 I heard a lecture not too long ago on atheroembolic renal disease which claimed that atheroembolic renal disease is to nephrology as sarcoidosis is to internal medicine. That is to say, it can present in a myriad of fashions, ends up being the diagnosis in a surprising number of complex cases, and pops up an inordinate number of times on tests.
I heard a lecture not too long ago on atheroembolic renal disease which claimed that atheroembolic renal disease is to nephrology as sarcoidosis is to internal medicine. That is to say, it can present in a myriad of fashions, ends up being the diagnosis in a surprising number of complex cases, and pops up an inordinate number of times on tests.
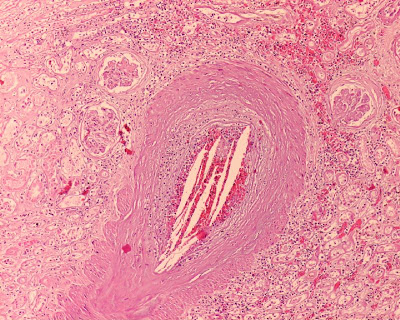
Although spontaneous atheroembolic can occur, much more commonly it is the result of iatrogenesis, with cardiac catheterization being probably the most common offender. Mechanical disruption of atherosclerotic plaques results in a showering of cholesterol emboli to downstream organs, where they are likely to lodge in small arterioles. The crystals induce an inflammatory reaction, resulting in adventitial fibrosis that eventually obliterates the vessel lumen. The crystals of cholesterol are dissolved during fixation, leaving biconvex “ghosts” within the affected arterioles, as demonstrated on this biopsy section.
Other physical & laboratory findings that can tip you off to a diagnosis of atheroembolic disease include livedo reticularis, amaurosis fugax, bluish discoloration of the distal extremities (often in an asymmetric pattern), peripheral and/or urine eosinophilia, and an elevated ESR/CRP.


