 A relatively recent study by Bockenhauer et al in NEJM reports the identification of a new disease gene in a rare tubulopathy syndrome that sheds light on the physiologic mechanisms of salt transport in the kidney.
A relatively recent study by Bockenhauer et al in NEJM reports the identification of a new disease gene in a rare tubulopathy syndrome that sheds light on the physiologic mechanisms of salt transport in the kidney.
The article describes children with an autosomal recessive inherited condition termed “EAST Syndrome”, which stands for epilepsy, ataxia, sensorineural deafness, and tubulopathy. Specifically, patients had evidence of renal salt wasting with low-normal blood pressure, resulting in activation of the renin-angiotensin system and a resultant hypokalemic metabolic alkalosis. Individuals also demonstrated significant hypomagnesemia and hypocalciuria. Genetic studies identified the cause of EAST Syndrome: mutations in the gene KCNJ10, a potassium channel which is expressed in all of the affected tissues (brain, inner ear, and kidney) in this disorder. They go on to demonstrate that mice made deficient for KCNJ10 show a similar salt wasting phenotype as in affected humans.
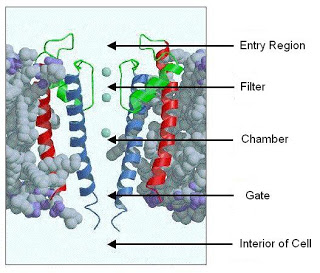
What does KCNJ10 do? The authors propose that this potassium channel sits at the basolateral membrane of tubular epithelial cells where it recycles potassium, which is necessary for maintaining the activity of the Na/K-ATPase. Although rare, EAST Syndrome helps provide greater molecular detail of how the kidney absorbs salt, and suggests that researchers look for polymorphisms in this gene which may explain some of the genetic predisposition towards hypertension and salt handling by the kidney.


