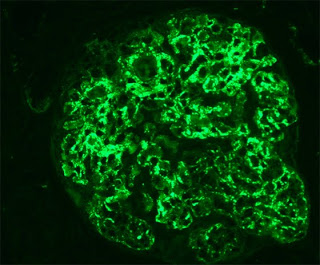
Six months after a kidney transplant, a patient developed a rising creatinine, significant proteinuria (~2g/day), hematuria and low C3 levels. A kidney graft biopsy showed severe glomerulonephritis with mostly occluded capillary loops with immunofluorescence staining negative for immunoglobulins but strongly positive for C3 (representative picture on left). On EM, subendothelial and mesangial electron dense deposits were visualized. The features are characteristic of the so-called C3 glomerulonephritis (GN).
C3 GN is part of the same family as dense deposit disease (DDD) and fall into the new proposed classification of C3 glomerulopathy. Compared to C3 GN, DDD is characterized by extremely electro-dense intra-membranous deposits on EM. Both entities can present with features of MPGN, once significant chronic endothelium glomeruli damage occurs. These glomerular pathologies shared in common its pathogenesis, which involves complement dysregulation.
Classically, immunoglobulins that deposit in the glomeruli are the major triggers of glomeruli inflammation. In rare settings such as C3 GN, complement proteins are present in the glomerular lesions in the absence of immunoglobulins. Abnormal activation of the alternative pathway is implicated on this finding. Either an acquired or inherited defect in the control of alternative complement pathway should be investigated.
The following tests are generally recommended:
** Levels of C3 and complement factors B/H/I
** Presence of C3 nephritic factor (C3 NeF)
** Genotyping for certain complement mutations (common in kids)
Our patient underwent complement testing and was found to have circulating C3 nephritic factor. This factor is an IgG autoantibody that directly stabilizes the C3-convertase activating complex of the alternative pathway and thereby prevents the normal inhibitory action of complement factor H, leading to continuous activation of the complement cascade and consequent deposition of complement by-products in the glomeruli.
Although atypical hemolytic uremic syndrome (aHUS) is also strongly associated with a dysregulation of the alternative pathway, glomerular lesions in aHUS do not exhibit C3 deposits or electro-dense deposits on electron microscopy, differentiating from C3 glomerulopathies. How changes in complement regulation leads to very diverse presentations might be related to the underlying defect. Nonetheless, atypical HUS could be placed in one side of this spectrum of renal diseases associated with alternative complement dysregulation (figure below; adapted from Servais et al. 2007).
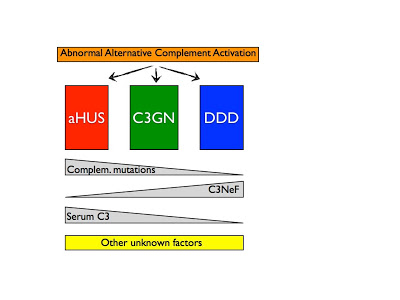
While the pathogenesis is complicated, even harder is the treatment challenge of C3 GN in our patient above. There are a couple of new promising approaches and markers that might help guide therapy. I will try to cover them on my next blog.


Thank you for the comments. I agree Raghuanth, the major difficulty with these patients is getting the complement tests done. They are expensive and take a long time to come back, therefore limiting the applicability to all patients. We are trying to work with some companies to optimize that. Will update on the blog as we get things more consistent.
That was a nice post. We also have been getting a lot of biopsy immunofluroscence results with just C3 alone and having diverse LM pictures ranging from normal histology to mesangioproliferative to crescentic. We are sending EM for all these and planning to do a series on them. Unfortunately we dont have facilities for doing a full complement workup and I think thats really needed in all these cases.