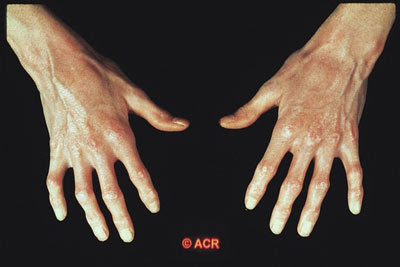
 Scleroderma is a chronic autoimmune disease characterized by fibrosis and hardening of the skin and other organs–occasionally involving the kidney to such an extent that dialysis becomes necessary. There are two main flavors of scleroderma:
Scleroderma is a chronic autoimmune disease characterized by fibrosis and hardening of the skin and other organs–occasionally involving the kidney to such an extent that dialysis becomes necessary. There are two main flavors of scleroderma:(1) the CREST syndrome, a localized form of the disease in which the kidney is NOT typically involved. This variant is typically anti-centromere antibody-positive. Hearkening back to your internal medicine days, you will recall that “CREST” stands for “Calcinosis, Reynaud’s phenomenon, Esophageal dysmotility, Sclerodactyly, and Telangiectasias.”
(2) Diffuse scleroderma, which is the type that may result in hypertension and renal involvement. These patients are more likely to be anti-SCL70 antibody-positive. The term “scleroderma renal crisis” is used to describe scleroderma patients with aggressively accelerating hypertension which may even result in renal failure. The mechanism of disease is a thrombotic microangiopathy, and urinalysis is generally bland. The mainstay of therapy for scleroderma renal crisis is blockade of the renin-angiotensin system.


