Experimental Biology (EB) took over the city of Orlando, FL from April 6th to the 10th. It is the largest interdisciplinary annual meeting, hosting five different societies, and bringing together thousands of scientists from around the world. It is a one-of-a kind meeting that explores cutting edge science from fields ranging from anatomy, biochemistry, investigative pathology, pharmacology, and physiology. Meeting attendees are diverse and range from academic scientists, government agencies, and professionals from industry. EB provides endless opportunities to explore the ever-expanding field of biomedical research and science.
While glancing through the EB program, inundated by all the sessions offered, I came across one in particular that sparked by interest, “Moving the needle on hypertension: what knowledge is needed?”
It was not your typical session due to the speakers all participating in a panel discussion and debate following their presentations. Dr. Alicia McDonough from the University of Southern California started off the session by exploring the gaps in knowledge about the role of sodium and potassium in hypertension regulation.
As a student studying hypertension, salt is always a topic of conversation that I come across. Potassium, on the other hand, is one that isn’t always given the attention it deserves (see a recent Tweetorial by Dr. Paul Welling)
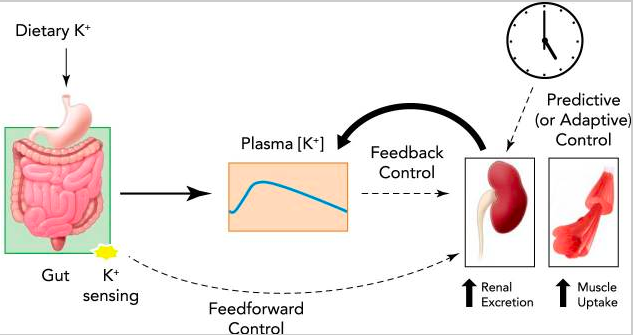
Potassium, an electrolyte that usually takes a backseat to sodium, plays many imperative roles in the human body. The Western diet today consists of high sodium and low potassium food, as the majority of the population choses convenient processed food over fresh produce.
Many papers discuss the importance of decreasing sodium intake to lower blood pressure, however, Dr. McDonough is on the forefront of research providing evidence suggesting that increasing dietary potassium may have an equally important effect on lowering blood pressure. This is also the premise of the well known DASH diet, which emphasizes foods rich in calcium, potassium, fiber, and protein.
Overall, sodium is still a key player in blood pressure regulation, however, potassium is vital for keeping our blood pressure within normal limits. Simply reducing sodium intake may not be enough to control hypertension on its own. Looking at the ratio of sodium and potassium levels is a novel angle while investigating the effects on hypertension. If you would like to read more on potassium homeostasis, check out Dr. McDonough’s recent publication
As a PhD student with a neuroscience background, in a renal physiology lab, and studying hypertension, I was extremely interested in the second speaker. Dr. William Farquhar, from the University of Delaware. He talked about the effects of dietary sodium on brain and blood vessel function.
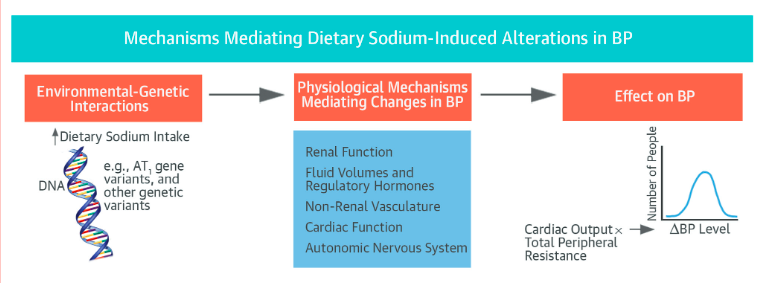
There is copious amounts of research supporting the hypothesis that dietary sodium can unfavorably affect multiple target tissues and organs. Some of those including: the heart, vasculature, kidneys, as well as specific areas of the brain. Overall, in the vasculature, chronic high sodium intake stiffens the arteries and if hypertensive patients reduce their dietary sodium intake, arterial stiffness is significantly reduced.
In the brain, both the effects of hypertension and/or the brain’s effect on blood pressure are less explored. Brainstem nuclei play an imperative role in blood pressure control and may be heavily influenced by sodium, causing a sensitization of sympathetic neurons; specifically in the rostral ventral lateral medulla. Surprisingly, even without the increase in blood pressure, the chronically increased sympathetic outflow alone may have harmful effects of target organs, in specific, the heart (via muscle contractions) and the kidneys (via increased aldosterone levels). To read more on dietary sodium and health, check out Dr. Farquhar’s recent publication
The session concluded with Dr. Richard Wainford, from Boston University, whose talk was titled, “Personalized Precision Medicine Approach to Combat Salt-sensitive Hypertension: Feasible or Fantasy?” Personalized medicine has been a rapidly growing topic.
The pathophysiology of hypertension is one that has a complex web of connected factors such as susceptibility genes, physiological systems, and environmental factors. Taking into consideration unique molecular or risk profiles of specific patients during the diagnostic and screening methods is imperative to better identify the predisposition towards a disease.
The big question is, can we or how can we use this personalized medicine to treat salt-sensitive hypertension? The biggest part of the war against salt-sensitive hypertension is the salt intake itself and the overall lack of consideration by the population of salt levels in the western diet. Recommendations on salt intake vary among sources, however, even with a set recommendation, Western society is inundated with salt in processed food. Changes in sodium intake will only change with market forces, however, a societal approach, and effective education is also a necessity.
Overall, personalized medicine for salt-sensitive populations is feasible, but with the current societal diet trends, I can also see why many physicians see it as being fantasy. To read about a novel biomarker useful for identifying individuals at risk for developing salt sensitive blood pressure, check out Dr. Wainfords recent publication.
There is still an enormous amount to be expounded about the physiology of hypertension and the innate physiological drive for sodium intake. This session’s aim was to examine the newest science in specific areas of hypertension research from the role of both potassium and sodium mechanisms in hypertension development and control; the effects of sodium on the brain; as well as individual variability in sodium intake.
In my opinion, this session achieved its goal. I truly appreciated the way this session was put together and the professional and informative debate between scientific professionals that followed. The level of respect for each professionals unique views and opinions created a very interesting and open conversation that I found to be very effective. I hope future organizers will consider using this format for future sessions as I found it a refreshing and effective arrangement.
This was my first year attending Experimental Biology and as overwhelming as it was, I can’t wait for next year. The cutting edge science being done from the wide range of fields is truly inspiring. Don’t miss out on the excitement of next year’s Experimental Biology hosted in San Diego, CA from Apr. 4th to the 7th in 2020!
Kasey Belanger
PhD student at Augusta University