We have recently
posted about problems using warfarin in renal patients. On a similar note, I was recently involved in the care of a 58-year-old African-American patient who presented with oliguric AKI and a supratherapeutic INR level of 14.9 while on warfarin therapy for pulmonary embolism. Although AKI was probably secondary to ischemic ATN from massive bleeding (requiring 11 units of PRBCs), this patient made me wonder whether warfarin could itself cause AKI in the absence of significant hemodynamic changes.
It has been suggested that warfarin may induce AKI by causing
glomerular hemorrhage and
renal tubular obstruction by RBC casts.
The first report by Abt, et al observed glomerular hematuria in a patient with excessive warfarin anticoagulation with underlying structural abnormality of glomerular basement membrane, suspected warfarin-induced glomerular hematuria. This finding was also noted by
Kabir et al and
Brodsky et al. subsequently reviewed
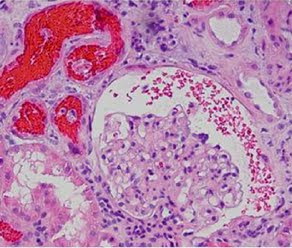
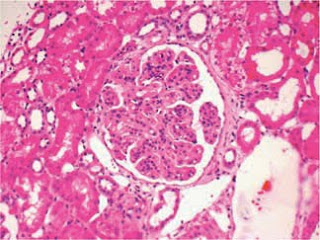
renal biopsies from 9 patients with elevated serum creatinine level (mean, 4.3±0.8 mg/dL) and abnormal INR (mean, 4.4±0.7 IU) after excluding acute/active glomerulonephritis. INR was normalized before the kidney biopsy. The biopsy specimens revealed RBCs in both Bowman spaces and tubules. The occlusive RBC casts were mostly localized to distal nephron segments. The presence of RBCs was
unlikely related to the biopsy procedure as the distribution of RBCs was within the nephron, non-uniform, and not in the interstitium or around the edges of the biopsy specimens. Moreover, the presence of occlusive
RBC casts compressing tubular epithelium suggested glomerular hematuria. All of these patients had underlying kidney disease.
Recovery was incomplete in six of nine patients. Based on this review, it seems that warfarin is unlikely to cause AKI in patients with normal renal parenchyma. However, elderly patients with underlying kidney diseases may be at risk for developing warfarin-associated AKI by this mechanism.
In addition to this potential renal complication of warfarin therapy, there were 2 case reports of warfarin-induced AIN by Volpi et al. and Kapoor et al. The latter case reports a patient on warfarin for 2 months for DVT who presented with AKI, supratherapeutic INR and skin rash. Renal biopsy revealed AIN and punch skin biopsy showed LCV with high eosinophil count, highly suggestive of drug-induced reaction after a negative comprehensive work-up and the absence of other recent medication changes. Warfarin was withdrawn and the patient’s renal function began to resolve upon discharge. Spontaneous cholesterol embolization is also widely reported in patients with diffuse atherosclerosis on anticoagulation.
In summary, it appears that in patients with pre-exiting CKD, warfarin may precipitate AKI via either glomerular hemorrhage and intra-tubular obstruction, AIN, spontaneous cholesterol embolization, in addition to hemodynamic change secondary to massive blood loss. This should be borne in mind in cases of AKI in patients taking warfarin, when diagnosis is unclear.
Boonsong Kiangkitiwan, M.D.

asd
i want expert comment on following issues on EM proven MPGN Type2(DENSE DEPOSIT DISEASE):
1)Current role of concurrent use of Tacrolimus,MMF,Prednisolone
2) Role of warfarin.
DR.KAILASH SHEWALE,MD,DNB(NEPHRO)
NASHIK.MAHARASHTRA,INDIA.
Thanks for feedback – will keep this in mind for a future post
I was wondering if you were interested in exploring the link between Immunosuppresant therapy for renal transplants recipients and Lymphomas.
We also have seen a warfarin induced AIN (biopsy proven) at our institution.