 Have you ever given THAM (tromethamine)? For whatever reason I was completely unfamiliar with the drug as a resident, but it is given not infrequently in the surgical ICU’s in the hospitals in which I’ve worked as a renal fellow.
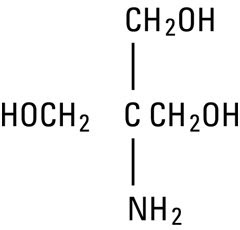
Have you ever given THAM (tromethamine)? For whatever reason I was completely unfamiliar with the drug as a resident, but it is given not infrequently in the surgical ICU’s in the hospitals in which I’ve worked as a renal fellow.THAM can be considered as an “alternative buffering agent”–that is, it is sometimes used in place of sodium bicarbonate in critically ill patients with significant metabolic acidosis. It is a biologically inert amino-alcohol (see structure above) which acts as a proton acceptor. Its purported advantage with respect to bicarbonate is that it allegedly decreases PaCO2 (as opposed to bicarbonate, which will cause an increased PaCO2), thus providing a way to treat ICU patients with acidosis who are difficult to adequately ventilate. However, it is eliminated primarily by the kidney and is associated with hyperkalemia, and many of the patients in whom its use might be beneficial (status-post cardiac bypass surgery, post-cardiac arrest) are likely to have renal impairment, making its safety profile questionable. It is also known to cause hypoglycemia.
I don’t have a lot of experience using this drug, but THAM dosing can be estimated as follows, according to this NEJM article: THAM (in milliliters of 0.3M solution) = lean body weight (in kilograms) x the base deficit (in millimoles per liter). The maximal daily dose is 15 mmol/kg for an adult (3.5 liters of a 0.3M solution in a patient weighing 70kg).

