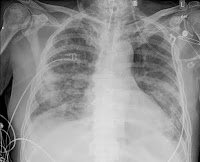
 While performing an electronic chart biopsy prior to examining a consult patient, I noticed a “nephrologic no-no,” which can be seen on the patient’s chest x-ray coursing under the right clavicle (see image). This finding was confirmed on my physical examination. The surgical team decided intra-operatively that the patient might need dialytic intervention so a right subclavian temporary dialysis catheter was placed. I had never seen one before, but I am sure many nephrologists who are no longer junior woodchucks like myself were around when subclavian dialysis catheter use was common. As my co-fellow Dr. McMahon pointed out in a previous post, the subclavian route was popular until an association was noticed between this route and subclavian thrombosis and stenosis. Ted Steinman, one of our attendings at The Brigham, co-wrote a paper this year entitled, “Dialysis at a crossroads: 50 years later.” In it, he and other pillars of nephrology propose a new path for dialysis therapy, and this is worth a read. One component of this path recommends changing the mantra “Fistula First” to “Catheter Last” given the unexplained augmented use of catheters and increased catheter-associated infections during the fistula first initiative. In other words, catheters should be the “last” choice for dialysis intiation given all of the complications caused by their use compared to grafts and fistulae. Furthermore, fistulae are not always attainable and cannot always be created in a timely fashion; thus, a graft is the next best thing and a very suitable alternative. The authors also propose that the Center for Medicare and Medicaid Services should consider catheter use to be sub-standard care. The overall premise behind the “Catheter Last” remains roughly the same, but this is an interesting way to think about our patients who are nearing the need for dialytic intervention that may motivate us more to prevent use of the dreaded catheter, especially when a subclavian one slips through the cracks.Posted by Will Pendergraft
While performing an electronic chart biopsy prior to examining a consult patient, I noticed a “nephrologic no-no,” which can be seen on the patient’s chest x-ray coursing under the right clavicle (see image). This finding was confirmed on my physical examination. The surgical team decided intra-operatively that the patient might need dialytic intervention so a right subclavian temporary dialysis catheter was placed. I had never seen one before, but I am sure many nephrologists who are no longer junior woodchucks like myself were around when subclavian dialysis catheter use was common. As my co-fellow Dr. McMahon pointed out in a previous post, the subclavian route was popular until an association was noticed between this route and subclavian thrombosis and stenosis. Ted Steinman, one of our attendings at The Brigham, co-wrote a paper this year entitled, “Dialysis at a crossroads: 50 years later.” In it, he and other pillars of nephrology propose a new path for dialysis therapy, and this is worth a read. One component of this path recommends changing the mantra “Fistula First” to “Catheter Last” given the unexplained augmented use of catheters and increased catheter-associated infections during the fistula first initiative. In other words, catheters should be the “last” choice for dialysis intiation given all of the complications caused by their use compared to grafts and fistulae. Furthermore, fistulae are not always attainable and cannot always be created in a timely fashion; thus, a graft is the next best thing and a very suitable alternative. The authors also propose that the Center for Medicare and Medicaid Services should consider catheter use to be sub-standard care. The overall premise behind the “Catheter Last” remains roughly the same, but this is an interesting way to think about our patients who are nearing the need for dialytic intervention that may motivate us more to prevent use of the dreaded catheter, especially when a subclavian one slips through the cracks.Posted by Will Pendergraft


The femoral vein is generally the next site considered after the right IJ as outlined by Gearoid here.
If a patient needs dialysis acutely…i.e. post op what else do you do, they probably went for the neck first and had a problem.
If you are fortunate enough to have a scheduled transplant in your near future yet discover that RRT is needed in the meantime, I can certainly see that the creation of a fistula would do little good; a subclavian catheter would be a good option for patients in this sort of situation. Your case is one of the exceptions of which Graham speaks.
While I awaited my scheduled kidney transplant, I developed the early symptoms of calciphylaxis or calcific uremic arteriolopathy. This was an unexpected development and my nephrologist decided that RRT was needed. Two days later I had a subclavian catheter inserted and two more days later I started with in-center hemodialysis. I was on dialysis for approximately 10 weeks before the transplant. The catheter worked very well for me, with no associated problems.
Graham, yes, I understand. Thanks for those comments. I like the sound of "rigorous constant evaluation."
MooseMom,
The reason population metrics (which can be as small as a single clinic panel or as large as the USRDS) are needed is actually outlined nicely above. When initially thinking about a care process issue such as catheter access most physicians' minds jump to the exceptions.
"I can't do any better than I am because the only time I fail is in the exceptional circumstance." This, of course, is not true.
Failures occur for multiple reasons along the care process some of which are outside the physicians direct control. These breakdowns are often only visable from the population level. In order to decrease the variance from the ideal, processes and outcomes need to be measured, analysed, stressed and remeasured.
The reasons behind current clinical outcome shortfalls are multiple and single sweeping solutions have clearly not been forthcoming. It's not that physician professionalism has failed it's that there's more at play impacting outcomes.
I believe that the way forward is through rigorous constant evaluation of our care and improving whenever we find a quantifiable shortcoming in a way that benefits both the individual and the population.
The current low number of patients on home hemodialysis, which is a concern of yours that I share, has multiple causes and can be addressed in the above systematic manner without RCT.
And yes, "suboptimal" is a euphemism.
If I had had three unsuccessful AV fistula surgeries, I would certainly think twice about having a fourth go, and I wouldn't claim my nephrologist was giving me "sub-standard care". I would, however, probably be questioning the ability of the vascular surgeon!
Do you all really need "metrics" to provide "quality care impetus"? That's a disturbing thought.
Yes, current dialysis care is indeed subobtimal (and that's a euphemism), and while RCTs are valuable, they are not going to alleviate the true suffering of a dialysis patient who crashes TODAY.
Thank you.
Anonymous,
This certainly does not sound like "substandard" care. It sounds like excellent patient centered care (assuming your patient was educated about and offered PD if possible, which I'm sure they were).
I believe that the ESRD Quality Incentives Program (QIP) and others like it should guide population care rather than individual patient care. We all have patients who, after careful followup and evaluation end up with a catheter for one reason or another. As I understand it, the QIP catheter metrics are based on the population care principle. We will get payed for the exceptions but not if we have an unreasonably high number of them.
These metrics will hopefully provide both financial and care quality impetus for us improve our delivery systems so that the exceptions become more infrequent.
I think we all agree that the current state of dialysis care is suboptimal. We need to approach the improvement in value of our care models with the same rigor that for years has been applied to the areas of basic and clinical research.
Interestingly, there are patients who refuse peripheral access. One is awaiting a transplant, and has had three attempted AV access surgeries which were unsuccessful. She declines further access surgery. Does my compliance with her wishes, after extensive discussion and informed consent, make my care of her 'substandard'? In my experience, AV access surgeries are sometimes easier conceived than accomplished.
It's still a good thing to know HOW to put in a subclavian. I've been "out there" 4 years and have put in maybe 10 subclavians, out of about 300 lines. Always when other sites are taken, occluded, or otherwise unable to place a line.
Yes, Graham, you're spot on! And thank you for saying that my comments are always appreciated. I'm not sure I believe you, but that's a charming thing to say, anyway. LOL We see RFN as our hope for the future. I love this blog and check it every day. Thank you for the opportunity to comment.
Cheeler,
Thanks for the comment and agreed that exceptions do exist.
However, we can't let the exceptions blunt our enthusiasm for performance improvement (which I don't think you imply but just to be clear). Ideally quality metrics set the bar just above where we are currently and then move higher upwards as we innovate.
These targets are not always easy to achieve (if they where we'd all already be meeting them!) but with focused work should be possible. Take at look at the work of Kaiser Hawaii as an example of the supposedly insolvable problems of late referral and starting HD with fistula.
MooseMom,
As always, your comments are appreciated and thank you for the link to the Hemodoc post.
I assume (and correct me if I'm missing the mark) that you post this as a reminder that reducing catheter rates, while an important goal, is not the only part of the nephrology value improvement movement. Increasing the numbers of patients on home hemodialysis is also an important metric that we need to address a we move forward.
http://www.hemodoc.com/2010/12/at-a-crossroads-or-just-on-the-wrong-road.html
Making catheter use sub-standard of care by CMS guidelines/reimbursements may be tricky. Often (it seems to me) that patients with CKD approaching dialysis have a goal of care that is palliative in nature should they approach the need for RRT (i.e., they would decline dialysis). However, oftentimes their goals of care change when they become uremic, after they have already bypassed the ideal time for fistula planning and maturity, and need catheter placement.