 We’ve known this medical factoid since we were medical students: you can’t successfully replete a potassium-depleted patient if they have low magnesium levels. But what is the mechanism by which this occurs?
We’ve known this medical factoid since we were medical students: you can’t successfully replete a potassium-depleted patient if they have low magnesium levels. But what is the mechanism by which this occurs?
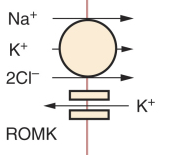
One possible explanation is put forth in a 2007 JASN article by Huang and Kuo. In this paper, the authors suggest that magnesium regulates the activity of ROMK, the renal outer medullary potassium channel, providing a rationale for how low Mg levels lead to low K levels. ROMK is the inwardly rectifying K channel on the apical surface of the distal nephron which is required for the backleak of K+. When there is high intracellular Mg2+, it will block the ROMK channel pore and prevent K+ from effluxing. Conversely, a low intracellular Mg2+ would allow for high ROMK efflux activity and therefore result in K+ wasting. The authors are cautious to state that additional factors (e.g., high aldosterone levels, increased Na uptake, etc) may also be required to result in clinically significant renal K+ losses.

