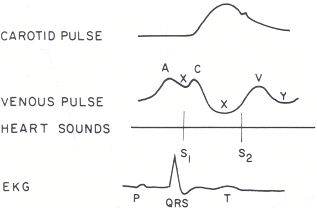
 In the previous blog we discussed some of the physiological principles underlying the JVP. Now I thought I’d present some manuscripts relating to the utility of the isolated use of JVP in clinical practice.
In the previous blog we discussed some of the physiological principles underlying the JVP. Now I thought I’d present some manuscripts relating to the utility of the isolated use of JVP in clinical practice.The first is a comparative study of hand-held ultrasound examination of IVC diameter vs clinical JVP assessment in determining RA pressure among medical residents. All assessments occurred within one hour of patients having a right heart cath. One resident, blinded to the ultrasound results performed the clinical examination in 40 patients. The JVP was not visualized in 37% of the 40 patients. In the remaining 63%, the sensitivity for predicting an RA pressure >10 mm Hg was 82% with ultrasound and 14% from JVP inspection. This of course is an extremely small study, with only one person at one experience level performing the exam.
An interesting study examining the presumed distance between the sternal angle and the mid right atrium recruited 160 patients undergoing CT chest scans. Using geometric calculations, they estimated the sternal angle – RA distance to be 8 cm, 9.7 cm and 9.8 cm at 30, 45 and 60 degrees elevation respectively. They found considerable inter-subject variability, with dependent variables including age, smoking status and AP chest diameter. This really emphasizes the need for a standard reference point to allow intra-patient comparisons and poses questions of the ability to compare similar measurements in different patients.
A systematic review published in Chest in 2008 examined the usefulness of measured CVP in relation to blood volume, CVP in determining fluid responsiveness and finally delta CVP in determining fluid responsiveness. 24 studies with a total of 803 patients were included. The pooled correlation coefficient between CVP and blood volume was 0.16 (95% CI 0.03, 0.28). Following fluid administration, the pooled correlation coefficient between baseline CVP and delta Cardiac Index was 0.18 (95% CI 0.08, 0.28); the pooled correlation coefficient between delta CVP and delta Cardiac Index was 0.11 (95% CI 0.015, 0.21). These results suggest a poor relationship between the isolated inspection of CVP and prediction of blood volume and fluid responsiveness, with the caveats of study heterogeneity in a systematic review.
These studies underscore that the JVP should not be used in isolation, as a measure of volume status nor fluid responsiveness. Furthermore, in order to derive any usefulness from it, we must understand what it actually signifies. As long as we perform it with a standard approach in each patient, understanding the fact that it’s a window to the pressure in the RA (not volume) and if it is part of an overall patient examination, then I think it can help with a detailed clinical work-up. Remembering that there are many processes that can cause an elevated JVP will help broaden your differential and keep you alert to the possibility of alternative patho-physiological processes. As one of my attendings said, ‘it’s free and you can do it everyday’.

