 When somebody receives a kidney transplant, the current strategy is to hit them hard with immunosuppression initially–using potent medications such as thymoglobulin, Cell-Cept, steroids, and tacrolimus at higher levels–and that medication can generally be tapered to much lower levels with time without putting the patient at any additional risk for rejection.
When somebody receives a kidney transplant, the current strategy is to hit them hard with immunosuppression initially–using potent medications such as thymoglobulin, Cell-Cept, steroids, and tacrolimus at higher levels–and that medication can generally be tapered to much lower levels with time without putting the patient at any additional risk for rejection.
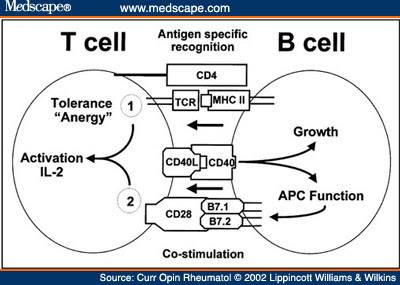
The reason for this stems from the difference between direct versus indirect T-cell stimulation. In the early (e.g. first 3 months) transplant period, donor antigen-presenting cells, typically B-cells, are able to directly stimulate recipient T-cells when the donor MHC itself is recognized as foreign by recipient T-cells. This leds to a robust immune response which is 100x more potent than indirect T-cell stimulation, in which recipient MHC presents processed, donor antigens to recipient T-cells. The late (e.g. after 3 months) immune response is dominated by the indirect immune response since most of the donor B-cells are now dead at this time point, and the indirect immune response is easier to control.

