Dihydropyridine (DHP) calcium channel blockers are notoriously associated with dependent oedema, but what mechanisms underlie the pathogenesis of this finding? Here are some explanations from a nice review I came across.
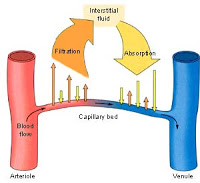
Going back to Starling’s forces governing the formation of interstitial fluid – net capillary fluid filtration is influenced by hydrostatic pressure, oncotic pressure, capillary permeability and lymphatic drainage.
Upon change in posture from lying to standing, hydrostatic pressure in the vessels of the lower extremities increases. However, this is held in check by autoregulatory mechanisms which cause protective vasoconstriction via local sympathetic reflexes and myogenic reflexes – the latter are caused by smooth muscle contractions in response to increased vessel transmural pressure.
These myogenic reflexes are mediated in part by L-type DHP sensitive calcium channels. They allow calcium influx, causing pre-capillary smooth muscle constriction, thereby reducing hydrostatic pressure in the capillary bed – the final result is guarding against increased interstitial fluid accumulation.
DHP calcium channel blockers can prevent the entry of calcium to smooth muscle cells, preventing this protective pre-capillary vasoconstriction, facilitating the formation of dependent oedema. In patients with already impaired autoregulation (e.g. diabetics) calcium blockers may be associated with more profound leg oedema than others. Of course, there are likely other factors at play, including increased capillary permeability and other local neurohormonal influences.