CyC is a 13 kDa cysteine protease inhibitor that is produced by all nucleated cells. It is freely filtered at the glomerulus and then catabolized in the proximal tubule such that very little appears in the urine. CyC levels are affected by renal function but also independently influenced by age, gender, BMI, fat mass, triglycerides and the presence of diabetes. Interestingly, these are all components of the metabolic syndrome.
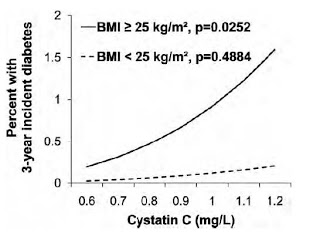
In 2011, a paper was published in Diabetologia that found that elevated levels of CyC were associated with an increased incidence of type II diabetes. The thought was that CyC was potentially involved in the pathogenesis of diabetes. In July, a paper was published in NDT that shed a bit more light on this issue. The authors reported the results of a 3-year study of French adults in whom the incidence of diabetes was low. In this study, in common with previous research, CyC predicted incident diabetes. However, when stratified by BMI, CyC predicted incident diabetes only in participants with a BMI >25 at baseline.
So what is the explanation for this? CyC secretion has been shown to be 2-3 times higher in obese patients than in non-obese patients. CyC is also highly expressed in subcutaneous adipose tissue. Data from the Framingham Heart Study has shown that adipose tissue was not associated with CKD using creatinine-based estimating equations while it was associated with CKD using a CyC-based equation. CyC may play a role in preventing inflammation associated with increased adiposity explaining the increased secretion in obese patients.
The implications of this are that, although CyC may predict diabetes, it is unlikely that it adds any more to prediction algorithms considering that it is not independent of BMI and the metabolic syndrome – both of which are well known to be associated with diabetes. The second implication is that the fact that CyC is better at predicting mortality than creatinine (at the same level of eGFR) is related to non-renal factors – again, adiposity and the metabolic syndrome. It similarly suggests that in obese patients, estimating equations that utilize CyC may not be as accurate as previously suggested. The search for a better biomarker of GFR continues…