Having completed four years of medical school, three years of residency, and now a few months away from my completing my training as a nephrology fellow, I experienced a new type of learning – interprofessional education (IPE). IPE is defined as an occasion when learners from two or more professions in health and social care learn together with the objective of cultivating collaborative practice to provide patient-centered care. As nephrology fellows, we have significant interactions with other health professions everyday: dialysis nurses, technicians, medical/surgical nurses, patient care assistants, nurse practitioners, and physician assistants.
IPE has been endorsed by the Institute of Medicine (IOM) and described as an important step in advancing health professional education for many years. Not surprisingly, the IOM states that patients receive safer, higher quality care when health care professionals work effectively as a team, communicate productively, and understand each other’s roles.
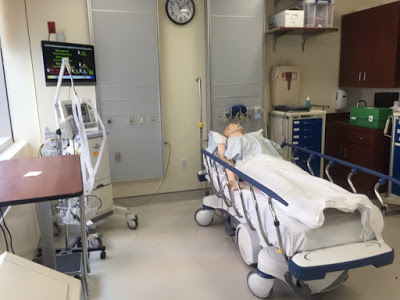
The IPE workshop I participated in was set in an advanced medical simulation center and involved physicians and nurses. The simulation room was complete with a monitor for vital signs and telemetry, a wide variety of medications and medical equipment, and a jarringly realistic patient mannequin who not only blinked and talked, but also had palpable pulses, audible heart and lung sounds, and even ultrasoundable tissue.
The simulation began with the assignment of roles (i.e. physician, nurse, respiratory therapist) and the description of a clinical scenario. Our first scenario was a patient with altered mental status in the setting of profound hypoglycemia. After the simulation began, we were recorded on video and also observed by a “debriefer” with whom we would discuss the simulation afterwards. The vital signs, physical exam findings, and voice of the patient were controlled by other members of the simulation team (who were behind a one-way mirror) in response to our actions in the simulation. Subsequent simulations involved situations where the patient experienced anaphylactic shock after receiving an antibiotic, crushing chest pain concerning for myocardial infarction, and cardiac arrest.
The debriefing session with the debriefer and all simulation participants, perhaps the most enlightening portion of the activity, allowed the entire team to talk about what went well and what didn’t go so well. Most importantly, we discussed how our teamwork and communication skills could improve. Had tasks been delegated effectively? Did all members of the team know their role and feel part of the team? Was the ultimate goal clear? When and why did communication breakdown?
The discussions often led to thoughts on perceived perceptions of other professional roles and important clarifications of what each team member can contribute. In one simulation, our “actual” roles were reversed, which led to an even richer discussion during the debrief session. We briefly discussed and received feedback on clinical management, though clinical performance was not the main focus of the debrief session.
Though this type of activity requires the participants to buy in to the simulation experience to maximize its effectiveness, it provides a unique opportunity to practice and learn from an almost real-life setting. Before attempting venipuncture on a patient, trainees can practice on their colleagues. Before placing central venous catheters or performing cardiopulmonary resuscitation (CPR), trainees may practice on mannequins. Interprofessional communication is a core skill set that everyone needs to practice and hone. Mastery of this skill set will ensure the delivery of the highest quality of care. I believe that we, as a medical community, need to start including IPE into the curriculum at all levels of medical training. If practice makes perfect, shouldn’t we all start practicing how we interact with other professionals?
Samira Farouk, MD
NSMC Intern 2018
Chief Nephrology Fellow, Icahn School of Medicine at Mount Sinai