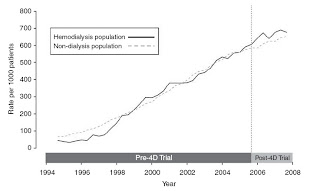
 It can often be difficult to stop something once it’s been started; take statins for example. It seems that despite consistent evidence from two large, randomized controlled trails demonstrating the lack efficacy of statins for preventing cardiovascular mortality in dialysis patients, there has been little impact on the prescribing habits of nephrologists. This study shows that in the 2 years following the negative 4D result, the rate of statin prescription in diabetic hemodialysis patients actually increased by 10%.
It can often be difficult to stop something once it’s been started; take statins for example. It seems that despite consistent evidence from two large, randomized controlled trails demonstrating the lack efficacy of statins for preventing cardiovascular mortality in dialysis patients, there has been little impact on the prescribing habits of nephrologists. This study shows that in the 2 years following the negative 4D result, the rate of statin prescription in diabetic hemodialysis patients actually increased by 10%.There are probably several reasons for this practice, such as scepticism about the result in ESRD patients given the proven efficacy of statins in other groups, or a reluctance to engage in therapeutic nihilism. Personally, I worry about precipitating a cardiovascular event by stopping these drugs; the 4D and Aurora trials do not address the issue of discontinuation. With such a high rate of cardiovascular events in this population, aren’t you just asking for trouble by drawing a line through the Lipitor on the medsheet? It’s a thorny question, and one we may put to poll on this blog next week.



You can't have it both ways.
Nice post. This is definitely a tough issue. Although I no longer feel compelled to start statins on dialysis pts, I do not feel strong enough to advocate enthusiastically for discontinuation.