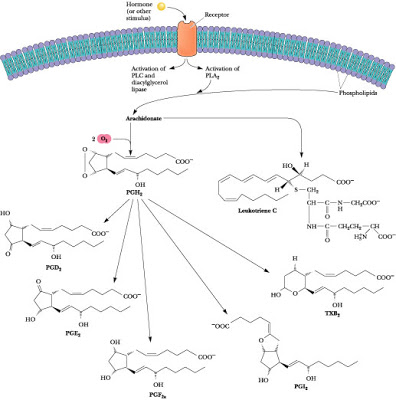
A few basics about the prostaglandins, a major player in renal hemodynamics. Prostaglandins are fatty acid-based compounds which carry out a variety of cellular effects. The pathway begins with phospholipid within the plasma membrane, which is converted to arachidonic acid by the enzyme phospholipase A2. Arachidonic acid then goes to one of two pathways: either it is metabolized by lipooxygenase to the leukotriene pathway (important for inflammation) OR it is metabolized by cyclo-oxygenase to the prostaglandin pathway. A variety of chemical modifications lead to different classes of prostaglandin: PGD’s, PGE’s, PGF’s, PGI’s, and thromboxane.
There are many different classes of prostaglandin present in the kidney, but perhaps the most well-known is prostaglandin E2 (PGE2). PGE2 is at least in part responsible for the vasodilatation of the afferent arteriole which increases blood flow to the glomerulus; this phenomenon describes why NSAIDs (which inhibit prostaglandin synthesis) result in afferent arteriole vasoconstriction and why NSAIDs can cause a reduced GFR in patients who rely heavily on prostaglandin synthesis to maintain renal blood flow. PGE2 also is known to inhibit ADH-stimulated water permeability in the cortical collecting duct.
There are two isoforms of the cyclo-oxygenase enzyme which converts arachidonic acid to prostaglandin H2: COX-1 (which is the constitutively active “house-keeping” gene present in most cells) and COX-2 (an inducible form of the enzyme which is generally active with inflammation). The COX-2 inhibitors (Vioxx, Celebrex, Bextra) were designed to exploit this, having a greater specificity for inflammation-associated increases in prostaglandins. Interestingly, however, the kidney constitutively expresses COX-2, and therefore COX-2 inhibitors can lead to alterations in renal hemodynamics similar to the NSAIDs.