Diabetic nephropathy (DN) is well recognized by the glomerular basement thickening (GBM), mesangial matrix expansion and formation of nodules in the mesangium – the classic Kimmelsteil Wilson lesions. The very sight of these lesions makes a pathologist confirm the diagnosis of DN. However it`s not always as straightforward as it seems and these typical lesions do not always dominate the microscopic picture.
Crescents always makes us wonder about the presence of underlying immune-mediated disorders. We investigate the patient extensively with antibody profiling, complement work up and other battery of tests. Sometimes a crescent may appear unexpectedly in the biopsy of a diabetic patient. A diabetic patient can have ANCA vasculitis after all. If the clinical picture is suggestive of immune disorder, the work up for these diseases will help in arriving at the diagnosis. Immunofluorescence and electron microscopy are also crucial in this regard.
But what if it is a crescent of non-immune etiology? Also described as superimposed lesions of collapsing glomerulopathy (CG) on DN, it is characterized by proliferation of parietal epithelial cells (PECs). These ‘crescents’ do not show inflammatory cells and GBM has continuity, without any breaks and there is no fibrin in the Bowman space. CG lesions in DN are associated with an increased rate of progression of disease with earlier onset of ESRD. PEC markers like Claudin-1 show strong positivity in Bowman space in these lesions. In fact the cells in Bowman`s space in these crescents show double positivity with Claudin-1 and Nephrin (a visceral epithelial cell marker) in one study. This indicates de-differentiation of PECs into podocytes, forming cross bridges across the urinary space with the PECs trying to replace the latter as podocytopenia is a prominent feature in DN.
There are no definite treatment recommendations for these lesions in DN. Based on few case reports available, aggressive control of diabetes, hypertension and use of ACEI/ARB`s might help to some extent. But the overall prognosis is grim. This highlights the need for careful assessment of such patients. Diabetic patients may have true crescentic , but not all ‘crescents’ in diabetes are crescentic glomerulonephritis!
Post by Sriram Sriperumbuduri
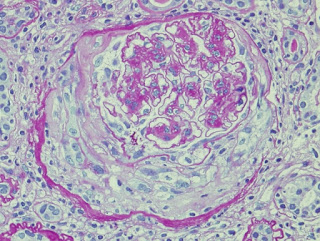
Image from http://renalpathologyreview.blogspot.co.uk/2013/04/diabetic-nephropathy-with-crescents.html



Thank you for sharing such a helpful blog. This really helps me because my father is suffering from Diabetes. Thank you so much for post it.
Agree with you. Probably represents a subset of Diabetic nephropathy with aggressive progression,& poor response to available treatment. History of prolonged periods of poor glycemic & hypertension control usually present.