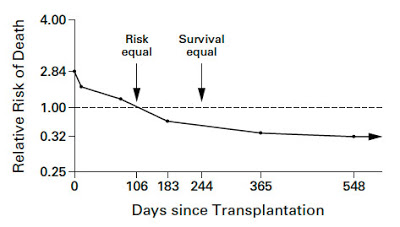
 The evaluation of a dialysis patient for possible kidney transplantation is a great challenge. On one side, we know that if the patient continues on dialysis, his yearly mortality will be around 20%. On the other hand, kidney transplantation carries a relative higher risk in the first year after transplantation and only those that survive over the first year will truly benefit from it. There is a classic paper from Wolfe et al. that shows when the line is crossed to the benefit side (Figure 1) in average.
The evaluation of a dialysis patient for possible kidney transplantation is a great challenge. On one side, we know that if the patient continues on dialysis, his yearly mortality will be around 20%. On the other hand, kidney transplantation carries a relative higher risk in the first year after transplantation and only those that survive over the first year will truly benefit from it. There is a classic paper from Wolfe et al. that shows when the line is crossed to the benefit side (Figure 1) in average.
In fact, recent analysis suggested that the traditional CV risk factors add little predictive value regarding development of coronary heart disease after transplantation. The most important transplant-specific predictors of cardiovascular events included duration of pre-transplant dialysis, new onset diabetes after transplantation and history of delayed graft function and/or acute rejection. Immunosuppressive drugs play a major role in some of these factors. In addition, advanced age, sex, race and obesity were also included to compose the PORT risk score, which predicts the probability of developing coronary heart disease after transplantation. This score performed better than the Framingham equation in the transplant population with a c-Statistic value of around 0.8.
In addition to patient selection, 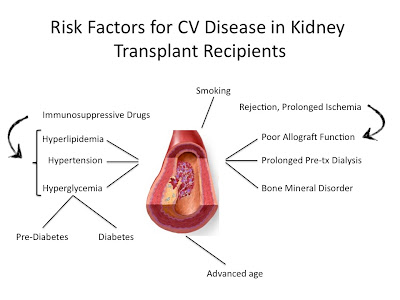 the post-transplant medical care is essential. A surprising observation came from Dr Gaston and colleagues’ work that evaluated the use of cardioprotective medications in kidney transplant recipients. Fewer than 30% of hypertensive patients with CV disease or diabetes were taking an ACEI/ARB 6 months post-transplantation, the use of aspirin was uncommon and statins were only prescribed in half of patients. We know that there are challenges with the use of ACEI/ARB in the initial period after transplantation due to its potential confusing effect with creatinine elevation. A meta-analysis comparing the effect of these agents with the traditional calcium channel blocker (amlodipine) showed that ACEI/ARB were associated with a decrease in GFR and a lower hematocrit, though proteinuria was significantly decreased and potassium levels were not affected.
the post-transplant medical care is essential. A surprising observation came from Dr Gaston and colleagues’ work that evaluated the use of cardioprotective medications in kidney transplant recipients. Fewer than 30% of hypertensive patients with CV disease or diabetes were taking an ACEI/ARB 6 months post-transplantation, the use of aspirin was uncommon and statins were only prescribed in half of patients. We know that there are challenges with the use of ACEI/ARB in the initial period after transplantation due to its potential confusing effect with creatinine elevation. A meta-analysis comparing the effect of these agents with the traditional calcium channel blocker (amlodipine) showed that ACEI/ARB were associated with a decrease in GFR and a lower hematocrit, though proteinuria was significantly decreased and potassium levels were not affected.
Despite their conclusion that there were insufficient data to determine the effect of ACEI/ARB on patient or graft survival, I strongly believe that extrapolating the literature from other populations is necessary due to the poor quality of trials so far. Diabetics and patients with proteinuria or history of heart failure/myocardial infarction would, in particular, benefit from those agents, in addition to statin/ASA once their kidney function has stabilized after transplantation. Highly opinion-based for now but hopefully new trials will be addressing this important question soon and meanwhile there is lots of room for improvement in the cardiovascular care after transplantation.

Dear Dr. Leonardo V Riella
It’s a great pleasure to read your blog. I find your post very informative. Lately, it seems that doctors and medical personnel are trying harder to monitor a patient’s risk factors for developing disease long before there are any obvious signs of a problem.
As a reader, I consider your writing to be a great example of a quality and globally competitive output. It would be a great thrill and honor if you could share your genuine ideas and knowledge to our community, Physician Nexus. With this you can gain 1000 physician readers from over 62 countries on Nexus.
We would love for you to visit our community. It's free, takes seconds, and is designed for physicians only – completely free of industry bias and commercial interests.
Best,
Lee Marie Lomoljo
On behalf of the Physician Nexus Team
http://www.PhysicianNexus.com