 Post-transplant lymphoproliferative disorder (PTLD) occurs in < 1% of kidney transplant recipients, but can often be a serious complication. In essence, PTLD is a form of lymphoma which occurs due to decreased immune surveillance as a result of the immunosuppression used to prevent allograft rejection.
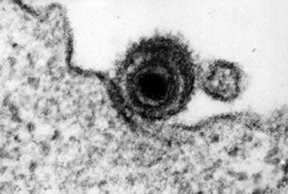
The pathophysiology of PTLD is intimately linked to the Epstein-Barr virus (EBV–pictured on the left attaching to a host cell), a member of the gamma herpesvirus family. It attaches to B-cells and in the absence of immune surveillance may result in hyperproliferation of B-cells leading to a lymphoma. Most often the disease is a systemic one with extensive lymphadenopathy and involvement in multiple solid organs. However there are variants of the disease in which the sole manifestation is within the transplanted kidney itself. The infected cells are almost always from the recipient as opposed to being from the donor.
PTLD is best treated by withdrawing immunosuppresion–often by completely removing CNI inhibitors & MMF while continuing low-dose prednisone. In addition, rituxamab (a monoclonal antibody against CD20, a B-cell antigen) has been noted to have a positive effect (which makes sense since this is almost always a B-cell lymphoma). Chemotherapy such as the CHOP regimen are reserved for patients with PTLD with more worrisome lymphoma-type features.
Post-transplant lymphoproliferative disorder (PTLD) occurs in < 1% of kidney transplant recipients, but can often be a serious complication. In essence, PTLD is a form of lymphoma which occurs due to decreased immune surveillance as a result of the immunosuppression used to prevent allograft rejection.
The pathophysiology of PTLD is intimately linked to the Epstein-Barr virus (EBV–pictured on the left attaching to a host cell), a member of the gamma herpesvirus family. It attaches to B-cells and in the absence of immune surveillance may result in hyperproliferation of B-cells leading to a lymphoma. Most often the disease is a systemic one with extensive lymphadenopathy and involvement in multiple solid organs. However there are variants of the disease in which the sole manifestation is within the transplanted kidney itself. The infected cells are almost always from the recipient as opposed to being from the donor.
PTLD is best treated by withdrawing immunosuppresion–often by completely removing CNI inhibitors & MMF while continuing low-dose prednisone. In addition, rituxamab (a monoclonal antibody against CD20, a B-cell antigen) has been noted to have a positive effect (which makes sense since this is almost always a B-cell lymphoma). Chemotherapy such as the CHOP regimen are reserved for patients with PTLD with more worrisome lymphoma-type features.

