EPS is quite rare, but has a high associated mortality (25-50%). It is relevant even for those of us who take care of few/no PD patients, as over half of all cases present after changing from PD to HD and it can even present post renal transplantation.
So what is EPS? Basically, it is an inflammatory condition, characterized by severe peritoneal fibrosis and thickening, leading to adhesions, small bowel obstruction and ascites formation. It occurs in between 0.5- 2.8% of PD patients and is seen primarily in patients who have been on PD for over 5 years, with risk increasing as time on dialysis increases (Up to 17% in those on PD over 15 years). However, there have been reported cases in patients on PD for less than 6 months. Frequently, patients have had recurrent episodes of peritonitis although again, this is not universal. Infection is thought to ‘prime’ the membrane for fibrotic change and may be a precipitating event.
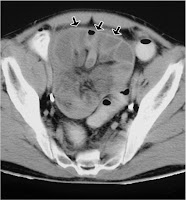
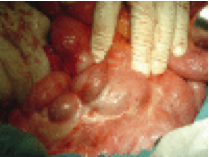
The clinical presentation can be quite vague, so a high degree of suspicion is needed to make the diagnosis. Patients may present as ‘failing’ PD but EPS should be considered in any patient with persistent GI symptoms and declining nutritional status either while on PD or after transfer to HD. Commonest complaints include decreased appetite, early satiety, nausea and vomiting. Recurrent episodes of small bowel obstruction are seen in severe cases. In the right clinical setting, bloody dialysate (PD) or recurrent +/- bloody ascites (HD) may also point to EPS. Abdominal CT scanning can be helpful (as above). However, direct visualisation with laparoscopy and peritoneal biopsy are sometimes needed to confirm the diagnosis. Interesting reviews on the condition are here and here.
Martina McGrath MD

I think one way of dealing with this problem of EPS is to train patients who are already used to self care peritoneal dialysis (PD) at home in home hemodialysis (HD) care. With this paradigm shift, it will be easy for patients to maintain their independence of in-centre HD care. This will be a good way for patient management in the near future.
I'd never heard of this! So, are you saying that perhaps those on PD who have had at least one bout of peritonitis should be particularly vigilant for signs of "failing to thrive" and suspect this condition? Is this a risk that PD patients are routinely made aware of as they initiate dialysis?