As the longevity of non-renal organ transplants increases, so too does the risk of eventually getting chronic kidney disease. The occurrence of post-transplant CKD is relatively common due to two primary factors: (1) a dependence on calcineurin inhibitors for immunosuppression, which over the longhaul can result in chronic nephrotoxicity, and (2) an increased susceptibility to repeated bouts of acute kidney injury in the peri- and post-transplant state, often due to hemodynamic fluctuations such as hepatorenal syndrome (in those with liver failure) or cardiorenal syndrome (in those with heart failure).
Not surprisingly, different organ transplants are associated with different rates of CKD and ESRD than others. In a paper by Ojo et al in NEJM in 2003, investigators determined which organ transplants had the highest rate of renal failure. Topping the list was intestine transplants, which occurred in a whopping 21.3% of recipients over a 5-year period. This was followed by (in decreasing order) liver transplants, lung transplants, heart transplants and a much more modest risk of about 6.9% for those with a combined heart-lung transplant.
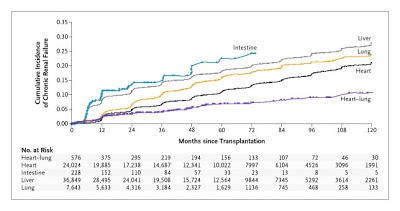 Not surprisingly, key predictors of CKD in this patient population in a multivariate analysis included old age, female sex, pretransplantation hepatitis C infection, hypertension, diabetes, and the presence of post-op AKI.
Not surprisingly, key predictors of CKD in this patient population in a multivariate analysis included old age, female sex, pretransplantation hepatitis C infection, hypertension, diabetes, and the presence of post-op AKI.
Although not mentioned in this particular paper, the prevalence of CKD/ESRD associated with stem cell transplants is overall lower than for the solid organs listed above. One potential reason for this is that calcineurin inhibitors are not required chronically in many of these patients.

What is left out of this article by Ojo et al. is the incidence of CKD in hematopoietic cell transplantation. This is a systematic review in the American Journal of Transplantation that attempts to answer this important question.
http://www3.interscience.wiley.com/journal/121421710/abstract?CRETRY=1&SRETRY=0
Matt Sparks
Renal Fellow, Duke Hospital