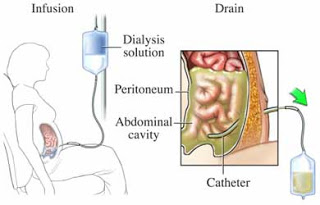
 A recent post got me thinking of the differential diagnosis of blood-stained peritoneal dialysis effluent. I thought it would be interesting to share some of the differentials and to remember that the Tenchkoff catheter can truly be a window to the abdominal cavity.
A recent post got me thinking of the differential diagnosis of blood-stained peritoneal dialysis effluent. I thought it would be interesting to share some of the differentials and to remember that the Tenchkoff catheter can truly be a window to the abdominal cavity.Blood-stained PD fluid can be dramatic and frightening for both patient and doctor alike. As little as 4-5mls of blood can be enough to cause grossly apparent colour changes in the fluid. A very succinct review can be found here.
Catheter related conditions
– Catheter insertion, manipulation and trauma/pulling of the external limb of the catheter can all cause local tissue damage at the peritoneal entry site, which could lead to blood staining.
– Insertion related trauma to intra-abdominal organs and/or vasculature can also cause more serious and more persistent bleeding. This may be reduced by laparoscopic assisted placement of catheters, which allows more direct visualization of the catheter during insertion. The risk of bleeding obviously increases if patients have significant adhesions and previous surgeries (often relative contraindications to successful PD anyway).
Menstruation
In female patients menses accounts for around one third of cases of haemoperitoneum associated with PD. This of course varies with age. The menstrual history is an important area to ask about during history taking from female PD patients. Ovulation can also result in haemoperitoneum.
Obstetric related
Lacerations of the gravid uterus by the PD catheter have been proposed as a possible rare cause for bloody PD fluid during pregnancy.
Other intra-abdominal organ pathology
Rupture cysts from ADPKD have been proposed to cause bloody PD fluid, despite their retroperitoneal location. It’s postulated that superficial cysts may form adhesions with the peritoneal cavity, allowing access after cyst rupture.
Liver and splenic lesions may cause bleeding into the peritoneal cavity – e.g. tumours, cysts, rupture and trauma. Bloody dialysate has rarely been reported after colonoscopy procedures also.
Surgery
Intra-abdominal surgery has been well recognized to lead to bloody PD fluid. The tendency to bleed may be enhanced by advanced uraemia and by the coexistence of any coagulopathies.
Of note gross haematuria is rare with infectious aetiologies of peritoneal disease. However, it is important to take advantage of the relative ease of acquiring a fluid sample when a PD patient presents with abdominal pathology. Remember that we can check for more than just white cells in a PD fluid sample – we can also look for red cells, amylase and abnormal cytology as just a few examples of additional tests. Putting all these clues together may lead us to an alternative and interesting diagnosis.


Have you ever gotten answers as to why this happens to you?
I believe my bloody dialysate was after I lifted too much weight and stretched too much while reaching to trim a tree branch. I was to strenuous that day. There was dull pain on the side where my catheter is located. That night the blood in the drain fluid was dark red and there was alot. The blood showed up during each drain throughout the entire time I was on the cycler (four times during 7 hours). The next day I went to the dialysis unit and they drained my fluid. It was mostly clear; just a hint of pink. Again that second night there was bright red blood filling the tubing, but it was only with the first drain cycle. The last 3 drain cycles were all clear. That third day I tried to be less active during the day. I noticed some throbbing pain when I first got up and moving around that morning. On the third night the drain fluid was completely clear. On the fourth day I noticed I could not take a vigorous walk or bend too much without feeling sore. That fourth night, I had some pink, but it was very faint. On the Fifth day I still felt sore after taking short walks. Drain fluid on the fifth night was completely clear.