 Much of medical residency training in the US is centered in the hospital. This is also true of many of the fellowship programs in internal medicine. As we have seen a continual increase in the number and acuity of patients admitted to the hospital. The number of house staff have remained static. The busy nephrology fellow spends a majority of time rounding on inpatient services, answering consults or arranging renal replacement therapy for patients already on some form chronic dialysis who happen to be admitted to the hospital. Typically, outpatient exposure to CKD and transplant come during the fellow’s weekly continuity clinic. However, obtaining adequate exposure to patients on some form of chronic dialysis performed either in-center or at home can be challenging. An online survey of 133 recent nephrology graduates (2004-2008) published in the March 2010 CJASN showed that 81% were well-training in caring for primary care issues in patient with CKD/ESRD. They also showed that 80% felt that they were well-trained/competent in in-center hemodialysis, but 60% and felt that little or no training was offered in home HD. This same survey showed that 78% had little or no training in dialysis unit directorship. The majority of respondents to this survey were recent graduates (>2 years since fellowship).
Much of medical residency training in the US is centered in the hospital. This is also true of many of the fellowship programs in internal medicine. As we have seen a continual increase in the number and acuity of patients admitted to the hospital. The number of house staff have remained static. The busy nephrology fellow spends a majority of time rounding on inpatient services, answering consults or arranging renal replacement therapy for patients already on some form chronic dialysis who happen to be admitted to the hospital. Typically, outpatient exposure to CKD and transplant come during the fellow’s weekly continuity clinic. However, obtaining adequate exposure to patients on some form of chronic dialysis performed either in-center or at home can be challenging. An online survey of 133 recent nephrology graduates (2004-2008) published in the March 2010 CJASN showed that 81% were well-training in caring for primary care issues in patient with CKD/ESRD. They also showed that 80% felt that they were well-trained/competent in in-center hemodialysis, but 60% and felt that little or no training was offered in home HD. This same survey showed that 78% had little or no training in dialysis unit directorship. The majority of respondents to this survey were recent graduates (>2 years since fellowship).
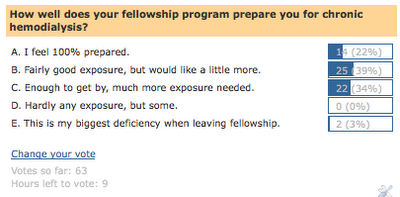
RFN decided to conduct a poll to see whether or not nephrology fellows were well-prepared to attend chronic outpatient hemodialysis clinics. Our results were a little different than the one published in CJASN. Out of 63 total respondents to our poll, only 14 or 22% felt that they were 100% prepared for chronic hemodialysis clinics. 25, or 39% felt that they had good exposure, but would like more. Interestingly, 22 or 34% of respondents indicated that much more exposure was needed. What do we make of this poll? It is clear that nephrology training is heavily centered in the hospital. How do we shift our focus out of the hospital to gain not only more exposure to chronic “stable” patients, but more longitudinal continuity of care? This is really where learning happens. Following patients on a long term basis is the only way to learn about the ever changing nutritional, access related, weight adjustment etc. etc. etc. issues that patients on chronic renal replacement therapy have. I would be interested to hear about the different outpatient experiences fellows from programs around the US and world have. We typically spend 6 consecutive months dedicated to following a group of patients on a given dialysis shift with the close supervision of an attending. Patients are seen weekly while on dialysis. Fellows with an interest in home-hemodialysis or nocturnal dialysis can choose to follow these patients as well. This allows for the fellow to have a great deal of continuity of care. In conclusion, from the results of the RFN poll it appears that nephrology fellows are wanting more exposure to chronic hemodialysis. Trying to balance each of the different areas of nephrology education can be difficult, but chronic dialysis needs to be a centerpiece of any successful fellowship program.


Michelle- I don't think this is the case. First off- A majority of fellows who responded to this poll (which is not scientific) felt that they were well prepared for chronic dialysis. 34% indicated that they knew enough to get by, but merely wanted more exposure. We have no way of knowing who answered the poll or what stage of training they are in. I did include a published article which did show that a majority of graduates feel well prepared.
Oh,jeez! This is disturbing. I'm about to start dialysis, and knowing that the majority of nephrologists don't feel well-trained enough in dialysis is disconcerting, to say the least. Why is that? Seems like once a CKD patient transitions to dialysis, s/he is pretty much forgotten and relegated to the dust heap.