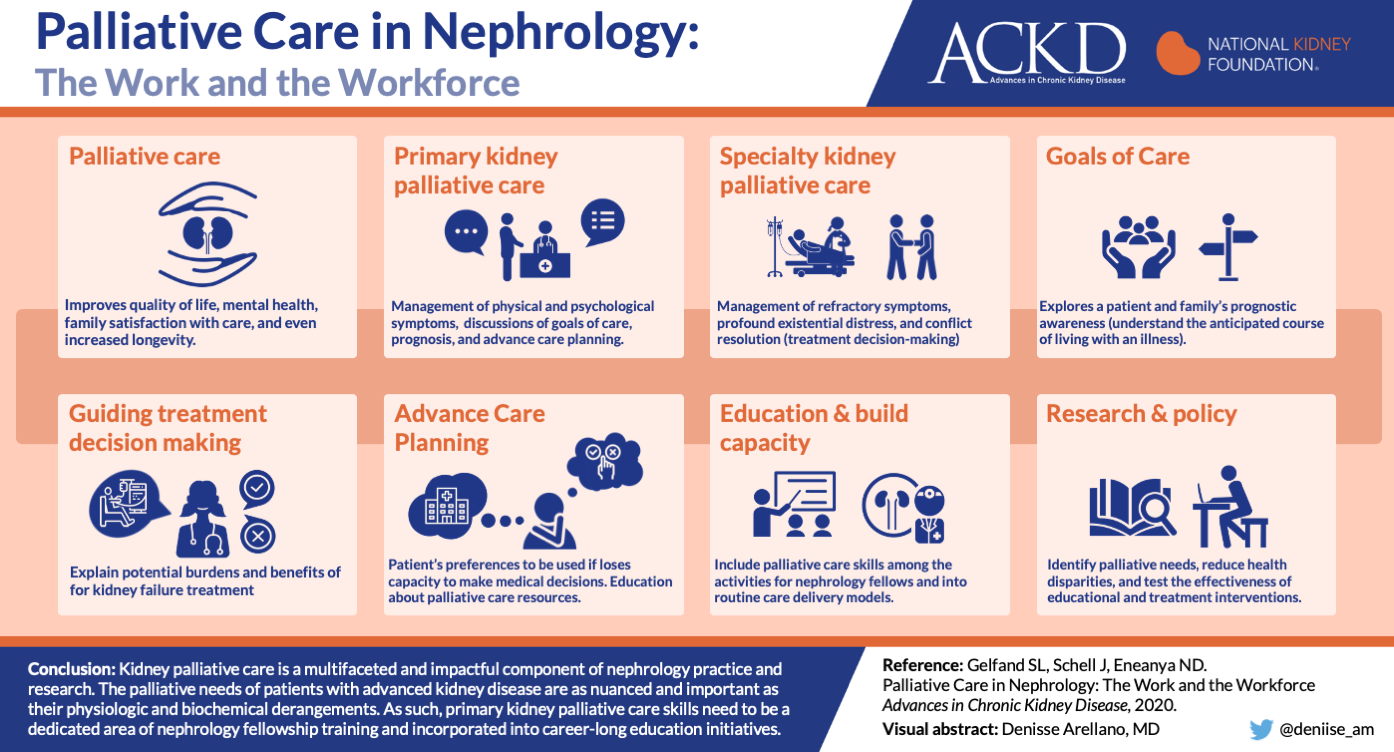
10. Palliative Care in Nephrology
Palliative continues to be an important part of the nephrology workforce. Dr. Gelfand and colleagues review the all aspects of the palliative care workforce including ensuring adequate exposure during fellowship training in order to build capacity. The authors discuss the importance of strong communication skills to help guide decision making, advance care planning, and goals of care. Finally, research and policy changes are needed to help ensure palliative care medicine continues to evolve and play an integral role in nephrology.
11. Private Practice Nephrology
The majority of practicing nephrologists in the United States are in private practice. Preparing fellows for a career in private practice has recently garnered increased focus. Dr. Agha and colleagues discuss strategies to ensure trainees are prepared for this transition. They also discuss traditional and emerging opportunities for individuals in private practice. These include diversifying ones practice, interventional nephrology, increasing use of home dialysis, research, and business ventures.