Ultrafiltration failure is a frequent clinical problem in PD patients. The most common etiologies are: fast peritoneal membrane transport, loss of peritoneal surface membrane and high lymphatic absorption. Mechanical and anatomical etiologies are occasionally seen.
Rule of 4’s is used to diagnose membrane ultrafiltration failure: less than 400ml UF using 4.25% bag after 4 hours.
Sudden onset of ultrafiltration failure may occur in the setting of peritoneal leakage. Though sometimes associated with localized subcutaneous edema, it is generally difficult to detect clinically. Retroperitoneal leakage is likely to arise from a tear or a gap in the peritoneum precipitated by an increase in intra-abdominal pressure associated with walking, coughing, straining, or using a high instilled volume (2.5 L or 3 L). Red flags may include history of hernia, pleuroperitoneal communication and large infusion volumes. The acute onset of ultrafiltration failure is another suggestive finding.
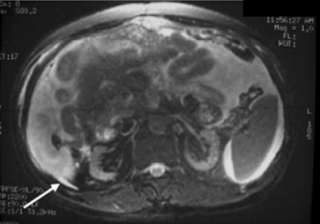
Best diagnostic modality is MRI (PD fluid can be used as constrast medium).
Management: involves interruption of PD. But few reports have achieved success by using fast cycles (1hour/exchanges x8) twice a week and leaving abdominal cavity empty between sessions for 4-8 weeks.