BK Nephropathy refers to damage suffered to a renal allograft as a result of the polyomavirus BK virus. It is named based on the fact that it was originally isolated in the urine of a kidney transplant patient with the initials “B.K.” in 1971. Infection with BK virus rarely causes problems in immunocompetent individuals; however, the increased use of potent immunosuppressives such as tacrolimus and MMF have increased the risk of BK nephropathy.
While BK nephropathy is often suspected based on monitoring of either serum or urine BK virus levels, the allograft biopsy is presently an essential aspect of its diagnosis. A few of the key characteristics of BK nephropathy worth noting:
1. interstitial fibrosis: there is a staging system for BK Nephropathy (see this article)–it lists three stages (A, B, and C) which vary according to the degree of interstitial fibrosis and, not surprisingly, is associated with prognosis.
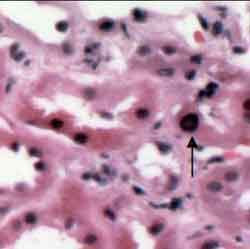
2. intranuclear inclusion bodies: renal epithelial cells may contain large nuclei indicative of viral infection. Viral infection may also occur in transitional epithelium of the bladder, and when shed into the urine show up as decoy cells, another non-invasive means of helping obtain a diagnosis of BK Nephropathy.
3. Immunohistochemical staining against the SV-40 T-antigen. These special stains will often clinch the diagnosis of BK Nephropathy, as it is highly specific for all polymaviruses (the most common of which is BK virus, but on occasion is JC virus). Staining should be restricted to the nucleus and is a sign of active viral replication.
4. Electron microscopy demonstrating viral particles: the viral particles are typically intranuclear, 30-50nm in diameter, and have a icosahedral capsid structure (see below).