The greyscale ultrasound image is derived from the amplitude information in the echoes returning from a structure/organ. Rapidly moving structures such as red blood cells within blood vessels make very low amplitude echoes that cannot be displayed. That is why blood vessels appear anechoic or black. On the other hand, Doppler ultrasound (DUS) uses the frequency information from the echoes instead of amplitude and enables us to detect and measure blood flow.
Following are some of the DUS applications pertinent to nephrology practice:
- Identify blood flow (e.g. vessel identification for catheter placement)
- Arteriovenous fistula assessment
- Assessment of intracardiac flows to determine stroke volume, right ventricular systolic pressure etc.
- Assessment of systemic venous congestion
- Renal and splenic artery resistive index measurement during hemodynamic assessment
Most of these are considered ‘advanced’ applications that require a higher level of psychomotor and cognitive training compared to basic POCUS. Having thorough knowledge of the working principles of DUS makes these techniques easier to learn and interpret.
Let us start by understanding the Doppler effect and then briefly discuss various Doppler modalities.
Doppler effect:
The Doppler effect is a shift in the frequency of sound waves due to relative motion between the source (= moving RBC) and the observer (= transducer). In ultrasonography, the transducer sends out sound waves of a particular frequency (transmitted frequency or Ft) and listens to the echoes. When the target structure is moving (RBC), the returning or reflected frequency (Fr) is different. The difference between Ft and Fr is called the ‘Doppler shift’. It is determined by these 4 things:
- Transmitted frequency (Ft)
- Velocity of the blood flow (V)
- Angle of insonation (angle between the ultrasound beam and blood flow)
- Velocity of the sound in tissue (C)
Putting them into an equation, we get the formula, Doppler shift = 2 x Ft x V x cos q / C
Note that the angle (q) is the only thing that really changes in this equation and rest are almost constant. Cosine of 90 degrees is 0, which makes the Doppler shift 0 and cosine of 0 degrees is 1, which allows the maximum Doppler shift. In other words, when the angle of insonation is perpendicular to the blood vessel, the flow is not detected well and if the ultrasound beam is parallel to the vessel, you get maximum flow detection [Figure 1]. In reality, its not always possible to have the ultrasound beam parallel to the blood flow. Therefore, an angle of <60 degrees is considered acceptable (e.g. during flow measurement in AV access).

Figure 1: The Doppler equation
Color Doppler:
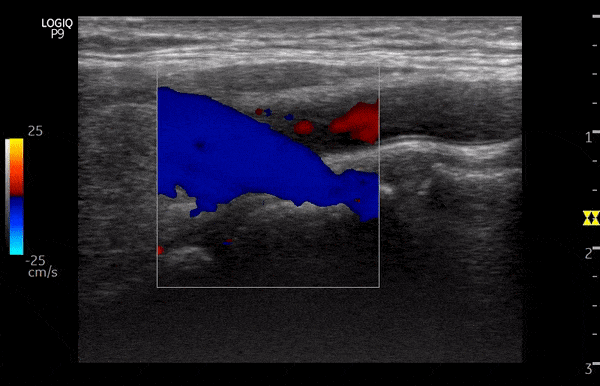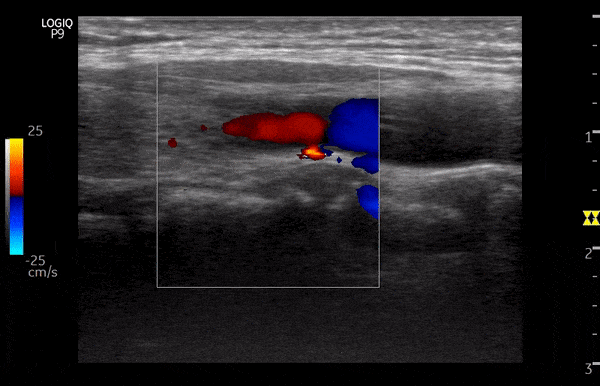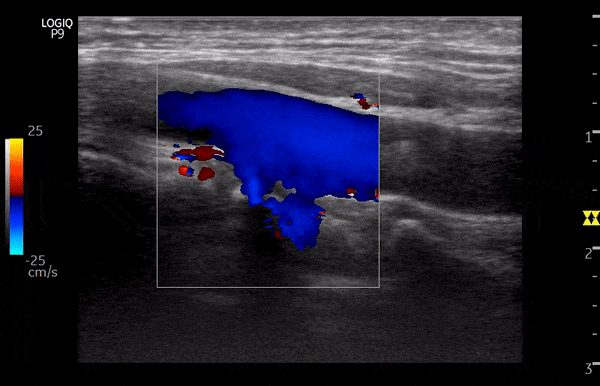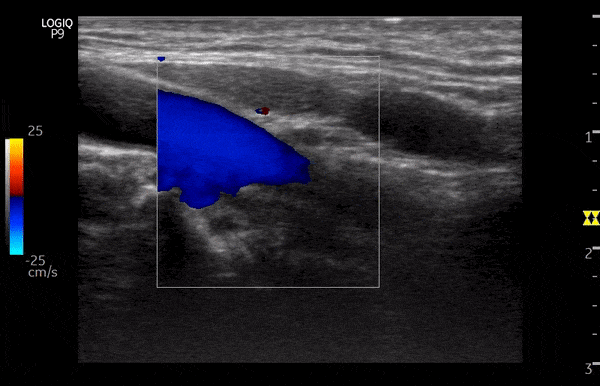
Color Doppler or color flow Doppler helps us to know 2 things: (1) whether there is any flow and (2) the direction of flow. It does not ‘quantify’ the flow (= does not give the exact velocity or allow waveform analysis). When the RBC moves away from the transducer, the reflected frequency (Fr) is lower than the transmitted frequency (Ft) and the shift is represented as blue color. Conversely, if the RBC is moving towards the transducer, Fr is higher than the Ft and the shift is represented as red color. This can be remembered by the mnemonic BART (Blue Away; Red Towards) [Figure 2]. This is how we know the direction of flow. It is important to remember that these colors just represent the flow direction and have nothing to do with whether the vessel is an artery or a vein.
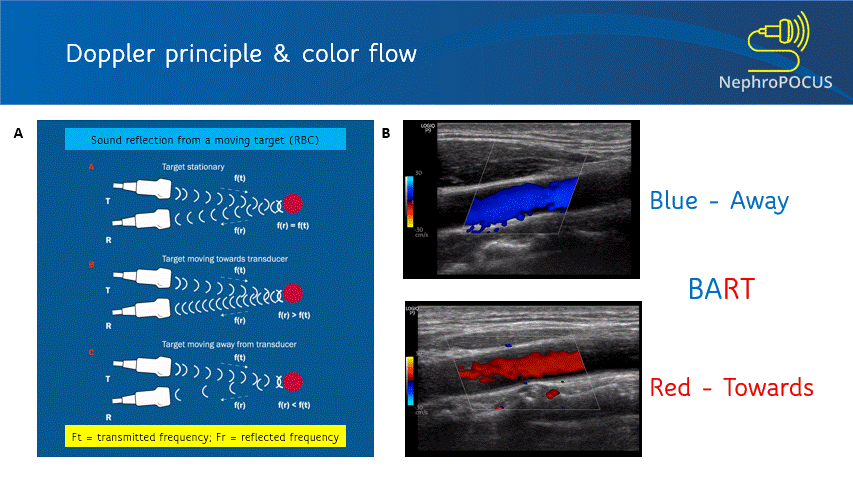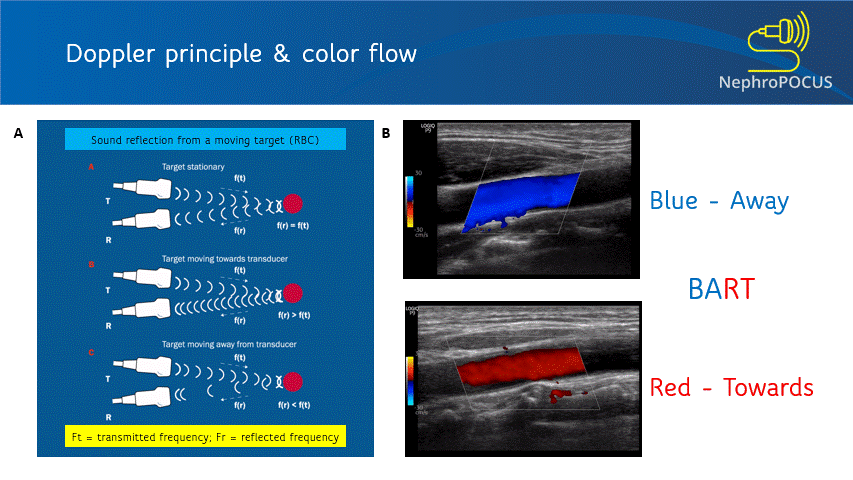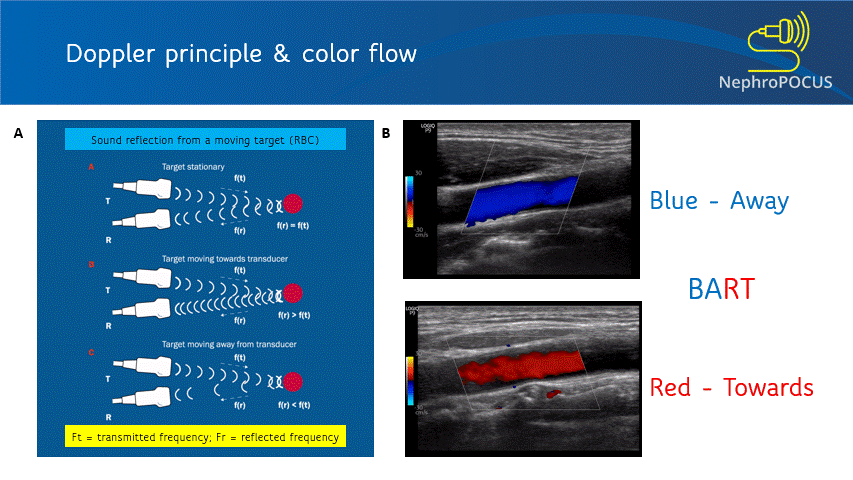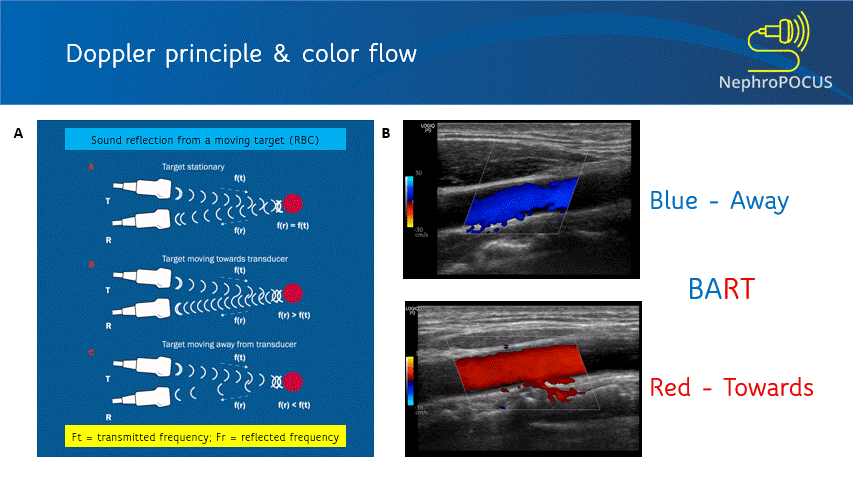
As mentioned, you do not get good flow or accurate information on the direction if the angle of insonation is 90 degrees (perpendicular to the vessel). We can use the ‘beam steering’ function to alter the angle of insonation without changing the probe position [Figures 3-5].
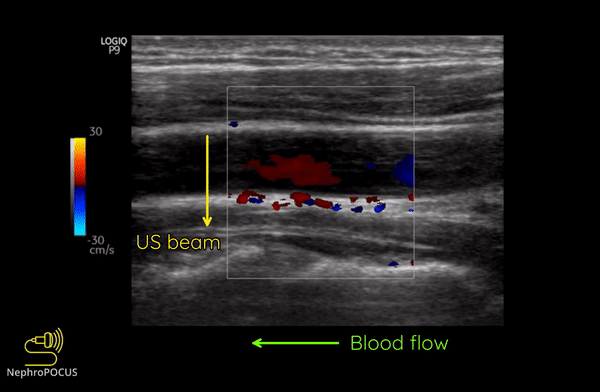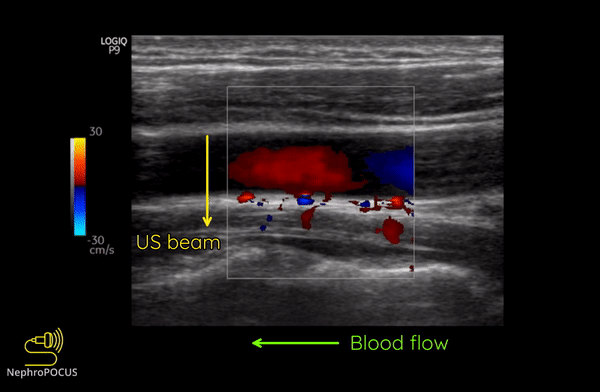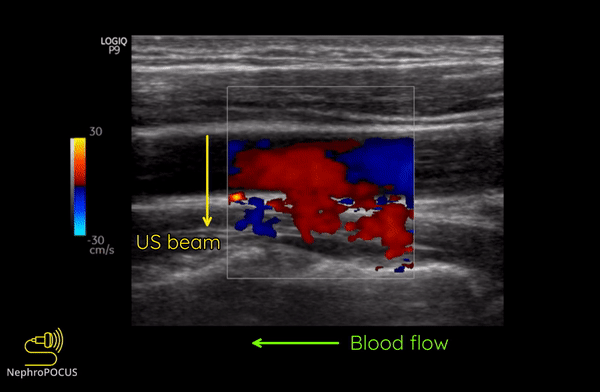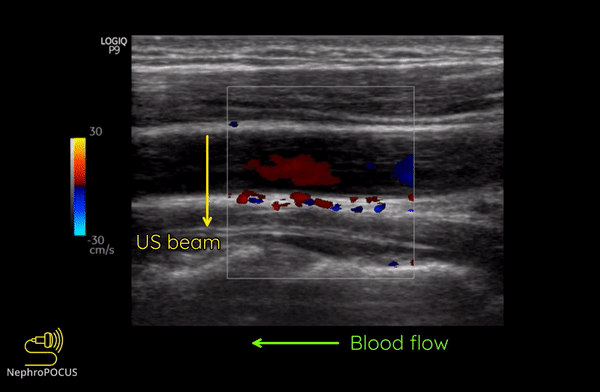
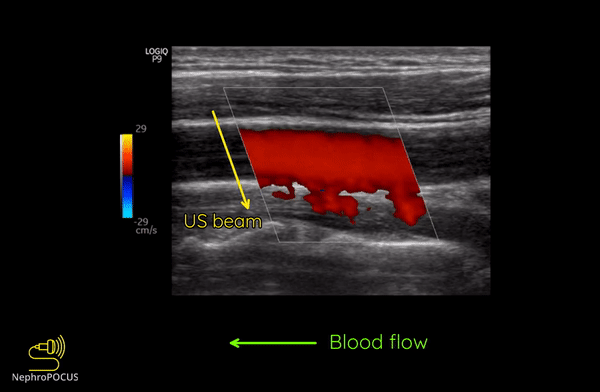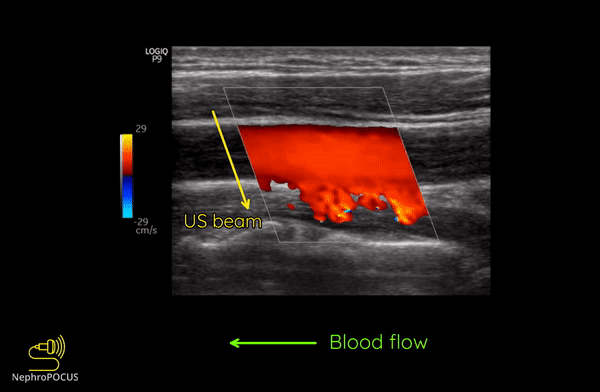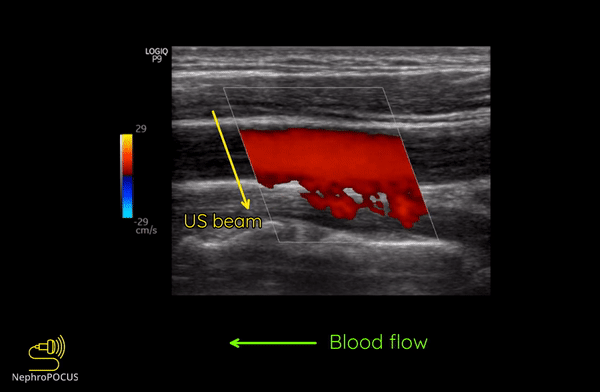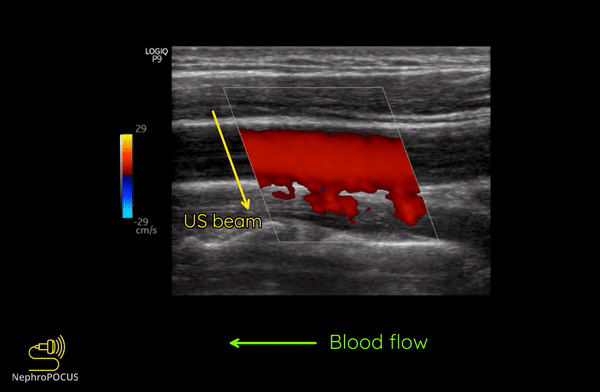
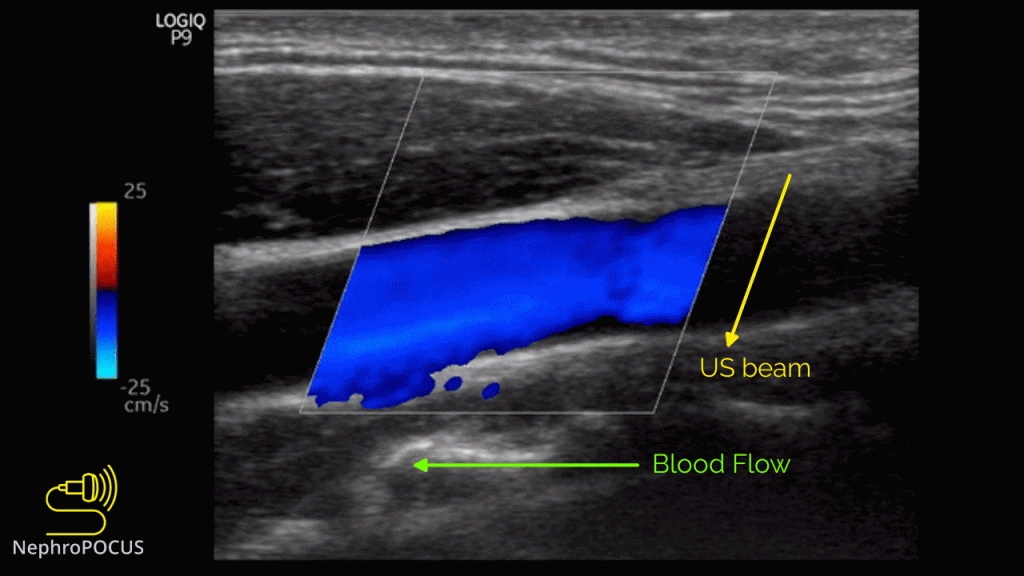
Alternatively, angle can also be adjusted by simply moving the transducer so that it is oblique to the vessel if the anatomy permits [Figures 6 and 7].
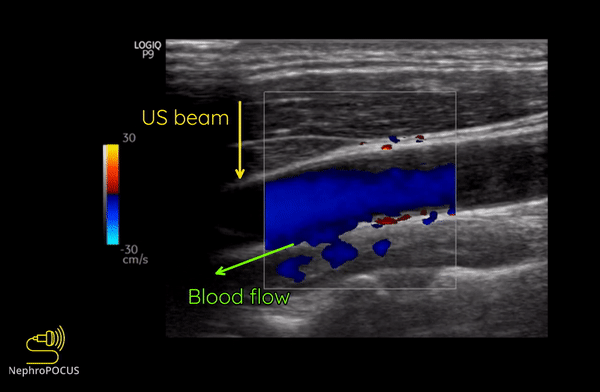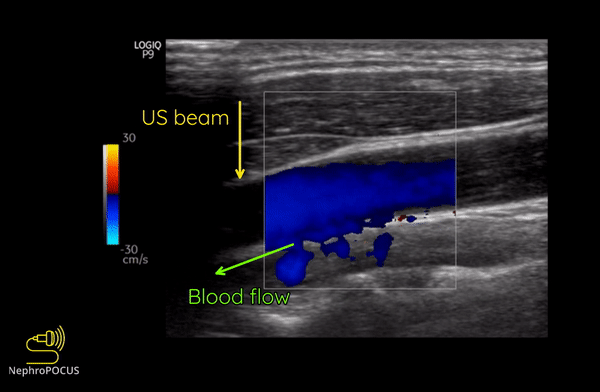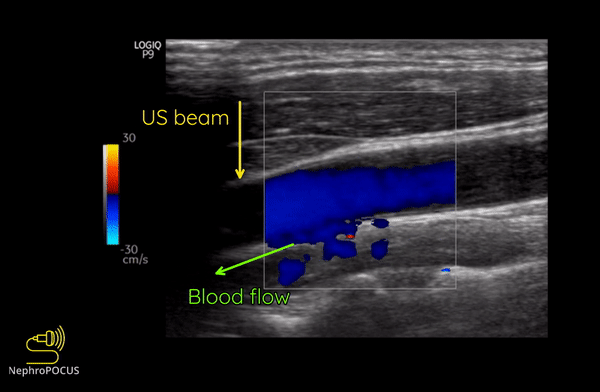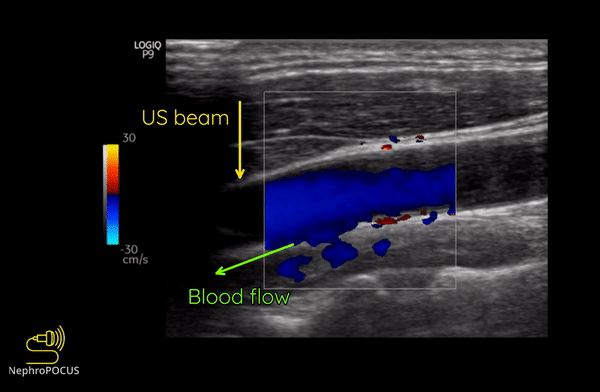
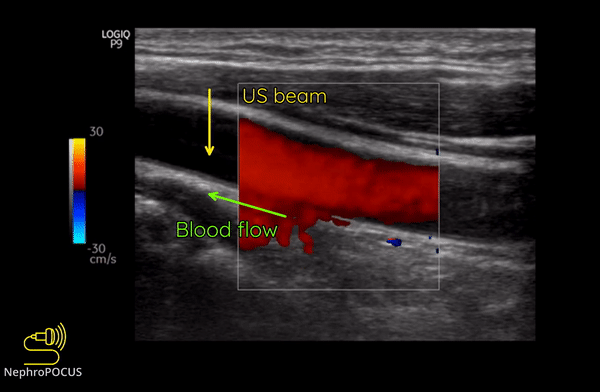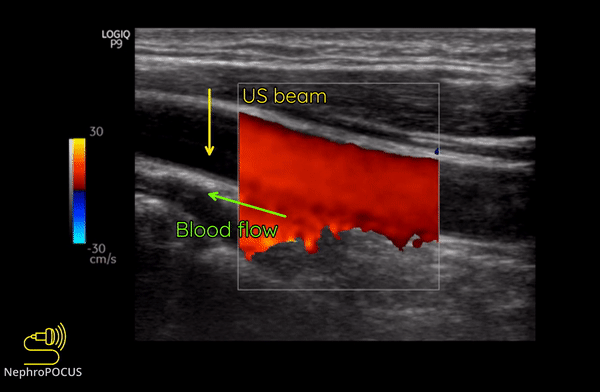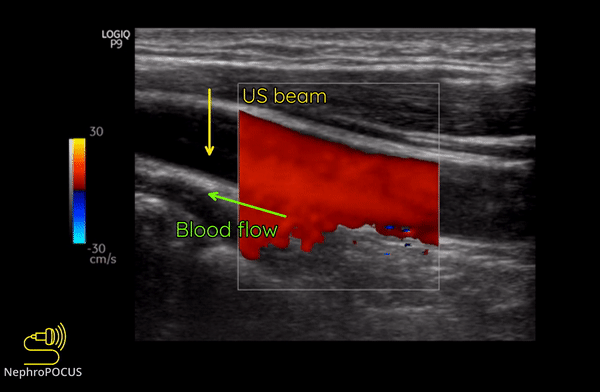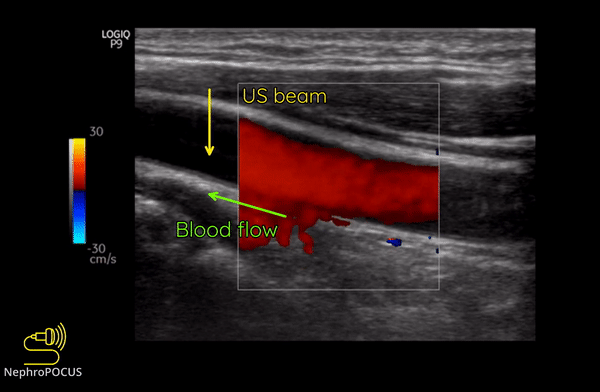
Figure 8 illustrates the change of colors from red to blue in the same blood vessel by changing the angle of insonation.
Power Doppler:
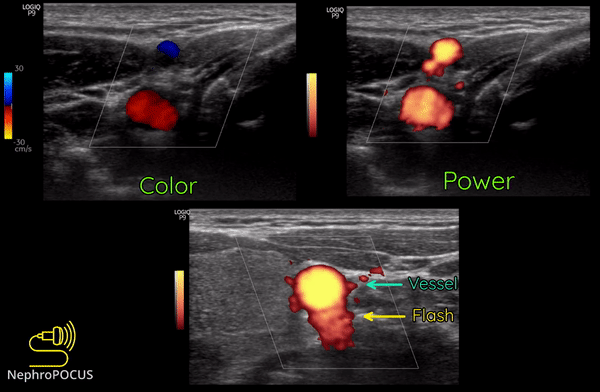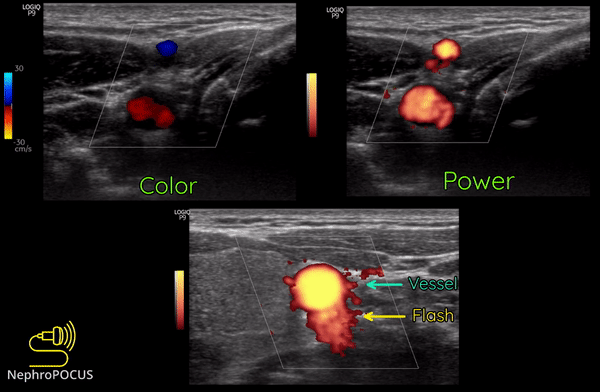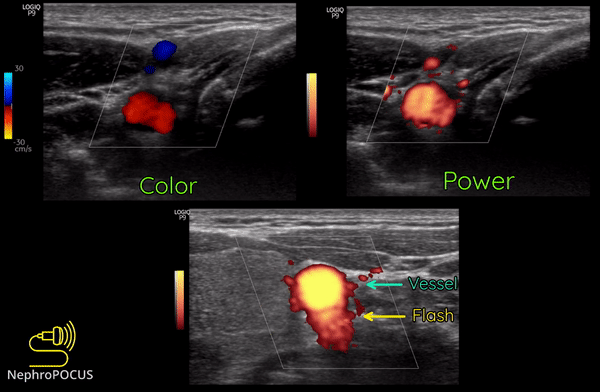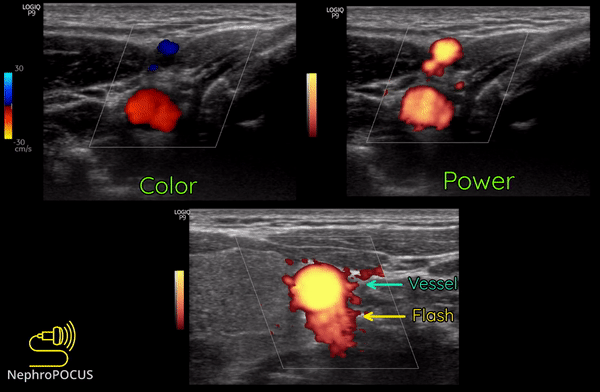
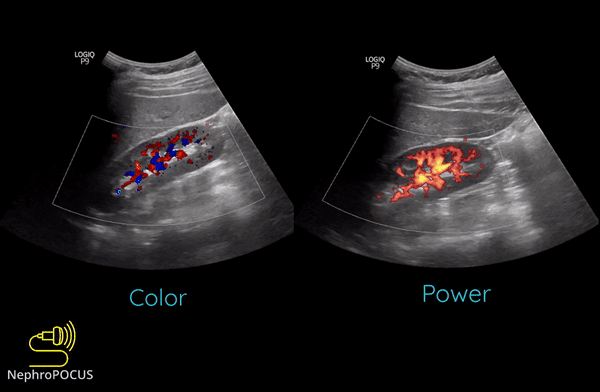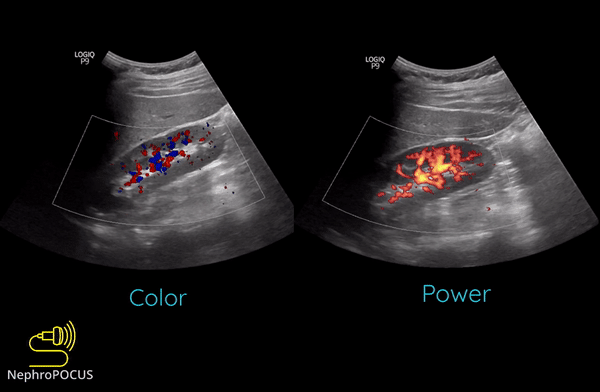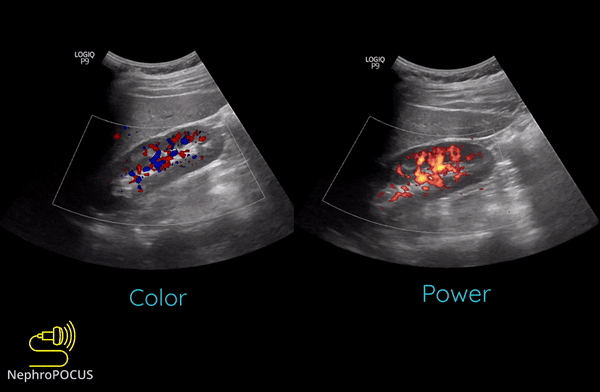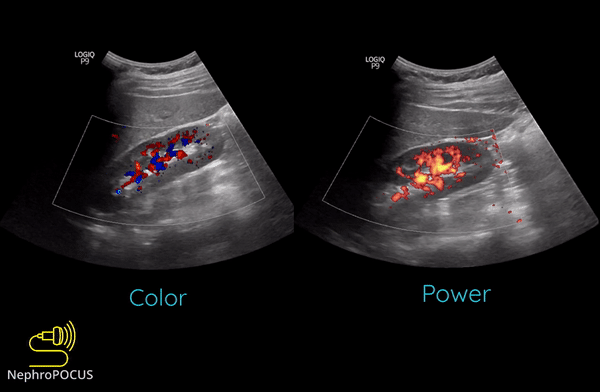
Power Doppler is another qualitative Doppler modality that tells us whether there is any flow. Unlike color Doppler, it does not give any information on the direction of flow (no red-blue). The hue and brightness of the signal represent the ‘power’ or intensity of the returning echoes rather than the frequency information. This power is related to the number of RBCs producing the Doppler shift. The key advantage of power Doppler is that its sensitivity for detecting flow is 3-5 times higher than with conventional color Doppler. It can be used to detect low-flow vessels (e.g. trying to avoid a small vessel while draining an abscess, assessing tumors etc.). Another advantage is that it is less angle dependent. Downside is its susceptibility to ‘flash artifacts’ because it is too sensitive and captures the movement of the surrounding soft tissue.
Following are examples of some images obtained using power Doppler. Color images included for comparison [Figures 9 and 10]
In the next part, we will delve further and talk about the spectral Doppler.
Abhilash Koratala, MD (@NephroP)
Medical College of Wisconsin



Hi Michelle,
Thanks for pointing that out. It was a mistake. Will try to replace the figure.
Abhilash (@NephroP)
Great information, thanks so much for sharing your knowledge.
I have a comment regarding figure 5.
In figure 5, the transducer is located at the side of the image where your yellow US beam arrow is.
On your Color map in figure 5, blue is set as the top color indicating that blue represents flow towards the transducer, not away.
Your blood flow arrow at the bottom of the figure indicates flow away from the transducer, which would be red on the color map displayed in figure 5.
So either your color map is inverted, or your blood flow direction is opposite that indicated in figure 5.
Very informative, I am more rich in knowledge after reading this.