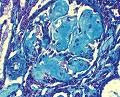
At Renal Grand Rounds yesterday, we discussed the case of a previously healthy 50 year old man who presented with fulminant hepatic failure and AKI. He was initially thought to have AKI related to either SIRS/hypotension or Hepatorenal Syndrome (which should be a diagnosis of exclusion), but was astutely noted to have significant (about 6 gm/day) proteinuria. The patient was worked up further: his serum electrophoresis revealed a monoclonal immunoglobulin spike and urine Bence Jones protein was present. Serum free kappa light chains were high and the kappa to lambda light chain ratio was significantly elevated. Concomitant liver biopsy revealed AL amyloidosis, which was further confirmed and typed by fat pad and colon biopsies. Unfortunately, the patient succumbed to multi-organ failure.
By way of quick review, amyloidosis is a group of diseases characterized by extracellular deposition of beta sheet fibrils which, in systemic forms, cause progressive organ dysfunction.
AL amyloidosis is characterized by fibrils that contain fragments of the variable portion of monoclonal light chains. This is the result of a clonal expansion of plasma cells, but interestingly, most patients with AL amyloidosis do not develop the manifestations of multiple myeloma, and most multiple myeloma patients do not have amyloid deposition. What both diseases have in common, however, is renal dysfunction which presents with significant proteinuria. Of note, given the pathophysiology of these diseases, the proteinuria is not related to albuminuria. Therefore, it is important to obtain a spot protein to creatinine ratio on all patients who may have otherwise unexplained or difficult to explain AKI, and subsequently pursue further work-up, including free serum light chain measurement.
In AL amyloidosis, response to therapy correlates with reduction in circulating light chains, so a hematologic response is the first marker in anticipation of renal function recovery or improvement. Interestingly, as well, the degree of baseline proteinuria on presentation correlates with response to treatment. Current treatment options include melphalan (an alkylating agent) plus steroids, Velcade (Bortezomib, a proteasome inhibitor) and rescue stem cell transplantation, which remains controversial.


Isn't it lamda chain is elevated with low k/lamda ratio in AL amyloid.