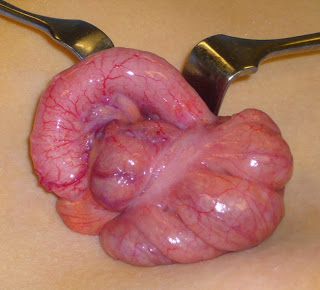
 Traditionally surgeons have relied on a well-honed abdominal exam, combined with abdominal imaging usually in the form of an iv-contrast CT scan, to make the diagnosis of acute appendicitis. Nevertheless, there remain significant instances of “false negatives” (usually a delay in diagnosis due to real episodes of appendicitis not picked up on imaging, occasionally resulting in appendiceal rupture) as well as instances of “false positives” (individuals who undergo appendectomy due to suspected appendicitis, but turn out to have no local inflammation on biopsy).
Traditionally surgeons have relied on a well-honed abdominal exam, combined with abdominal imaging usually in the form of an iv-contrast CT scan, to make the diagnosis of acute appendicitis. Nevertheless, there remain significant instances of “false negatives” (usually a delay in diagnosis due to real episodes of appendicitis not picked up on imaging, occasionally resulting in appendiceal rupture) as well as instances of “false positives” (individuals who undergo appendectomy due to suspected appendicitis, but turn out to have no local inflammation on biopsy).
In order to improve the rapidity of diagnosis of appendicitis, Kentsis et al sought to identify new urine biomarkers which could conceivably help, as described in a recent issue of Annals of Emergency Medicine. In brief, their study subjected 12 urine specimens–6 from patients with appendicitis and 6 from patients without appendicitis–to mass spectrometry. They identified a list of several potential biomarkers which were elevated uniquely in appendicitis. They then attempted to validate selected markers in 67 children admitted for suspected appendicitis, 25 of which eventually turned out to have true appendicitis. The most promising candidate was leucine-rich alpha-2-glycoprotein (LRG), which demonstrated near-perfect sensitivity & specificity for predicting appendicitis early on.
I think the study is relevant to nephrology to the extent that substances specific to disease processes other than the kidney can be detected in the urine: “the urine is the window to the soul.” It also is another example of how this cool “high-throughput”-type technology will continue to lead to the identification of new useful diagnostic tests relatively quickly.