As the authors point out, one of the major difficulties in determining the best treatment (and assessing the comparative effectiveness of therapies) is the heterogeneity in the presentation and prognosis of patients with IgA. It is extremely common, with up to 1.6% of zero-hour allograft biopsies having evidence of asymptomatic IgA. As a result, many patients are diagnosed incidentally and never have any clinically significant disease. One important issue relates to determining who is going to progress. The recently introduced MEST classification came about in an effort to define histological markers in IgA that predict progression. However, follow-up studies have indicated that the only consistent marker of progression was the degree of interstitial fibrosis and atrophy. It should be noted that this classification does not include crescents which are associated with a poor prognosis. Traditional clinical markers of progression include hypertension, increased BMI, smoking and, most importantly, persistent proteinuria of >1g/24 hours.
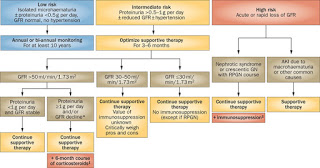
The treatment of IgA depends on the clinical presentation. Patients with normal blood pressure, normal renal function and no proteinuria can generally be watched in the clinic with no specific treatment and, in fact, it is debatable if these patients should be biopsied in the first place. The figure below (originally from JASN and reproduced in NRN) provides a suggested algorithm for the management of patients with IgA depending on the stage at presentation.
It is important to state that the only treatment that has been consistently been shown to be beneficial in patients with IgA is RAAS blockade.The role of corticosteroids is controversial and the current KDIGO guidelines suggest the use of steroids only in patients who have been on optimal therapy for 3-6 months, have persistent proteinuria >1g and have an eGFR of >50 ml/min/1.73m2. Low dose steroids are of no benefit and the use of higher dose steroid regimens is associated with significant morbidity so this recommendation comes with significant caveats. Other immunosuppressants including cyclophosphamide, MMF and azathioprine have been trialed in IgA and despite some encouraging results in open-label and retrospective studies, prospective studies have failed to show a consistent benefit. However, there are ongoing RCTs that will be reported in the next 12-24 months that may finally give us the definitive answer with regard to these agents.
Tonsillectomy, more commonly performed in Japan, is not recommended, either by these authors or in the KDIGO guidelines. Fish Oil may be of benefit in patients with persistent proteinuria >1g but is probably of limited use in other groups. One of the limitations of the studies of fish oil in IgA is that they were generally performed prior to the widespread use of ACEi and it is uncertain if they add any additional benefit to these agents. Again, the dose needs to be sufficient (supranormal doses).
Finally, crescentic IgA is a different entity that generally is associated with rapid progression. It is only diagnosed when more than 50% of glomeruli have crescents; the presence of a single crescent in one glomerulus should not prompt the institution of aggressive immunosuppressive therapy. Again, there are no RCTs that demonstrate a benefit of cyclophosphamide but there are some retrospective studies that have shown some effectiveness. That said, in the presence of rapidly progressive disease and active glomerular inflammation, the recommendation is that a combination of steroids and cyclophosphamide should be used.