 Tuberous sclerosis complex (TSC) is a rare genetic disease, caused by mutations within one of two genes (TSC1 or TSC2) which is named for the formation of hard tumors (“tubers”) within a variety of tissues, including the CNS, kidneys, eyes, heart, lungs and skin. Often, dermatologic clues can be essential to making a diagnosis; common examples include facial angiofibromas (a rash of reddish spots appearing on the nose and cheeks in a butterfly distribution), “ash leaf spots” (hypopigmented macules), ungual or subungual fibromas, Shagreen patches (areas of thick, leathery skin, often found at the nape of the neck), and cafe au lait spots.
Tuberous sclerosis complex (TSC) is a rare genetic disease, caused by mutations within one of two genes (TSC1 or TSC2) which is named for the formation of hard tumors (“tubers”) within a variety of tissues, including the CNS, kidneys, eyes, heart, lungs and skin. Often, dermatologic clues can be essential to making a diagnosis; common examples include facial angiofibromas (a rash of reddish spots appearing on the nose and cheeks in a butterfly distribution), “ash leaf spots” (hypopigmented macules), ungual or subungual fibromas, Shagreen patches (areas of thick, leathery skin, often found at the nape of the neck), and cafe au lait spots.
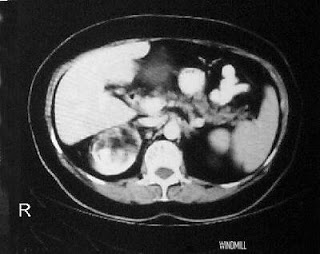
Most patients with tuberous sclerosis have some renal lesion, though fortunately it is usually not severe. There are a wide range of renal manifestation of TSC, many of which are detailed in this 2006 Kidney International review by Rakowski et al. About 80% of patients have renal angiomyolipomas, an abnormal collection of blood vessels, smooth muscle, and fat cells; these are best identified on CT as fat-containing lesions. They are felt to pose little to no risk of evolving into anything malignant, though they are at risk for bleeding (and sometimes even catastrophic bleeding). In addition to angiomyolipomas, up to 45% of TSC patients get cysts. Rarely, TSC and ADPKD can occurs simultaneously, as the TSC1 gene and PKD1 gene are located near one another and may be deleted in some instances. Finally, about 1-2% of TSC patients will develop renal cell carcinoma. This can be tricky to diagnose (especially given the high likelihood of angiomyolipomas or simple cysts). Individuals with TSC who get kidney failure and enjoy a transplant generally do well, though the current recommendation here is to perform a bilateral native nephrectomy at the time of transplant in the hopes of minimizing the cancer risk in the setting of immunosuppression.


Is there a chance of the renal tumors redeveloping in a transplanted kidney?