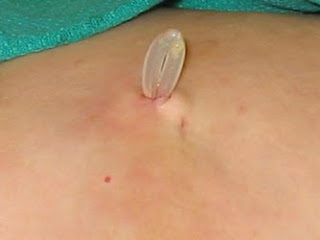
One of the issues that we come across repeatedly in the clinic is the timing of access insertion. We all want to avoid the use of catheters and so we refer patients early (when possible) for fistula formation. This is a bigger problem when your patient wants to start PD. You don’t want the patient to have the catheter placed too early because then they will be unnecessarily exposed to the risk of infection. At the same time, you don’t want to wait too long and get to the stage where the patient requires urgent HD (and often, once they start HD it is difficult to make the transition to PD). I saw a patient in the clinic a few weeks ago that fits this bill perfectly. He is an otherwise healthy man in his 60s who has a very active life and a full-time job. His creatinine had been stable for 2-3 years but climbed rapidly earlier this year and we thought he would need to start soon. However, his creatinine stabilized again and he is feeling well so we have him in a holding pattern with regard to the PD catheter insertion. Our surgeon suggested implanting a buried PD catheter, a technique that he has just started doing in our institution. For this technique, the catheter is buried subcutaneously at the time of insertion. Then, when the patient is ready to start dialysis, the subcutaneous portion is externalized and the catheter can be used straight away. This can be done in the dialysis clinic and does not require a trip to the OR. Thus, a catheter can be inserted months (or even years) prior to use and the problem of timing is dealt with very elegantly. Recently, a paper was published which described the experience of the University of Denver where they have been using this technique as standard since 2000. In total, 134 catheters were implanted in that time. The period prior to externalization varied between 2 and 788 days with an average of 40 days. There was no relationship between catheter embedment time and the risk of catheter failure. 90% of catheters worked immediately and of the remaining 13 catheters, 12 were easily corrected laparascopically. Only 1 patient failed this technique and required transition to HD. This seems like a great technique and I look forward to seeing the results here over the next few months.
See also this earlier paper in KI about the experience with the use of buried catheters in Ottawa.

Great post. I have been reading articles online about straight catheter's because it was brought up in my nursing class the other day, that's how I came across your blog. I'm happy I did because this was a very interesting read. Thank you for sharing this with us!