U Penn
established an annual one-day seminar in nephrology symposium. This year was
titled “New Horizons in Nephrology: Updates in Glomerular Disease”.
established an annual one-day seminar in nephrology symposium. This year was
titled “New Horizons in Nephrology: Updates in Glomerular Disease”.
Dr.
Beck from Boston University gave the update on membranous nephropathy (MN). Previously,
we discussed his article in the NEJM in detail, and today we will go over some key points and updates:
Beck from Boston University gave the update on membranous nephropathy (MN). Previously,
we discussed his article in the NEJM in detail, and today we will go over some key points and updates:
- 75% of
MN is considered primary (idiopathic). - IgG4
subclass is predominant in idiopathic MN. - Anti-PLA2R
is highly specific for primary MN - Co-localization
of PLA2R and IgG4 within immune deposits on biopsy. - The
majority of patients with primary MN have circulating autoantibodies against
PLA2R.
There
is a clear association of anti-PLA2R with disease activity.
is a clear association of anti-PLA2R with disease activity.
– Positive
in nephrotic state.
in nephrotic state.
– Declines
prior to the decrease in proteinuria.
prior to the decrease in proteinuria.
– Absent
in remission.
in remission.
– Returns
with (or prior to) relapse.
with (or prior to) relapse.
– Associated
with recurrent MN
with recurrent MN
Methods
of testing:
of testing:
– Western
blot
blot
– Indirect
immunofluorescence test
immunofluorescence test
– ELISA :
Will likely be the test of choice. Available in Europe, not yet in the US.
Will likely be the test of choice. Available in Europe, not yet in the US.
Treatment:
– Do NOT
use corticosteroid monotherapy or MMF monotherapy for initial therapy of MN.
use corticosteroid monotherapy or MMF monotherapy for initial therapy of MN.
– No
single definitive immunosuppression could be easily identified.
single definitive immunosuppression could be easily identified.
Current
Initial therapy :
Initial therapy :
- Ponticelli
regimen: methylprednisolone 1g/d iv x 3 doses followed by oral prednisone
0.5mg/kg/d in months 1,3,5; oral cyclophosphamide (2mg/kg/d) in months 2,4,6. - Alternative
initial therapy for those who refuse or have contraindications to
cyclophosphamide is Calcineurin inhibitor (CNI) for at least 6 months. - Stop if
no remission in 6 months. - If
remission is attained, reduce dose every 1-2 mo by 50% and continue for at
least 12 months
Posted by Tarek Alhamad

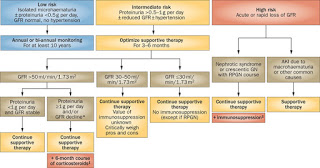
Totally agree. We just wanted to mention few updates about MN. Risk factors for developing worsening kidney dysfunction and ESRD are
– male sex
– Older age at onset
– Elevated Cr
– Proteinuria more than 8 gram /day
Treatment of MN is only indicated in case of expected worsening of kidney function; there is a substantial subgroup that will go into remission without intensive therapy as has been shown by hofstra and wetzels.