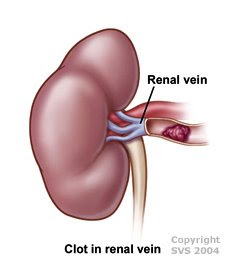
 Renal vein thrombosis is a thrombotic occlusion of one or both renal veins. Its most common cause is nephrotic syndrome, which is a hypercoaguable state though to be due at least in part to loss of the anticoagulant proteins protein C, protein S, and antithrombin III from diffuse protein wasting. It can also be secondary to nearly all other forms of nephrotic syndrome (e.g., minimal chnage disease, FSGS, MPGN) and also lupus nephritis particularly in the setting of a lupus anticoagulant. Renal cell carcinoma is also commonly associated with renal vein thrombosis, and local spread of tumor may also continue into the renal vein clot. A variety of imaging tools (e.g., venography, ultrasound, MRI, etc) are available for diagnosis of renal vein thrombosis but the most common means of diagnosing it currently is a CT scan with iv contrast. Surgical means of evacuating the clot are becoming increasingly rare and the mainstay of therapy involves anticoagulation and correcting the underlying cause (e.g., treating nephrosis with ACE-I/ARB, immunosuppresants as warranted, etc). The idea of giving prophylactic anticoagulation to prevent venous thrombosis in nephrotic syndrome is still a controversial one.
Renal vein thrombosis is a thrombotic occlusion of one or both renal veins. Its most common cause is nephrotic syndrome, which is a hypercoaguable state though to be due at least in part to loss of the anticoagulant proteins protein C, protein S, and antithrombin III from diffuse protein wasting. It can also be secondary to nearly all other forms of nephrotic syndrome (e.g., minimal chnage disease, FSGS, MPGN) and also lupus nephritis particularly in the setting of a lupus anticoagulant. Renal cell carcinoma is also commonly associated with renal vein thrombosis, and local spread of tumor may also continue into the renal vein clot. A variety of imaging tools (e.g., venography, ultrasound, MRI, etc) are available for diagnosis of renal vein thrombosis but the most common means of diagnosing it currently is a CT scan with iv contrast. Surgical means of evacuating the clot are becoming increasingly rare and the mainstay of therapy involves anticoagulation and correcting the underlying cause (e.g., treating nephrosis with ACE-I/ARB, immunosuppresants as warranted, etc). The idea of giving prophylactic anticoagulation to prevent venous thrombosis in nephrotic syndrome is still a controversial one.


Another feature may be the presence of significant proteinuria. I cared for a SLE patient being treated for LN, proteinuria <1gm 1 week before. Admitted to the hospital with AKI, 17gm protein/gm creatinine, and massively distended lower extremities and increased abdominal girth. Found to have thrombus involving the IVC and RV. She had no suggestion of a lupus flair.
Patients with nephrotic syndrome are hypercoagulable and have an increased incidence of both arterial and venous thrombi. Urinary losses of ATIII, plasminogen and increased platelet count/platelet aggregation are among the possible mechanisms.
DVT of the extremities is the most common TE event observed in patients with nephrotic syndrome.
Why is RVT common in nephrotic syndrome? Hypercoagulable state +
1.Immune complex injury to glomerulus resulting in increased procoagulant activity.
2.loss of fluid across the glomerulus and the resulting hemoconcentration in the postglomerular circulation, which is worsened by diuretic therapy
Acute RVT is manifested by severe flank pain, microscopic or gross hematuria, increased LDH, acute renal failure in bilateral RVT and increased kidney size on imaging.
Chronic RVT is often silent an can present as PE.
Gold standard for diagnosis of RVT is renal inferior vena cavagram with selective renal venography which could allow also therapeutic intervention (catheter thrombectomy for acute RVT)
Routine screening and prophylactic anticoagulation for RVT is not recommended for patient with nephrotic syndrome.
Patients who have membranous nephropathy, massive proteinuria and low albumin ( <2.0 g/dl) represent the highest group for TE events and prophylactic anticoagulation is recommended by experts if they have an additional risk factor ( morbid obesity, immobilization, severe heart failure, previous TE event…)
Patients who have RVT and nephrotic syndrome should receive anticoagulation with warfarin targeting an INR of 2.0-3.0 for as long as they remain nephrotic and for a minimum of 6-12 months.
When starting heparin in patients with nephrotic syndrome for a TE event before switching to warfarin , be aware that these patients might require higher doses to raise the PTT into target range as their ATIII level is low and they may be relatively heparin resistant.