A 20-year-old female had Henoch-Schönlein purpura since age 9 leading to ESRD. She underwent kidney transplantation in 2018 from a live donor (mother) and received induction immunosuppression with thymoglobulin (100 mg once) followed by maintenance with tacrolimus (6 mg twice a day), mycophenolate sodium (720mg twice a day) and prednisone (30mg daily). The patient was discharged 5 days after surgery, with creatinine 0.9 mg/dL with tacrolimus trough level of 9.2 ng/mL.
Before surgery, the hemoglobin level ranged from 12.1g/dL to 11.6g/dL. At the time of medical discharge Hb was 9.8g/dL.
During the follow-up, the patient was asymptomatic, with no increase in creatinine level and with good trough tacrolimus level (range of 8-12 ng/ml). However, at 2 months post-transplant, she developed worsened anemia with a hemoglobin of 6.1g/dl. At this time, the patient remained asymptomatic. She was then referred to the ED.
The exams at the time showed: hemoglobin 6.2 g/dL; reticulocyte 0.29%; haptoglobin 89 mg/dL; LDH 220 U/L.
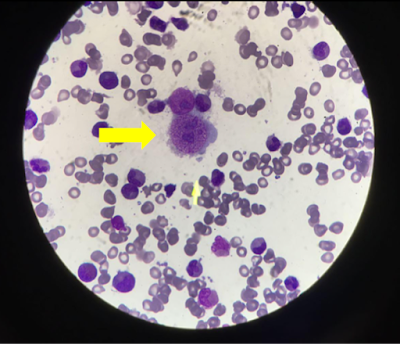
Subsequently, a bone marrow aspirate was performed and showed a giant pronormoblast with prominent nuclear inclusions, characteristic of parvovirus B19 infection.(FIGURE 1)
The patient received 2 doses of intravenous immunoglobulin (1g/kg/day) and was switched from tacrolimus to everolimus.
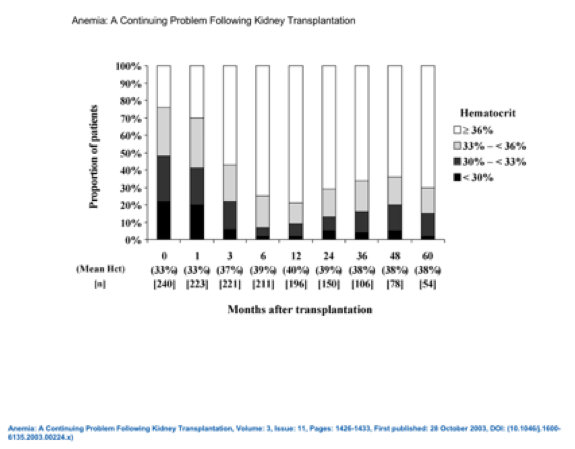
Anemia is a very common finding during post-kidney transplant consults. It is not uncommon to have patients that remain with anemia in the first 3 moths after the procedure.
Read more here. (FIGURE 2)
The lack of large case series would make us imagine that parvovirus B19 infection after kidney transplant is rare. The incidence in post-transplant is not easy to estimate (range from 1-10%) and mostly occur in the first year, suggesting donor transmission, as described here. Also, anemia is a common finding after kidney transplant and may have many other differentials that would appear higher on the list, including drug-induced myelosuppression and bleeding. Additionally, parvovirus B19 surveillance is not performed in routine clinical practice.
A 2006 review from Mayo Clinic showed that among 98 patients with PVB19 infection after transplantation, 54% were kidney transplants, 9% liver transplants, 12% heart or lung transplants and 24% autologous or allogeneic HSCT recipients.
The mean age of the patients was 35.2 ± 17.1 years. The majority (58%) were male.
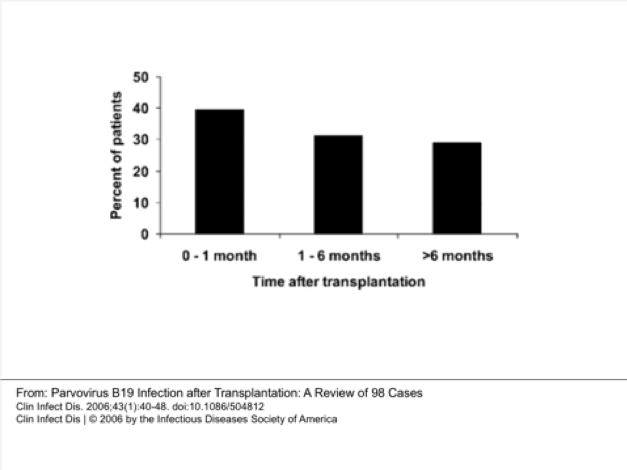
The median time to onset of parvovirus B19 disease was 1.75 months (range, 1 week–96 months) after transplantation. Overall, this study suggested that kidney recipients are in particular susceptible to parvovirus infection and that timing of presentation is variable though highest in the early period post-transplant.
(FIGURE 3). Finally, it is reasonable to think that the magnitude of parvovirus B19 infection is underestimated.
Dr Felipe Paste
São Paulo, Brazil