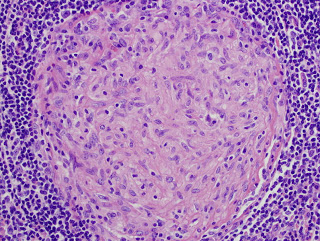
 Although it’s not common (somewhere between 0.5 – 0.9% of all native kidney biopsies according to published case series), one of the fellows produced an interesting case of granulomatous interstitial nephritis in Renal Grand Rounds today.
Although it’s not common (somewhere between 0.5 – 0.9% of all native kidney biopsies according to published case series), one of the fellows produced an interesting case of granulomatous interstitial nephritis in Renal Grand Rounds today. The case, in a nutshell: a middle-aged individual with ESRD of unknown etiology who is now on a 2nd cadaveric kidney transplant which was transplanted about a decade ago, presented to the Transplant Clinic with a creatinine that bumped from its baseline of 1.8 mg/dL to 2.4 mg/dL and a urinalysis which was largely unremarkable with the exception of a few WBC casts. The patient was being treated with sirolimus 1mg po daily, MMF 500mg po bid, and prednisone 2.5mg po daily which had not been changed recently. A renal allograft ultrasound was unremarkable, as were tests for circulating donor-specific antibodies. The patient underwent an allograft biopsy, which surprisingly showed multiple granulomas in the renal parenchyma along with significant interstitital nephritis.
What’s the underlying etiology of the granulomatous renal disease? To be fair, we don’t yet know. Granulomas are essentially an organized collection of macrophages–they are often recognized by the presence of multinucleated giant cells, which are multiple macrophages which fuse together, and they can be broadly categorized as being either caseating (that is, containing a necrotizing core) or non-caseating granulomas. The following is a differential diagnosis of the most likely culprits:
1. Tuberculosis: TB is a classic cause of non-caseating granulomas. This patient worked in the health care industry and therefore had annual PPD tests, all of which were negative.
2. Fungal infection: Histoplasmosis and Cryptococcus are some of the more common granuloma-inducing fungal infections.
3. Other infections: Cat-scratch fever (caused by Bartonella henselae) and chronic pyelonephritis can sometimes cause granulomas to be seen on kidney biopsy, and in these instances the interstitial infiltrate is usually more neutrophil-rich.
4. Sarcoidosis: Although sarcoid most often manifests as pulmonary issues, it can really affect almost any site, including the kidney.
5. Wegener’s granulomatosis: Evidence of pulmonary-renal syndrome and glomerulonephritis can raise suspicion for Wegener’s. It’s important to realize however that granulomas in the kidney are much more rare than granulomas in the upper respiratory tract.
6. Drugs: there are several reported instances of AIN producing granulomatous disease in the kidney. Somebody at RGR also suggested that perhaps sirolimus (known to result in other inflammatory complications such as pneumonitis and oral ulcers, for instance) should be considered as a culprit.
7. Idiopathic.
Due to the rarity of the condition, there is little consensus on how the condition should be managed. This case series by Joss et al in a 2007 issue of CJASN suggests that low- to moderate-dose steroids, after successfully ruling out infectious etiologies, can be beneficial.



Tuberculosis classified under Caseating Granulomas and Sarcoidosis Non Caseating Granulomas
I think you mean Tb is a classic cause of "caseating" granulomatous disease, don't you? Sarcoid comes to mind as a classic cause of "noncaseating" granulomas.