 Cisplatin based therapy for the treatment of solid organ tumors is commonly associated with several renal abnormalities including;
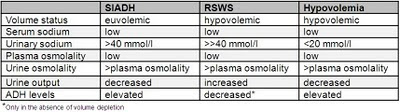
Cisplatin based therapy for the treatment of solid organ tumors is commonly associated with several renal abnormalities including;Renal salt wasting syndrome (RSWS) due to cisplatin has rarely been reported and is often confused with SIADH as a cause of hyponatremia (as discussed by Nate in a prior post). Increased urinary sodium (more than the intake) and increased urinary output in a hypovolemic patient are the key findings that help in differentiating this entity from SIADH (Table). Knowing this difference between these entities is important as RSWS is treated with sodium supplementation as opposed to water restriction with SIADH. Cerebral salt wasting has similar presentation as RSWS but has an associated cerebral lesion.
How hyponatremia occurs with cisplatin therapy can be understood by reviewing the mechanism of cisplatin nephrotoxicity. Briefly, cisplatin is a tubular nephrotoxin and causes;
- Dose dependant nephrotoxicity by particularly affecting the S3 segment of the proximal tubule, and to a lesser extent the loop of henle and the distal collecting system.
- Cisplatin enters the cells via the OCT2 transporters on the basolateral surface.
- Leads to decreased ATPase and mitochondrial activity.
- Activates proinflammatory cytokines
- Induces hypoxia
- All of which contribute to cell apoptosis and death.
Cisplatin, interestingly, may decrease the abundance of aquaporin channels in the cortical and medullary collecting duct, as shown in animal studies, thereby further contributing to impaired urinary concentration and polyuria. This may, in fact, limit the degree of the hyponatremia (secondary to decreased water reabsorption) that develops with salt wasting from proximal tubule dysfunction. Not surprisingly, patients with cisplatin nephrotoxicty often tend to be quite polyuric.
In conclusion, why cisplantin induced RSWS occurs so rarely, is unclear. It is possible that the condition may be under reported or frequently overlooked.
Viresh Mohanlal, MD



Thanks for the comment and citation. I will add the Pubmed link
to that article
http://www.ncbi.nlm.nih.gov/pubmed/3337511
Matt: as this was my case recently, just wanted to add one other clinical piece. In one of the orginal case series (Kaysen, et al, Annals of IM, 1988), they described the use of Fludrocrtisone in the setting of salt wasting. Fortunately, this pt responded to 0.9 NSS IV. BTW, his sodium fell to 112 ( despite use of Demeclocycline) Thanks. PSegal DO
http://www.ncbi.nlm.nih.gov/pubmed/20110413
This is a basic science paper in mice addressing this very issue. Looking at renal function in mice is not a trivial issue (as we do this in our lab). This study only showed partial protection of kidney damage with cimetidine. I could not find any human studies on the subject
good post, is there any data on cimetidine to attenuate cisplatin nephrotoxicity, via blockade of of the OCT channel?
thanks for the comment, typo- meant to say "water" restriction instead of "sodium" restriction for SIADH treatment, this has been changed.
As for aquaporin downregulation, you are correct in that decreased aquaporin levels by itself would likely lead to hypernatremia.
In this scenario (cisplatin toxicity) you have proximal tubule injury leading to salt wasting in combination with polyuria so that these patient have a combination of defects. I would speculate that the aquaporin down regulation might, in fact, be somewhat protective so that the patients don't develop even more profound hyponatremia from the salt wasting alone.
"sodium" restriction for SIADH or do you mean "free water" restriction? also, I'm confused about somthing: wouldn't downregulation of aquaporin channels cause aquaresis and HYPERnatremia, not HYPOnatremia? thanks.