 A woman in her 30’s presented with five years of severe hypertension, uncontrolled on trials of four or five agents over the past few years. She had had preeclampsia nine years ago that resolved after delivery, and for the next four years she was reportedly normotensive. Her hypertension had been diagnosed five years ago when she developed disabling headaches. Despite attempts at medical control, she continued to have systolic BPs over 200 mmHg, and diastolic BPs over 100 mmHg. In the past year, she had been hospitalized several times for syncopal episodes. Each time, her BP on arrival in the ED was >200/100. Cardiac and neurologic workups were repeatedly negative. According to the patient, she had had numerous urine and blood tests, which failed to yield an explanation for her hypertension. She did not remember having a renal ultrasound, but said she had had a CT which showed “my kidneys were in the wrong place”.
A woman in her 30’s presented with five years of severe hypertension, uncontrolled on trials of four or five agents over the past few years. She had had preeclampsia nine years ago that resolved after delivery, and for the next four years she was reportedly normotensive. Her hypertension had been diagnosed five years ago when she developed disabling headaches. Despite attempts at medical control, she continued to have systolic BPs over 200 mmHg, and diastolic BPs over 100 mmHg. In the past year, she had been hospitalized several times for syncopal episodes. Each time, her BP on arrival in the ED was >200/100. Cardiac and neurologic workups were repeatedly negative. According to the patient, she had had numerous urine and blood tests, which failed to yield an explanation for her hypertension. She did not remember having a renal ultrasound, but said she had had a CT which showed “my kidneys were in the wrong place”.
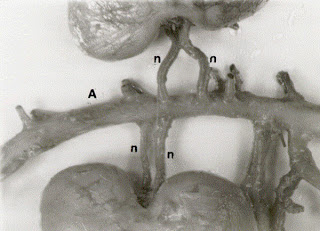
Workup in our clinic included normal renin and aldosterone levels (even on an ACEI, which should have increased plasma renin/aldo), and normal plasma metanephrines, VMA, and cortisol levels. She was not on oral contraceptives. Creatinine was normal, although she had trace urine protein on dipstick. Renal CT angiogram is where things got more interesting– she had a single pelvic kidney, with duplicated renal arteries and a third, accessory artery coming off the aorta to supply the posterior aspect of the kidney. There was no evidence of arterial stenosis, and no hydronephrosis. Her adrenals appeared normal.
I must admit, I am a little stumped about why this woman has such severe hypertension. However, I came across a possible explanation while doing a literature search, and wanted some feedback from this readership. Could her anomalous renal arterial anatomy have something to do with her high blood pressure?
In the 1950s, several autopsy studies suggested that persons who were hypertensive were much more likely than normotensive persons to have multiple renal arteries (somewhere around 70%). These studies were subsequently contradicted by several series of renal angiograms, which did not show an increased incidence of multiple renal arteries among hypertensive persons. Number of renal arteries and whether both kidneys were involved were not evaluated by most of the studies, nor was arterial length or diameter. It appears as though somewhere between 20 to 30% of the population has at least one additional renal artery, though the jury on whether there is an association with hypertension is still out.
The thinking behind the connection is presumptively that narrower and/or longer accessory renal arteries have decreased blood flow compared to a single renal artery; hence, renin secretion is increased. While this mechanism might result in increased blood flow to a normal kidney in a person who has only one kidney with multiple renal vessels (and may downregulate renin secretion in the normal kidney), I wonder what the effect would be on my patient, with her solitary kidney. The problem with this theory is that her renin and aldo levels were normal. However, I’m low on other ideas.
Please let me know what your thoughts are! I’m curious to know if anyone else has had experience with hypertension in patients with anomalous renal arterial blood supplies.


I have a young 22 years female with hypertension refer to me to rule out secondary causes of hypertension.
On investigation she had high renin and aldosterone. Based on that I suspected renovascular cause and advised CT Renal angio. On CT she had bilateral dual renal artery without stenosis.
I am still searching for mechanism responsible for hypertension.
Orthostatic hypertension: when pressor reflexes overcompensate
Joshua Fessel and David Robertson
Nature Clinical Practice Nephrology (2006) 2, 424-431
doi:10.1038/ncpneph0228
Received 26 October 2005 | Accepted 31 March 2006
This is about the best I can do, there really isn't much out there. So often it is missed because of the lack of orthostatic measurement, or simply dismissed as anxiety until it becomes a known issue.
POTS often has paradoxically low renin/aldosterone levels in spite of chronic hypovolemia. A rarer form, hyper-adrenergic POTS has upright hypertension that can be difficult to treat due to excessive levels of or response to norepinephrine. She could have autonomic changes due to sympathoexcitation from chronic hypovolemia or undiagnosed POTS. Both POTS and preeclampsia share a low circulating total blood volume.
The preeclampsia (hypovolemia,) hypertension and syncope make question a possible autonomic issue.
No, we didn't check orthostatics, but can at next visit. Do you think her sympathetic nervous system responsiveness would have been affected by preeclampsia-related hypovolemic changes? BTW a post on orthostatic hypertension would be great.
Damage from chronic hypovolemia (suggested by history of preeclampsia)? Were orthostatic vitals ever checked? Orthostatic HYPERtension can have serious consequences and is often overlooked.