 The physical examination of volume status is perhaps the most common assessment we perform in everyday clinical practice. It is also one of the most difficult and subjective tasks to perform. In particular, the JVP is one of these mystical signs that even very accomplished physicians can find hard to get right. So, here are some essential facts about the JVP that the trainee nephrologist needs to know:
The physical examination of volume status is perhaps the most common assessment we perform in everyday clinical practice. It is also one of the most difficult and subjective tasks to perform. In particular, the JVP is one of these mystical signs that even very accomplished physicians can find hard to get right. So, here are some essential facts about the JVP that the trainee nephrologist needs to know:– The JVP should ideally be measured on the right side using the internal jugular vein, as anatomically this is the straightest column of blood in contact with the right atrium
– The JVP gives an indication of the pressure in the right atrium – it is not a direct measure of volume. We can infer some information regarding the volume status based on the pressure, but must remember that there are other influences at play.
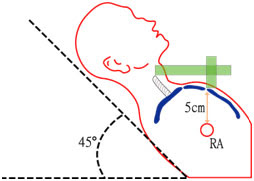
– The JVP should be measured with the patient at 45 degrees to the horizontal. In this position, the sternal angle is a vertical distance of ~5cm above the right atrium
– By convention the JVP is measured as the vertical height from the sternal angle, but many people add the additional 5cm when reporting it – the important thing is to state the reference point, i.e. RA or sternal angle
– A measurement of >3cm from sternal angle (>8cm from RA) is taken as evidence of high RA pressure in normal patients
– Points helpful in distinguishing the JVP from the carotid:
Visible, not palpable
Complex waveform – see here for more details
Varies with respiration – usually decreases on inspiration
Fills from above
Increases with pressure on the abdomen – the hepatojugular reflux
Most importantly, there are many conditions that can result in an elevated JVP:
1. Right ventricular failure
2. Tricuspid regurgitation or stenosis
3. Pericardial effusion or constrictive pericarditis
4. SVC obstruction – usually no waveform as transmission from the RA is blocked
5. Volume overload
In the next post I’ll try to cover some of the previous studies that have the examined the use of the JVP in clinical assessments and trials. Hopefully this has provided some useful review for trainees in one of the common everyday clinical practices.

Standing still or sitting down for long periods of time deactivates the muscular pumps resulting in a stagnation of blood in the legs and increasingly swollen veins. Long journeys by car, train and plane can be a severe strain on veins.
unsure if it was created by the author or not as it was 9 years go. You can use it.
Hello there. Great article/ post! Can you tell me: is the image/ diagram in this post created by Renal Fellow Or. or can you tell me who the original creator is? We’d like to use it in our course at Thompson Rivers University.
Cardiologists can estimate the blood pressure in the jugular vein by careful observation of the vein.
veins
The JVP is usually more obvious during inspiration. A low normal JVP is sometimes evident ONLY during inspiration. This is so because the descents, especially the X descent is brisker during inspiration and therefore more apparent.
Despite the inspiratory fall in intrathoracic pressure and the accompanying increase in venous return, there is a decline in MEAN RA pressure BUT an augmentation of RA contractile force. This preserves or increaes the crest of the A wave, thus accentuating the initial portion of the X descent as the RA relaxes more rapidly after its vigorous contraction. The Y descent is increased during respiration b/c tricuspid flow during the rapid filling phase is reinforced by the inspiratory fall in RV diastolic pressure.
Kussmaul's sign refers to an abnormal response to inspiration, that is a RISE in RA mean and jugular venous pressure
In a normal physiological state, inspiration will decrease intra-thoracic pressure (to suck air in), promoting venous return to the right atrium and therefore DEcreasing the JVP.
If the JVP increases on inspiration then something major is going on – this is known as Kussmaul's sign positive and can be associated with constrictive pericarditis and cardiac tamponade.
The JVD INCREASES, ( does not decrease) with inspiration!
A crude approach to the JVP is to have patient sit completely up right. If the JVP is visible its definitely elevated. Alternatively place the patient flat or near flat. If the JVP is not visible atleast half-way up the neck, it is low. You can then use the usual angles but in essence you are simply trying to identify a near normal JVP.
In order to allow patient comparisons, a reference is needed – by convention the reference angle has been 45 degrees. According to many clinical textbooks, at 45 degrees, the vertical height from the right atrium to the sternal angle is approximately 5cm.
If the patient does not have a visible JVP at 45 degrees, then lowering them to bring the JVP into visibility is a worthwhile maneuver. This new angle should be noted.
The patient angle should not matter if you are measuring the vertical distance to the sternal angle. I have heard of adding 4cm not 5cm,
There is a critical care study that showed the accuracy in Measuring JVP, regardless of level of training, is not sufficient enough to be clinically helpful. Given this I report JVD as low, med, or high (instead of a specific #). This also avoids confusion of whether the 4 cm was added or not.
There is a study out there (that I cant find) which concludes that hepatojugular reflex is BS.