The use of extracorporeal therapies, like dialysis, is a core part of nephrology training and practice. Fellowship programs spend a considerable amount of time delivering educational content aimed at kidney replacement therapies (KRT). This included hemodialysis, home-based dialysis, peritoneal dialysis, plasmapheresis, and continuous renal replacement therapy (CRRT) in the intensive care unit (ICU). One of the fundamental principles of delivering dialysis is the need to calculate what dose of dialysis is being delivered. How do we measure effectiveness? How much is enough? What modality? How often?
Scribner said in 1963
“If the treatment of chronic uremia cannot fully rehabilitate the patient the treatment is Inadequate”.
Since then, the term adequacy has been used to refer to the adjustment of KRT prescription. While completing my chronic hemodialysis rotation during my nephrology fellowship at Instituto Nacional de Nutrición in Mexico City, I rounded on 3 full shifts of patients every day from Monday to Saturday. Each shift I made notes, adjusted treatments, and completed transplant protocols. During this time, I became interested in urea kinetics and I started to calculate every urea kinetic parameter on patients. Patients normally get blood urea nitrogen (BUN) samples taken pre and post treatment every month, and only single pool Kt/V (spKtV) is recorded. However, I wanted everything; the equilibrated Kt/V (eKtV), standard Kt/V (stdKtV), normalized protein catabolic rate (nPCR), urea distribution volume (V), and equivalent continuous clearance. After performing a couple of these formulas by hand, I realized it was not practical and would benefit from a handy application on my phone to help me. To my surprise, the ones available were incomplete, not user friendly, or even worse they were expensive. With my disappointment and basic excel skills I computed every formula into a spreadsheet and gave it a format to look like a calculator. I called it,”The Adequacy Calculator”. I refined this to the “Adequator” after some time. While doing this, I noticed that the concepts became clearer when you manipulated the parameters to see how different scenarios change dose. For me, using the Adequator allowed me to really understand how dialysis was able to remove a particular substance and how changing different parameters led to changes in adequacy.
With the altruistic help of a very good friend, the spreadsheet became a mobile phone application (app). The Adequator contains three major sections:
- Intermittent therapies: Hemodialysis (HD) and Hemodiafiltration (HDF)
- Continuous Renal Replacement Therapies (CRRT)
- Therapeutic plasma exchange (TPE)
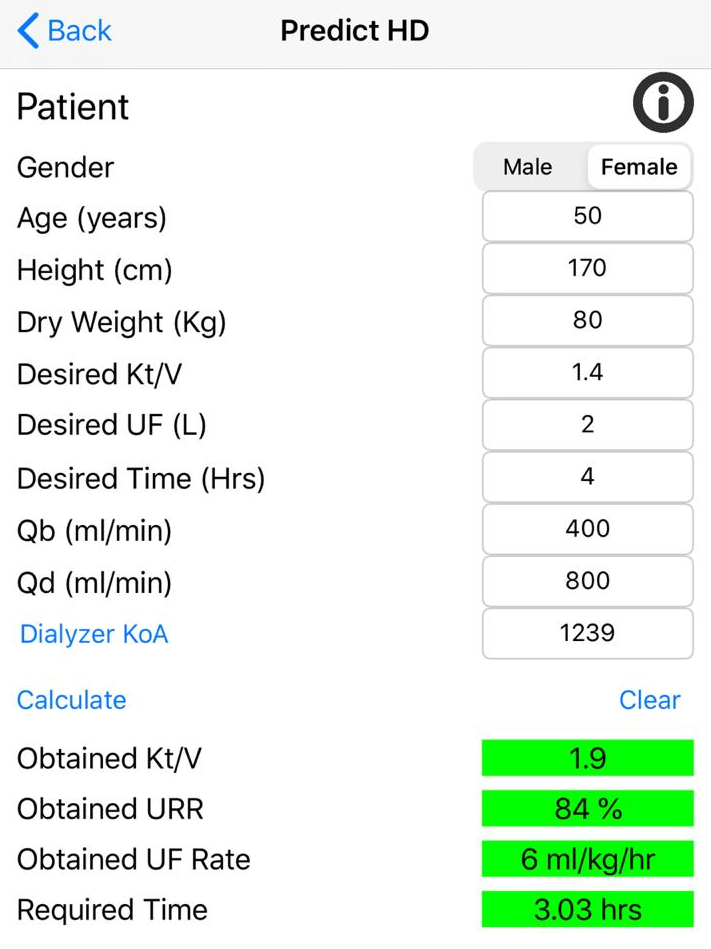
The Intermittent therapy section consists of two calculators for each modality HD and HDF. One calculator is used to evaluate and the other is to predict a hypothetical dialysis session. For example we want to predict the hypothetical session of a 50-year-old Woman: The session will be 4 hour long, Qb of 400 ml/min, Qd of 800 ml/min, 2 L fluid removal and a dialyzer with a KoA of 1239 ml/min. The Adequator predicts the urea reduction ratio (URR), eKtV, ultrafiltration (UF) rate and gives the required time needed to achieve the desired eKtV.
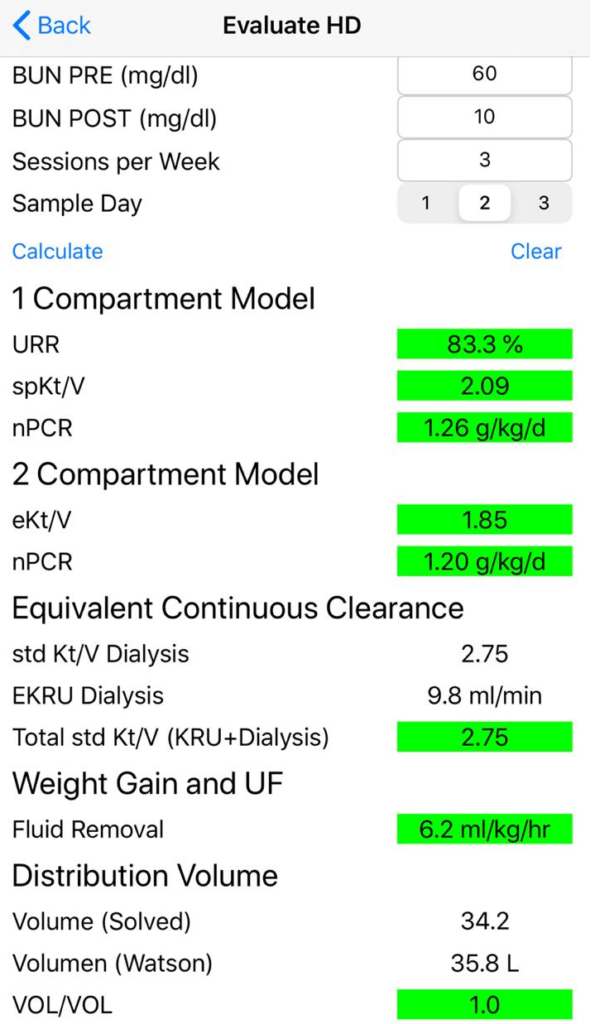
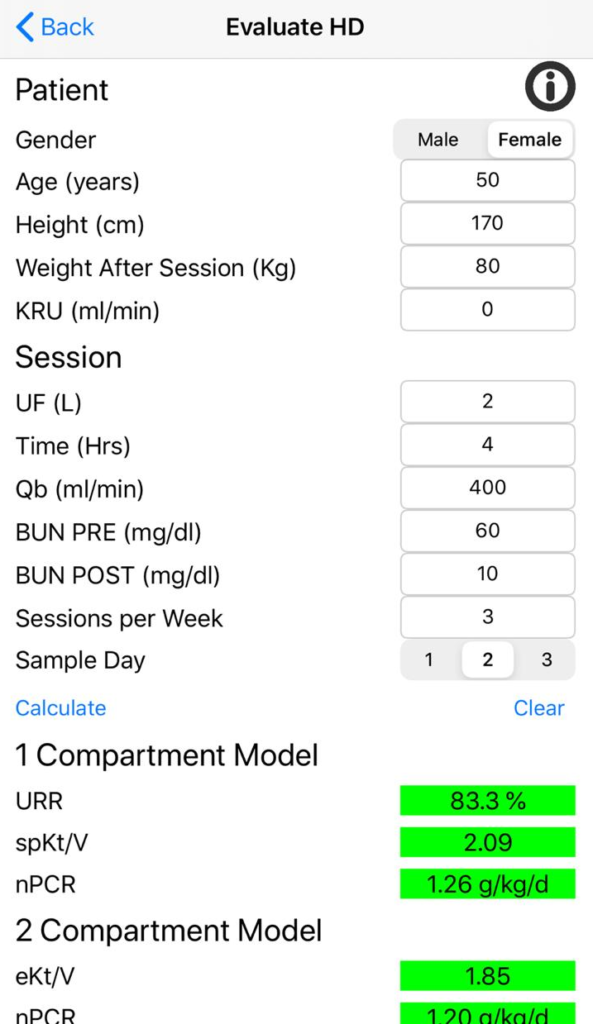
In this example scenario, the session was actually delivered and BUN samples pre and post treatment were 60 mg/dl and 10 mg/dl respectively. The patient has no residual kidney function, receives 3 sessions per week and the samples were taken on the second day of the week. The Adequator evaluates the session by calculating the KtV and nPCR for both 1 and 2 compartment models, equivalent continuous clearances, ultrafiltration rate and urea distribution volume.
The CRRT section is divided into three calculators:
- Prescription
- real delivered dose
- regional citrate anticoagulation (RCA).
- The prescription calculator works as a step method: Patient characteristics and desired dose are registered and a volume to distribute will appear. This volume should be divided according to the desired prescription and modality.
2. After dividing the dose, a minimum recommended Qb will appear. This is based on flow rate when using diffusion and filtration fraction when using convection. This is only a recommendation.
3. The next step is to determine the expected down time of the therapy (according to center statistics) and the capacity of the dialyzer to saturate the effluent (normally 100%).
Finally the results will be:
- Filtration fraction (FF) and dilution factor (DF): both calculated using plasma water.
- Predicted delivered dose: an estimate of the dose considering, predilution, down time and effluent saturation.
- Standard Daily KtV: calculated using Watson formula for total body water, considering the excess volume of the patient and the predicted dose.
- Clearance: An equivalent of the delivered dose in ml/min

The delivered dose calculator helps to determine dose when effluent and BUN samples are measured. The hypothetical prescription given previously was actually delivered. After 24 hours 57 Liters of effluent where recollected and BUN samples were taken from 2 different ports. The results of the Adequator are: effluent saturation, clearance and a delivered dose.
The RCA calculator helps determine the infusion rate of a particular citrate solution for a specific effluent dose and blood flow.
Other calculators are available inside the app:
- Albumin and volumes for TPE
- Kinetic model for removal of macromolecules with TPE (pheresis)
- KoA calculator
- Residual kidney function (KRU)
Calculators that will be added in the future:
- Sodium correction with CRRT
- Calcium infusion calculator during RCA
- Prolonged intermittent renal replacement therapies (PIRRT) clearance calculator
Pablo Galindo, MD @galindozip
Nephrology Fellow, NSMC Intern 2020
Instituto Nacional de Nutrición
Mexico City, Mexico


