Urine acanthocytes are a distinct type of dysmorphic erythrocytes that can be found during microscopic examination of the urinary sediment. Their unique characteristics make them rather pathognomonic of hematuria that originates from a glomerular disease, i.e., glomerular hematuria (Figure 1).
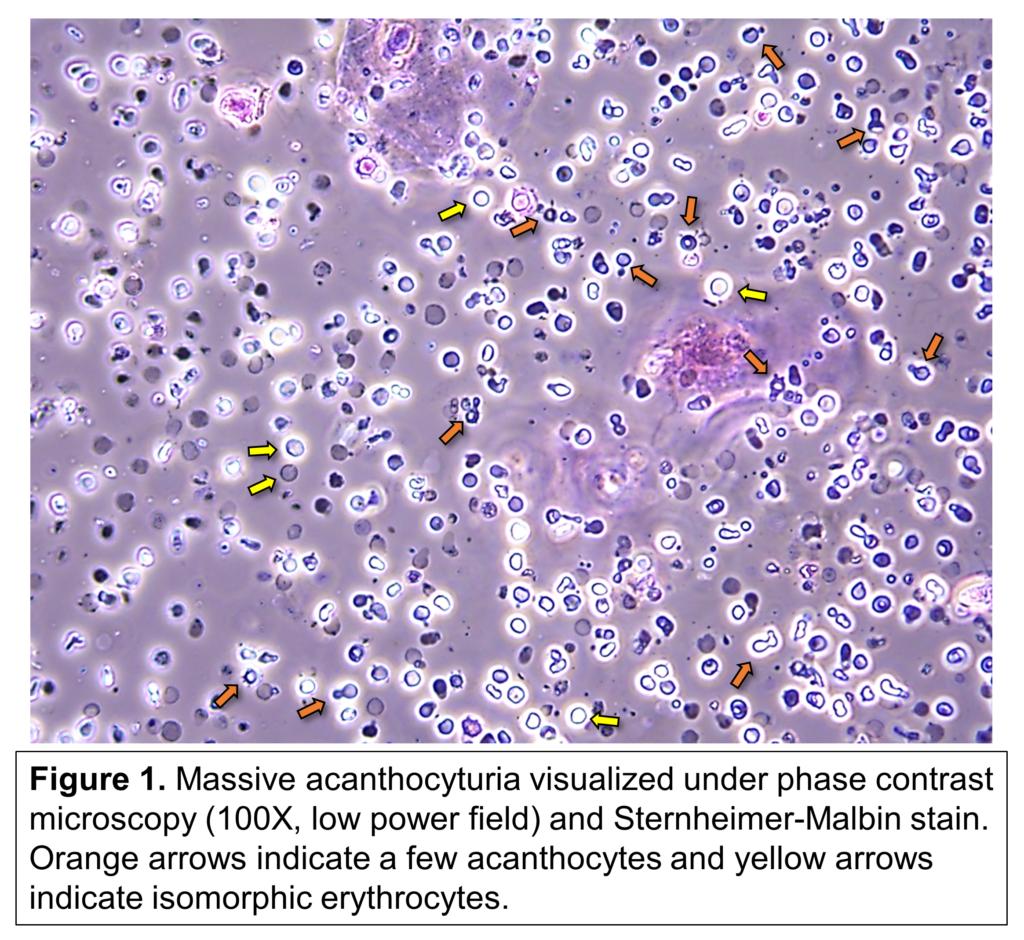
Among glomerular diseases, those characterized by proliferative lesions, lesions in the glomerular basement membrane or those affecting either the mesangium or the endothelial layer (e.g., class III-IV lupus nephritis, Alport, IgA nephropathy, infection-related glomerulonephritis, etc.) can present with acanthocyturia, whereas podocytopathies or non-proliferative diseases (e.g., FSGS, membranous nephropathy, etc.) typically do not present with glomerular hematuria.
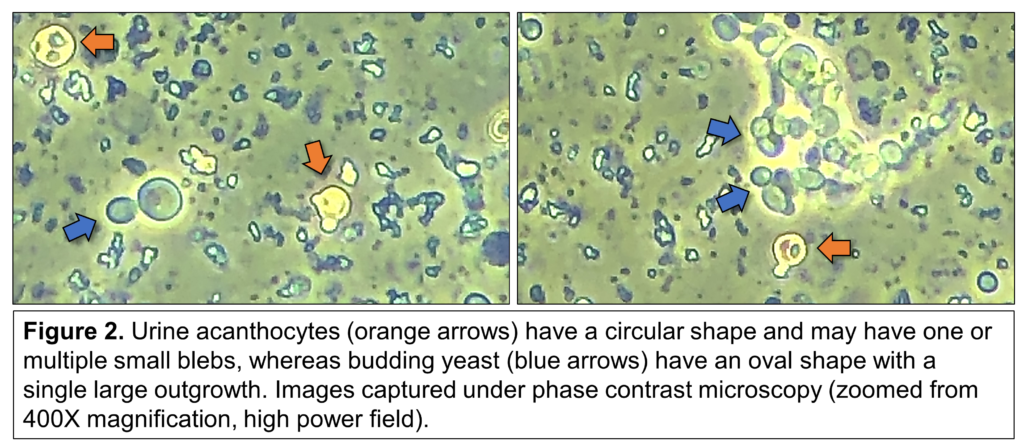
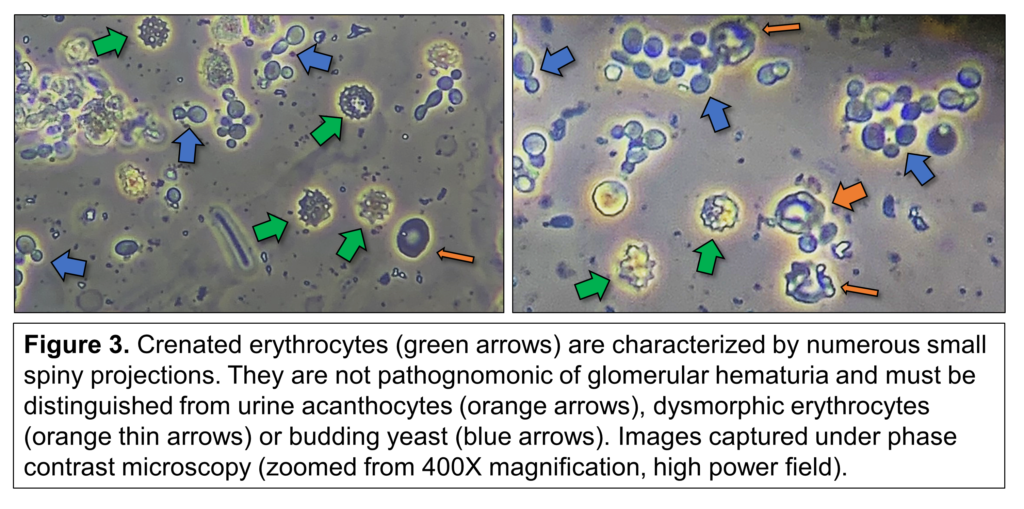
The optimal modality of microscopy to visualize and appreciate the unique morphology of urine acanthocytes is phase contrast microscopy, under 400X magnification. However, it is important to recognize 2 specific structures that can be misinterpreted as urine acanthocytes: 1) budding yeast (e.g., candiduria): these oval structures could adopt an almost circular appearance and exhibit protruding outgrowths as part of their asexual reproduction. Without close and careful inspection, budding yeast can be mistakenly recognized as dysmorphic erythrocytes with blebs or acanthocytes (Figure 2); and 2) crenated red blood cells: these markedly dysmorphic erythrocytes with “spiky” or multiple small spiny projections (Figure 3) can be found in urine sediment samples, but they do not indicate glomerular hematuria. Instead, they can arise from a hypertonic urine or dislodged blood clots. Anecdotally, they can occasionally be found in the context of candiduria.
@VelezNephHepato
#UrinarySediment #PisseProphet #UrineMicroscopy #SpinYourOwnUrine



does the diagnosis of dysmorphic RBCs is considered qualitative ( present/absent) or quantitative ( %) and if quantitative which % is considered significant ?
Very good slides