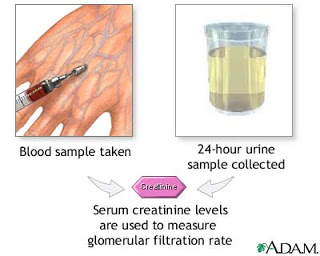
 The Panel 7: I remember it was one of the first things I learned in clinical medicine. Na, K, Cl, HCO3, BUN, creatinine and glucose. I know not all countries use the same “grid format” of presenting these numbers as we do in the U.S., but all of them use creatinine as the indicator of GFR which is so useful in interpreting a patient’s electrolyte values.
The Panel 7: I remember it was one of the first things I learned in clinical medicine. Na, K, Cl, HCO3, BUN, creatinine and glucose. I know not all countries use the same “grid format” of presenting these numbers as we do in the U.S., but all of them use creatinine as the indicator of GFR which is so useful in interpreting a patient’s electrolyte values.
While certainly useful, there is one big problem with creatinine that should be fairly obvious to all renal fellows: it is a relatively late marker of renal injury. By the time the creatinine has risen, there has already been significant renal damage. For some surgical patients in the ICU, immediately post-operatively after a CABG for example, we will start renal replacement therapy even with relatively “normal” creatinines in the 1.3 – 1.4 mg/dL range–if we feel there is a genuine acute kidney injury, as manifested (for instance) by anuria and volume overload. What if there was a blood test which indicated renal damage at the earliest stages of AKI–e.g., a substance whose concentration in the bloodstream (or urine) became significantly elevated before that of creatinine?
This is what the field of biomarkers is all about, and the race is on. Imagine a day where instead of creatinine in the lower right hand corner of the panel 7 there is a different test. An excellent review of the field can be found here, look for the April 2008 edition of the Brigham & Women’s “Nephrology Rounds” publication by Won Han. Four of the big biomarkers under investigation currently include neutrophil gelatinase associated lipocalin (NGAL), kidney injury molecule-1 (KIM-1), interleukin-18 (IL-18), and cystatin C. Many of them are detected in the urine–with the rationale that the earliest indication of tubular kidney damage would be to look for the presence of proteins expressed by renal tubular epithelial cells in response to ischemic damage in the urine. It could very well be that there is no single “winner” of the best test to detect early renal damage–perhaps different biomarkers can be used to detect injury within discrete regions of the nephron (e.g.,proximal tubular damage versus distal tubular damage), or perhaps different biomarkers will be able to detect different types of nephrotoxin-induced damage (e.g., contrast nephropathy versus sepsis-associated AKI). This is an interesting field with a promising future.



Very relavent information. All patients should be informed when faced with a diagnosis of Kidney Cancer.
Dear Dr Bellamy,
Your article is very interesting and indeed points the way to the future. However, I think that a better title would be “Beyond creatinine”, the types of tests that you mention offer the potential to detect renal injury so early that changes in therapy could avoid later increases in creatinine / renal failure. Serum creatinine is an important indicator of renal function, the biomarkers that you mention are indicators of ongoing renal injury. Your other comment about the potential of site specific biomarkers is also being addressed. Site specific renal biomarkers, eg. Alpha GST (proximal tubule) Pi GST (distal tubules) and RPA-1 (collecting duct) are currently under evaluation for this. For example, the International Life Sciences Institute nephrotoxicity working group found, alpha GST and RPA-1 to be more sensitive than serum creatinine for proximal tubule respective collecting duct injury while also providing site specific information. These studies also show the value of combining site specific biomarkers such as you suggest. They have submitted this data to the FDA for acceptance as qualified biomarkers for use in drug regulatory studies.
Studies are under way in humans where the release of biomarkers specific for the distal tubules may indicate more severe progressive injury. For example, in subjects undergoing coronary bypass elevations of urinary pi GST during, and immediately post, surgery may indicate the likelihood of the need for renal replacement therapy