 In the evaluation of patients with hyponatremia (serum Na less than 135 mEq/L), differentiating hypovolemia from euvolemia is often challenging, particularly if the history and physical findings are unrevealing and frequently leads to misdiagnosis. This conundrum exists even for the nephrologists and often leads to guesswork. Measuring the antidiuretic hormone (AVP) levels is not helpful as most cases of hyponatremia have either appropriate or inappropriate elevation of AVP levels and despite frequent reliance on central venous pressure (CVP) measurements to determine the volume status, they are rarely measured in hypovolemic or euvolemic states and their accuracy is debatable.
In the evaluation of patients with hyponatremia (serum Na less than 135 mEq/L), differentiating hypovolemia from euvolemia is often challenging, particularly if the history and physical findings are unrevealing and frequently leads to misdiagnosis. This conundrum exists even for the nephrologists and often leads to guesswork. Measuring the antidiuretic hormone (AVP) levels is not helpful as most cases of hyponatremia have either appropriate or inappropriate elevation of AVP levels and despite frequent reliance on central venous pressure (CVP) measurements to determine the volume status, they are rarely measured in hypovolemic or euvolemic states and their accuracy is debatable.
Reliance on the urine biochemical parameters therefore becomes necessary. Urine electrolytes particularly low urine sodium (less than 30 mEq/L) is often used to distinguish these two conditions but can be misleading, as up to 30% patients with hypovolemia may have elevated urine sodium and on the flip side, up to 40% SIADH patients may have low urine sodium (low salt intake). A recent CJASN review of SAIDH nicely covers this. Urine osmolality is often elevated (greater than 100mosm/kg) and does not distinguish hypovolemia from euvolemia. Recent studies have therefore suggested that a combined use of urine sodium (UNa), fractional excretion of sodium (FENa) and fractional excretion of urea (FEUrea) would best help in differentiating these two states (diuretic use, renal failure, hypocortisolism and hypothyroidism excluded).
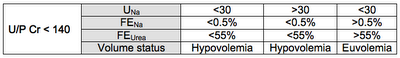 2) In patients with low urine flow (urine/plasma Cr greater than 140) an even lower FENa (less than 0.15%) and FEUrea (less than 45%) are recommended to capture all the cases of hypovolemia.
2) In patients with low urine flow (urine/plasma Cr greater than 140) an even lower FENa (less than 0.15%) and FEUrea (less than 45%) are recommended to capture all the cases of hypovolemia.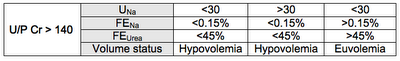 Low serum uric acid levels (less than 4mg/dL) and increased fractional excretion of uric acid (greater than 12%) are also useful in differentiating SIADH from hypovolemia, major exception being salt wasting syndromes (click here for review or here for a discussion about CSW vs. RSW). In these patients, unlike SIADH, correction of hyponatremia does not lead to improvement of hypouricemia and uricosuria, likely due to persistent proximal tubular defect causing impairment of uric acid absorption. Phosphaturia (FEPO4 greater than 20%), for the same reason also favors salt wasting, at least initially. Moreover, the plasma renin activity and plasma aldosterone levels are elevated in salt wasting but low in SIADH.
Low serum uric acid levels (less than 4mg/dL) and increased fractional excretion of uric acid (greater than 12%) are also useful in differentiating SIADH from hypovolemia, major exception being salt wasting syndromes (click here for review or here for a discussion about CSW vs. RSW). In these patients, unlike SIADH, correction of hyponatremia does not lead to improvement of hypouricemia and uricosuria, likely due to persistent proximal tubular defect causing impairment of uric acid absorption. Phosphaturia (FEPO4 greater than 20%), for the same reason also favors salt wasting, at least initially. Moreover, the plasma renin activity and plasma aldosterone levels are elevated in salt wasting but low in SIADH.
Although the interesting findings in these studies need further validation, they offer a completely different perspective and help us move away from complete reliance on assessment of volume status to make a correct diagnosis of hyponatremia, an exercise that often involves guesswork. Hopefully, the next time when we encounter hyponatremia, this new approach would help us to stop guessing.
Viresh Mohanlal, MD.


No.If you read the article, Una is not reliable in euvolemis states always but the combination of Una, FENa and FEurea is.In the second column, although UNa is <30, patient has FEUrea and FENa that is high,hence patient is likley euvolemic. UNa can be low if your solute intake is low in a steady state.Hope that answers your question.
for the second table ,for making a volume status euvolemic ,shouldnt the urinary Na excretion be > 30 meq/L
very nice. thanks for posting