The case against Sunday As A Day Of Rest For the Dialysis Unit: this older study (Bleyer et al, Kidney International 1999) looked at sudden death amongst ESRD patients according to days of the week using data from the USRDS. Here is the key graph showing mortality rates in ESRD patients by days of the week. The black bars represent deaths classified as cardiac arrest, the white bars represent deaths classified as “other cardiac” (e.g., myocardial infarction), and the gray bars represent deaths classified as “non-cardiac deaths.”
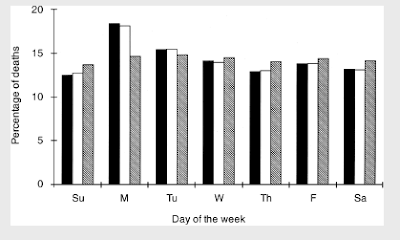
The most striking feature of this graph is that there is a clear spike in cardiac mortality seen on Mondays, and to a lesser degree on Tuesdays. The authors go on to show that patients who are dialyzed on a MWF schedule are most likely to have a cardiac death on Mondays whereas patients who are dialyzed on a TuThSat schedule are most likely to have a cardiac death on Tuesdays. In other words, death is most likely to occur during the long, dialysis-free “weekend”. Patients on peritoneal dialysis in contrast showed relatively constant mortality rates throughout the days of the week as compared to hemodialysis patients.
There are numerous potential explanations for these findings. Intradialytic weight gain is understandably higher over a 72-hour period compared to a 48-hour period, and fluid shifts during ultrafiltration might be more liable to result in hypotensive episodes that would be predicted to be particularly dangerous in those with underlying cardiovascular disease. Potassium or calcium levels may fluctuate more and therefore be more likely to result in arrhythmia. Overall, the Monday/Tuesday “mortality spike” in ESRD patients appears to reflect the intermittent nature of the currently popular three days a week dialysis strategy, and potentially points to a benefit for a more constant (e.g., daily, 6x/week, PD, etc) dialysis schedule, though this latter point remains a controversial one.



Dear Nathan, thank you for your last two posts on USRDS data and the American tragedy called dialysis. I look forward to hearing more about quotidian dialysis on your site.
Peter Laird, MD
http://www.billpeckham.com
Dialysis from the Sharp End of the Needle