Nephrology grand rounds in Duke University Medical Center this week inspired me to write this blog on a subject I now realise that I am weak on. Patients on dialysis are a unique group in whom we see diseases that are either vanishingly rare or not seen in non-renal patients. This includes diseases of the skin. I will give an overview of some of these conditions. Markova et al, gives a good overview of most skin disorders peculiar to renal patients. This will be part of a series of posts on skin disorders in renal patients.
1)Skin disorders involving calcification in renal failure.
Calcium and phosphate deposition in the skin has been said to be a contributing factor to pruritus that is common in renal failure as well as in other skin disorders. Here are two contrasting calcium related skin disorders with very different outcomes.
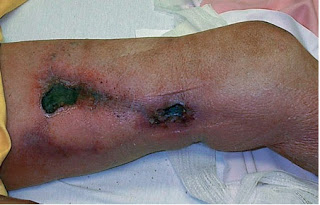
Calciphylaxis. In this disorder calcification of the small vessels of the dermis and subcutaneous tissues occurs. This leads to vessel thrombosis, tissue infarction and skin necrosis. It occurs in 1-4% of dialysis patients. Risk factors include hyperparathyroidism, an elevated calcium-phosphate product (>70 mg2/dl2), diabetes mellitus, female sex, obesity, warfarin use, and protein C or S deficiency. 1-year survival after the diagnosis of calciphylaxis is about 50%. In calciphylaxis patients get very painful violaceous reticulated plaques that are well defined and deep. These lesions develop into deep non-healing ulcers that can become gangrenous. Sepsis is the most common cause of mortality. Treatment options include a low phosphorous diet, normalizing calcium and phosphate with non-calcium based phosphate binders and low-calcium dialysate. Sodium thiosulphate 25g VI over 30 minutes three treatments per weeks has been shown to improve lesions and should be continued for 2 months beyond the resolution of lesions.
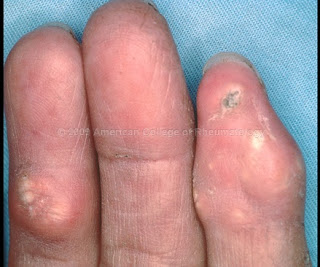
Calcinosis cutis. This refers to calcium deposition in the skin and is a subtype of calcinosis, a condition describing calcification in vessels and organs. Patients with calcinosis cutis get painless flexural infiltrating plaques at periarticular sites. The size and number of plaques corrolate with degree of hyperphosphatemia. Unlike calciphylaxis this disorder does not cause skin necrosis. Risk factors include low albumin, high phosphate, high alkaline phosphatase and morbid obesity. It occurs in about 1% of dialysis patients. There is no gold standard treatment but normalisation of calcium and phosphate can cause lesions to regress.
Posted by Andrew Malone



Duly noted and fixed.
A common mistake to be noted in this post is the word pruritis. I suppose it is meant as lingo for itching, however the correct word would be pruritUS, which is latin for itching and does not have anything to do with the ending -itis that is used for inflamatory disorders. This is a common mistake as pointed out in thisJAMA post: http://archderm.jamanetwork.com/article.aspx?articleid=209509