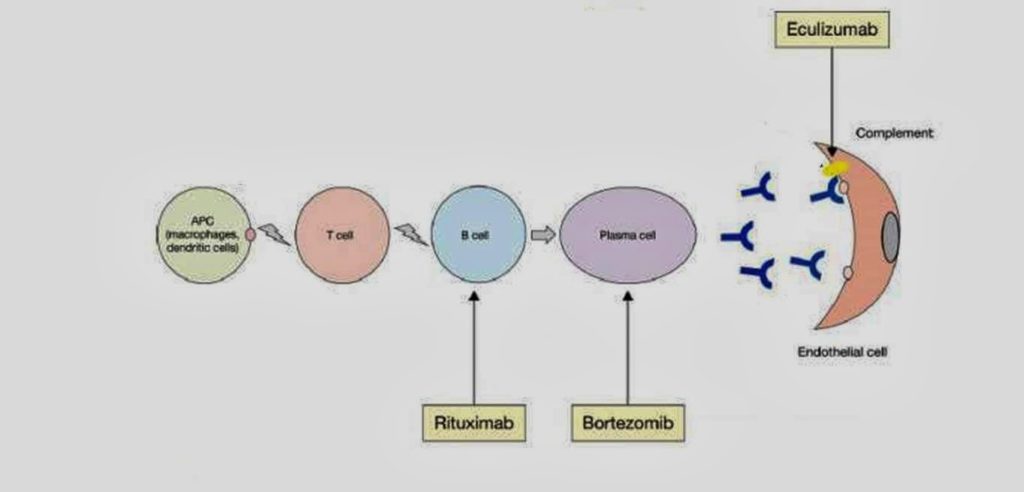
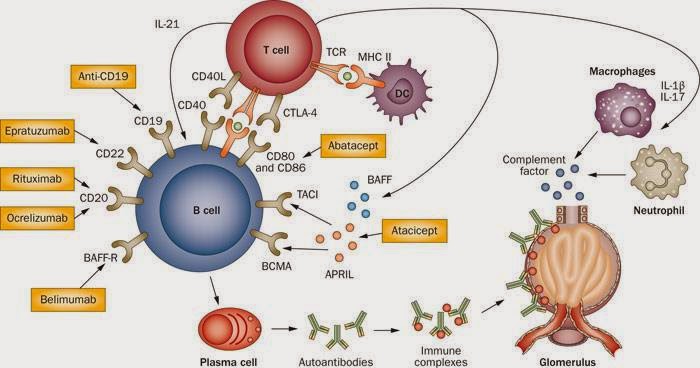
This is a really exciting bracket and is full of new agents that will hopefully lead to major advances in our field. Acthar is the outlier here as, even though it is a peptide, it is not an antibody. For all the other agents I find it helpful to visualize what the antibody is targeting and on which cell type. Hopefully these cartoons will help.
I think Rituximab and bortezomib should always go hand in hand when treating and auto- or alloimmune process as rituximab eliminates immature and naïve B cells and bortezomib eliminates B cells that have matured into antibody producing Plasma cells. There are some small trials reporting the use of both agents including a phase 2 trial in Waldenstroms Macroglobulinaemia but a large clinical trials using both these agents would be great.
In 2005 the FDA approved abatacept for RA after clinical trials showed benefit. However, there was evidence that this biologic might not be so efficacious in transplantation. Co-stimulation blockade on individual CD4+ T helper-cell subsets suggested a resistance of IL-17 secreting CCR6+ memory type 17 T helper cells (TH17) cells to CD28 and CTLA-4 blockade by abatacept. Effectively, abatacept inhibits the responsiveness of the total population, but a subset of cells are resistant to this inhibition.
Belatacept is a second-generation CTLA-4 Ig fusion protein that differs from abatacept by only 2 amino acid substitutions (L104E and A29Y), which gives rise to slower dissociation rates from both CD86 and CD80. Subsequent research revealed this agent to be 10-fold more potent in vitro, and a more effective inhibitor of renal transplant rejection than abatacept. The subsequent BENEFIT trials proved belatacepts efficacy in transplantation.
CR1 or complement receptor type 1 or C3b/C4b receptor or CD35 is protein encoded the CR1 gene. This gene is in the RCA (regulators of complement activation) cluster region of human chromosome 1. This region includes the CFHR 1-5 and CFH genes. All these genes when mutated can cause immune-complex glomerular diseases such as MPGN. This CR1 protein also accounts for all the Knops blood group antigens. Reductions in CR1 or down regulating mutations can also cause SLE. Soluble CR1 may be useful in transplantation also. One study showed that sCR1 treatment improved 24 hour creatinine and inflammatory profiles post transplant in rats transplanted after brain death.
As precursors to the plasma cells that secrete antibodies, B cells are central in the pathology of SLE.
Increased B-cell activation is due in part to increased levels of growth factors, including B-lymphocyte stimulator (BLyS), also called B-cell activating factor (BAFF). Belimumab is a human IgG1 monoclonal antibody that binds to soluble BLyS and thus prevents it from binding the BAFF receptors on B cells. So you can see where the trial names BLISS-52 and BLISS-76 come from, the numbers refer to the number of weeks the trials lasted. BLyS is a growth factor required for B-cell survival, maturation, and activation; germinal-center formation; the development of B cells into plasma cells; and immunoglobulin production. Many maturing B cells are completely dependent on the binding of BAFF receptors by BLyS to survive and mature. Memory B cells cells lack BAFF receptors. At least 50% of people with SLE have elevated plasma levels of soluble BLyS and there is a weak but significant correlation between high levels and active disease. Unfortunately patients with severe active LN were excluded from the BLISS trials.
For me Rituximab was the favourit in this groups as it is probably used in the greatest variety of diseases.
Thanks for reading and i hope you all learned something as i learned alot from NephMadness 2014. Now go to the NephMadness site and submit your brackets if you have not done so already!