 Why do we care about hypomagnesemia? And why are cardiologists so eager to replete the serum magnesium above 2.0 mg/dL?
Why do we care about hypomagnesemia? And why are cardiologists so eager to replete the serum magnesium above 2.0 mg/dL?
Very low serum Mg can result in serious cardiovascular and CNS effects. Specifically, hypomagnesemia can cause QRS widening and may predispose to various arrhythmias (there is a nice section on this in Up-To-Date under “Significance of Hypomagnesemia in Cardiovascular Disease.” Furthermore, very low serum Mg can result in CNS effects such as coma or seizure. In addition, hypomagnesemia is linked with two other important electrolyte abnormalities: hypokalemia (reflecting the clinical pearl that it is nearly impossible to correct total body potassium stores while the serum magnesium remains low) and hypocalcemia (which can result from hypomagnesemia-induced PTH resistance).
The following is one potential approach to hypomagnesemia:
1. Decreased Magnesium Intake: The big one here is chronic alcoholism, which is actually thought to be related both to a nutrititonal deficiency of Mg as well as a renal Mg wasting effect of EtOH.
2. Redistribution of Mg from the Extracellular to the Intracellular Space: This can occur as part of the constellation of electrolyte abnormalities seen with refeeding syndrome, hungry bone syndrome, or during the treatment of DKA.
3. GI Losses of Mg: This can result from nearly any cause of chronic diarrhea (e.g., Crohn’s Disease, hx small bowel resection, chronic infectious diarrheas, etc), as well as losses from vomiting or NG suction.
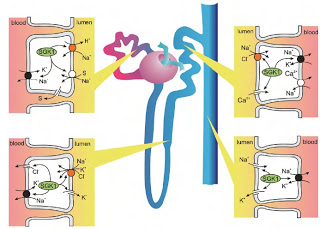
4. Renal Losses of Mg: Perhaps the most common cause of renal Mg wasting is simply diuretic use: both thiazide and loops diuretics can cause renal Mg loss. Other drugs (e.g., amphotericin B, aminoglycosides, cisplatin, pentamidine, cyclosporine, and tacrolimus) are also common culprits. Hypercalcemia also inhibits renal magnesium uptake. There are also a variety of genetic diseases that result in renal Mg loss, including Gitelman Syndrome, Bartter Syndrome, mutations in the paracellin or TRPM6 genes, and many others.

when I was chief at University of Arkansas for Medical Sciences they were considering dropping UpToDate as well and I had heard that this was beginning to be a common thing around the US. Apparently they (UpToDate) have dramatically increased the cost of an institutional subscription (which is typically paid for out of the library budget) so that more people will get individual subscriptions. The one bonus to the individual subscription is that it tracks your CME for you every time to log on and look at any page. I don't have one myself as I am still a research fellow and spend most of my time reading journals. would like to know if anybody else has any thoughts.
An important cause of Mg deficiency is the chronic use of proton pump inhibitors. Beware that some patients will develop this complication.
Wow–I can't imagine that's been a popular decision amongst MD Dukies. It's hard for me to envision an Up-To-Date-less world; it's kind of like the new universal medical textbook now. Not sure how much it costs our institution but I'll bet it's expensive.
Duke dropped UpToDate several months ago. We can still get it through the VA though. Any others hospitals having similar problems?
Matt Sparks