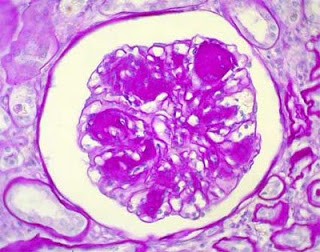
 Nodular glomerulosclerosis refers to a histologic pattern of nodular mesangial sclerosis with accentuated, lobular-appearing glomeruli on renal biopsy. Although classically described in association with diabetes (the so-called “Kimmelstiel-Wilson lesion”), the lesion is NOT pathognomonic for diabetic nephropathy. In fact, a number of renal conditions have been seen in association with this distinctive, histologic pattern. The differential diagnosis of non-diabetic, nodular glomerulosclerosis includes, but is not limited to:
Nodular glomerulosclerosis refers to a histologic pattern of nodular mesangial sclerosis with accentuated, lobular-appearing glomeruli on renal biopsy. Although classically described in association with diabetes (the so-called “Kimmelstiel-Wilson lesion”), the lesion is NOT pathognomonic for diabetic nephropathy. In fact, a number of renal conditions have been seen in association with this distinctive, histologic pattern. The differential diagnosis of non-diabetic, nodular glomerulosclerosis includes, but is not limited to:- Immunotactoid GN
- Fibrillary GN
- Fibronectin GN
- Cryoglobulinemic GN
- Amyloidosis
- Light Chain Deposition Disease (LCDD)
- Heavy Chain Deposition Disease (HCDD)
- Idiopathic Nodular Glomerulosclerosis
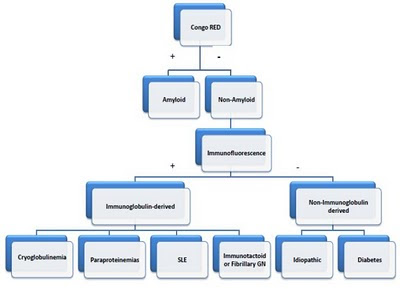
In order to determine the specific disease responsible for nodular glomerulosclerosis, a deliberate inspection of the renal biopsy (particularly, Congo red staining and IF) are requisite. The diagnosis of “idiopathic” nodular glomerulosclerosis remains one of exclusion. The following algorithm provides a systematic approach to the diagnosis of non-diabetic, nodular glomerulosclerosis:
 A strong, causative association between long-standing cigarette smoking and hypertension has recently been identified in individuals previously categorized as having “idiopathic” nodular glomerulosclerosis. In the largest case series available of “idiopathic” nodular glomerulosclerosis (n=23), Markowitz et al found a high prevalence of hypertension (95.7%), smoking (91.3%), hypercholesterolemia (90%), and extrarenal vascular disease (44%). The mean pack-years for smoking were 53 +/- 7 years. This cohort, in which diabetes was excluded, was comprised mainly of older, Caucasian male patients. The clinical presentation of this condition included renal failure (mean sCr 2.4 mg/dL) and proteinuria (mean 24 urine protein 4.7 g/d). The median time from biopsy to ESRD was 26 months.
A strong, causative association between long-standing cigarette smoking and hypertension has recently been identified in individuals previously categorized as having “idiopathic” nodular glomerulosclerosis. In the largest case series available of “idiopathic” nodular glomerulosclerosis (n=23), Markowitz et al found a high prevalence of hypertension (95.7%), smoking (91.3%), hypercholesterolemia (90%), and extrarenal vascular disease (44%). The mean pack-years for smoking were 53 +/- 7 years. This cohort, in which diabetes was excluded, was comprised mainly of older, Caucasian male patients. The clinical presentation of this condition included renal failure (mean sCr 2.4 mg/dL) and proteinuria (mean 24 urine protein 4.7 g/d). The median time from biopsy to ESRD was 26 months.Although the pathogenesis of “idiopathic” nodular glomerulosclerosis remains enigmatic, some have proposed that smoking alone is the putative agent. Potential mechanisms of renal damage induced by smoking include: oxidative stress from free radical formation, increased formation of advanced glycation end products (AGE), angiogenesis, and altered intrarenal hemodynamics. Given the plausible role of smoking in the pathogenesis, some have argued the nomenclature be changed to “smoking-associated nodular glomerulosclerosis”.
In summary, if the renal boards present a non-diabetic, elderly man with an extensive history of smoking, who insidiously develops renal failure and proteinuria, in conjunction with a renal biopsy that shows nodular glomerulosclerosis and negative IF and Congo red staining, the diagnosis is assuredly “idiopathic” or “smoking-related” nodular glomerulosclerosis.
Michael Lattanzio, DO


this does not exist…
We had a similar post few weeks ago
Check it out.Related to smoking and kidney disease. The key point is are pathologists going to start making these comments in their report and making this a diagnosis because right now its just an association. A good one but since so many people smoke– Why don't we see this more often!!!
http://www.nephronpower.com/search/label/glomerular%20diseases
Great post. Need to add labels to this post so we can refer to it later.